J Clin Aesthet Dermatol. 2019;12(11):28–31
 by Sherine Hosny Ahmed Abdel Rahman, MD; Mohamed Saber Hussein, MD; and Amira Ibrahim Mansour, MD
by Sherine Hosny Ahmed Abdel Rahman, MD; Mohamed Saber Hussein, MD; and Amira Ibrahim Mansour, MD
Drs. Ahmed, Hussein, and Mansour are with the Faculty of Medicine, Benha University in Banha, Egypt.
FUNDING: No funding was provided for this study.
DISCLOSURES: The authors have no conflicts of interest relevant to the content of this article.
ABSTRACT: Background. Vitiligo is a multifactorial polygenic disorder commonly associated with other autoimmune diseases. The reported link between vitiligo and abnormalities of serum interleukin (IL)-17, zinc, calcium, and vitamin D is not fully understood.
Objectives. We sought to assess the serum levels of vitamin D, calcium, zinc, and IL-17 in patients with vitiligo and to answer the question of whether patients with vitiligo are more prone to experience myocardial infarction.
Design. This was a case-control study and we did not exclude any eligible participants with other systemic autoimmune diseases. Serum vitamin D, calcium, zinc, and IL-17 levels were measured and correlated with disease severity.
Setting. The study was conducted at Benha University Hospital in Egypt.
Participants. Thirty patients with vitiligo and 30 age- and sex-matched healthy volunteers were included.
Measurements. Disease severity was measured using the Vitiligo Extent Tensity Index (VETI) score.
Results.Patients with vitiligo showed significantly lower levels of vitamin D (p<0.001), calcium (p<0.001), and zinc (p<0.001), and an insignificantly higher level of IL-17 compared to the control group (p=0.102). Patients with other autoimmune diseases showed significantly lower vitamin D (p=0.0001) and calcium (p<0.0001) levels and higher IL-17 (p=0.0431) and zinc (p=0.0274) compared to controls.
Conclusion. The levels of measured markers might make patients with vitiligo, especially those with autoimmune diseases, prone to myocardial infarction; the investigation of myocardial infarction, especially when a patient shows low vitamin D, calcium, and zinc or high IL-17 are recommended.
KEYWORDS: Calcium, IL-17, myocardial infarction, vitamin D, vitiligo, zinc ‘
Vitiligo is a multifactorial polygenic disorder with a complex pathogenesis1 and different hypotheses proposed to explain its pathogenesis, including biochemical, oxidant-antioxidant, neural, viral, and autoimmune processes.2 Calcium is defective in the keratinocytes and melanocytes of vitiliginous skin, and decreased intracellular calcium leads to the inhibition of tyrosinase activity and results in the inhibition of melanin synthesis.3 On the subject of vitamin D, in addition to its role in bone formation and calcium metabolism, its receptors are expressed in activated T-cells and dendritic cells.4 Zinc catalyzes the production of 5,6-dihydroxy indole-2-carboxylic acid, enhances the formation of eumelanin polymer,5 and prevents melanocyte apoptosis.6 Interleukin (IL)-17, secreted by T helper 17 cells, is an active participant in melanocyte destruction and the increase of the production of IL-1-beta and tumor necrosis factor-alpha. The IL-17 cytokine expressed in vitiliginous skin7 and its exact role or its receptors in vitiligo are still not fully understood.8 The present study described here aimed to compare levels of vitamin D, calcium, zinc, and IL-17 in patients with vitiligo to those of healthy controls and determine whether patients with vitiligo are more prone to myocardial infarction.
Patients and Methods
This case-control study included 30 patients with vitiligo as the study group and 30 age- and sex-matched healthy volunteers as a control group. This study was approved by the research ethics committee of our institute according to the Declaration of Helsinki. All participants were enrolled from September 1, 2017, to February 28, 2018, recruited during the same season to avoid vitamin D fluctuations. We excluded patients with malabsorption disorders, hepatic or renal diseases, and female patients who were pregnant or lactating. Also, patients receiving systemic steroids, phototherapy, hepatic enzyme inducers, sunscreen, or vitamin supplements three months prior were excluded.
After participants signed an informed consent form, personal history data, including indoor or outdoor occupation, course and duration of vitiligo, presence of systemic autoimmune disease(s), and family history of vitiligo and other autoimmune diseases were collected. Additionally, a complete general and dermatological examination of vitiliginous patches, confirmed by Wood’s lamp in query cases and assessed according to the Vitiligo Extent Tensity Index (VETI),9 was conducted. Then, after fasting for 12 hours, 5mL of venous blood was collected in a plain tube without anticoagulant, left at room temperature for 30 minutes until coagulation, and centrifuged at 1,500 rpm for 15 minutes. The resultant serum was stored at -20°C until analysis. Serum vitamin D and serum IL-17 were measured by using enzyme-linked immunosorbent assay (Shanghai Korain Biotech Co., Shanghai, China). Serum zinc and ionized calcium were measured with the colorimetric method using zinc fluid monoreagent (Centronic GmbH Company, Wartenberg, Germany) and a calcium colorimetric method kit (Shanghai BlueGene Biotech Co., Shanghai, China), respectively. All methods were performed according to the relevant manufacturer’s instructions.
Statistical analysis. Data were collected, revised, coded, and entered into the Statistical Package for the Social Sciences version 20 software program. Quantitative data were analyzed using means and standard deviations, while frequencies and percentages were used when presenting qualitative data. A Student’s t-test was conducted for independent samples, /apthe chi-squared test was used for comparing categorical data, and Spearman’s correlation coefficient was applied to measure the strength of the association between two variables, with p-values of less than 0.05 considered as statistically significant.
Results
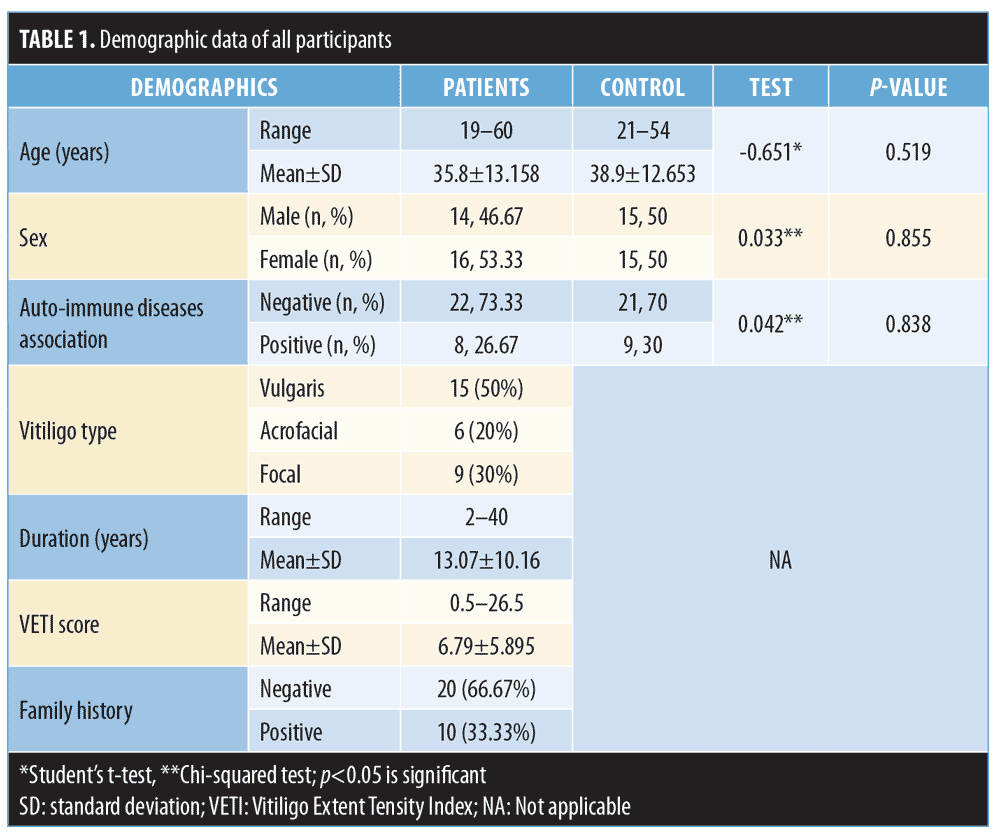
Table 1 presents the demographic data of patients and controls. There were nonsignificant differences between patients and control groups regarding age, sex, and history of autoimmune disease association (p>0.05). Vitiligo duration ranged from 2 to 40 years (mean: 13.07 years), while VETI score ranged from 0.5 to 26.5 points (mean: 6.79 points). The most common type of vitiligo was vulgaris (50%), followed by the focal type (30%), and acrofacial type (20%). Family history and association with other autoimmune diseases were positive in 33.33 percent and 26.67 percent of patients, respectively.
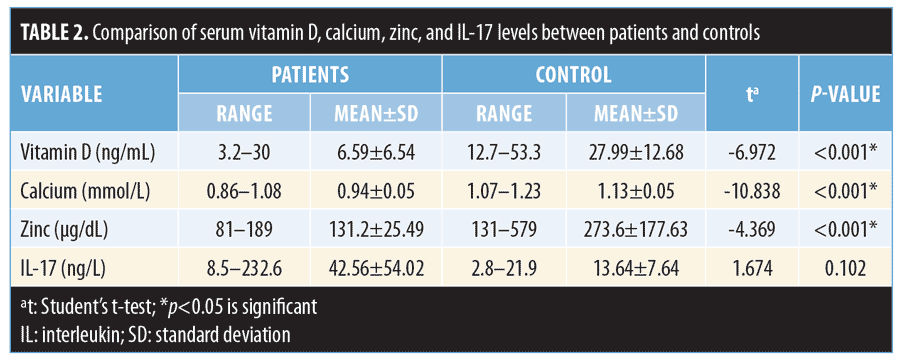
Patients with vitiligo demonstrated significantly lower levels of vitamin D (p<0.001), calcium (p<0.001), and zinc (p<0.001), but an insignificantly higher level of IL-17, compared to the control group (p=0.102) (Table 2). Patients with vitiligo and other autoimmune diseases also showed significantly lower vitamin D (p=0.0001) and calcium (p<0.0001) levels and higher IL-17 (p=0.0431) and zinc (p=0.0274) levels compared to their counterparts in the control group (Table 3).

The duration of vitiligo and VETI score showed a nonsignificant positive correlation with IL-17 and negative nonsignificant correlations with vitamin D, zinc, and calcium (Table 4). Serum calcium level displayed positive significant and insignificant correlations with vitamin D (r=0.686; p<0.001) and zinc (r=0.057; p=0.765) respectively. Meanwhile, negative nonsignificant correlations were found between vitamin D and zinc (r=-0.112; p=0.556) and between IL-17 and calcium (r=-0.159; p=0.401), zinc (r=-0.098; p=0.606), and vitamin D (r=-0.065; p=0.732).

A receiver operating characteristic (ROC) curve showed that the sensitivity results of vitamin D, calcium, zinc, and IL-17 were 83.33, 96.67, 70, and 36.67, respectively, while the specificity results were 100 for vitamin D, calcium, and IL-17 and 90 for zinc, respectively. The cutoff values for vitamin D, calcium, zinc, and IL-17 were 5.8 or less, 1.02 or less, 140 or less, and >21.9 respectively (Table 5).

Discussion
Vitamin D controls cell proliferation and differentiation, exerts immunoregulatory activities, and increases melanogenesis in cultured human melanocytes by way of its antiapoptotic effect.10 In the present study, the mean vitamin D level was significantly lower among patients with vitiligo than controls, which is consistent with other studies.11,12 Moreover, Zhang et al13 revealed a positive correlation between serum D deficiency and vitiligo incidence. On the contrary, Karagün et al14 reported a nonsignificantly lower vitamin D level in patients with vitiligo than in controls.
The IL-17 level was insignificantly higher among patients than controls in the current study, consistent with other studies.15,16 A previous study reported an increased expression of IL-17 in patients with vitiligo compared to controls and a higher expression in active lesions than stable ones.17 However, in another study that excluded patients with vitiligo who presented with other autoimmune diseases, IL-17 levels presented a nonsignificant difference between patients and controls.18
Other reports have suggested similar outcomes to our’s regarding findings of significantly lower calcium19 and zinc20,21 levels in patients with vitiligo compared to controls. Another study22 concluded that the disrupted ultrastructure of the stratum corneum lamellar membranes and disappearance of the calcium gradient coexist in vitiligo lesions, indicating that melanin in the epidermis might play a role in the formation of the epidermal calcium gradient and the maintenance of the structural integrity of the permeability barrier.
Kriegel et al23 pointed to the potential role of vitamin D in autoimmune disease prevention. We found that vitamin D and calcium were significantly lower in patients having other autoimmune diseases versus their counterpart controls, consistent with two previous reports.19,24 Calcium and vitamin D deficits increase the risk of malignancies, chronic inflammatory, and autoimmune diseases (e.g., insulin-dependent diabetes mellitus, inflammatory bowel disease, multiple sclerosis), as well as skeletal disorders.25 What’s more, low levels of ionized serum calcium prolong the ST segment,26 which is one of the earliest myocardial ischemia manifestations.27 Low vitamin D levels have also been associated with cardiovascular disease, including myocardial infarction.28,29 At the same time, the serum calcium level displayed a significant positive correlation with the vitamin D level in our study, boosting the likelihood of myocardial infarction in patients with vitiligo, especially in those with autoimmune disease.
To our knowledge, the higher IL-17 and zinc levels in patients with autoimmune disease versus controls have not been reported before. The pivotal role of IL-17 in the pathogenesis of human systemic and organ-specific autoimmune diseases has been noted in animal and human models.30 Rosenkranz et al31 showed that zinc suppresses T helper 17-mediated autoimmune diseases, reducing their number and proinflammatory cytokine production. Furthermore, Jafarzadeh et al32 reported that ischemic heart disease is associated with higher IL-17 and IL-18 levels. Also, Yesmin et al33 showed that the mean zinc level was significantly decreased in acute myocardial infarction patients compared to controls.
Cardiovascular diseases remain the leading cause of death worldwide and account for most of the premature mortality rates observed among chronic inflammatory diseases. Common mechanisms underlie these two types of disorders.34 Vitiligo was been shown to be significantly correlated with a family history of cardiovascular disease.35 Il-17 was suggested to contribute to the pathogenesis of cardiovascular diseases, including atherosclerosis and myocardial infarction, that occur prematurely in chronic inflammatory disorders.32,36 Moreover, vitiligo associated with other autoimmune conditions was linked to cardiomyopathy28,37 and idiopathic heart block38 in previous reports. Despite accumulating data confirming that patients with vitiligo and autoimmune diseases have a cumulative incidence of risk factors for myocardial infarction, we still lack adequate studies showing the real incidence of myocardial infarction among these patients.
Conclusion
While we acknowledge the small sample size as a limitation of our investigation, our study demonstrated that patients with vitiligo exhibit significantly lower levels of vitamin D, calcium, and zinc, and an insignificantly higher level of IL-17 compared to healthy controls. In patients with autoimmune disease in addition to vitiligo, significantly lower vitamin D and calcium levels and higher IL-17 and zinc levels were observed compared to controls. Certain levels of the present measured markers might make patients with vitiligo, especially those with autoimmune diseases, prone to myocardial infarction. We recommend that patients with vitiligo, especially those with autoimmune diseases, undergo myocardial infarction investigation, especially when they display low levels of vitamin D, calcium, or zinc, or a high IL-17 level. Further studies to detect the incidence of myocardial infarction in patients with vitiligo are warranted.
References
- Malhotra N, Dytoc M. The pathogenesis of vitiligo. J Cutan Med Surg. 2013;17(3):153–172.
- Halder RM, Chappell JL. Vitiligo update. Semin Cutan Med Surg. 2009;28(2):86–92.
- Schallreuter-Wood KU, Pittelkow MR, Swanson NN. Defective calcium transport in vitiliginous melanocytes. Arch Dermatol Res. 1996;288(1): 11–13.
- Ustun I, Seraslan G, Gokce C, et al. Investigation of vitamin D levels in patients with vitiligo vulgaris. Acta Dermatovenerol Croat. 2014;22(2):110–113.
- Cohen BE, Elbuluk N, Mu EW, Orlow SJ. Alternative systemic treatments for vitiligo: a review. Am J Clin Dermatol. 2015;16(6):463–474.
- Bagherani N, Yaghoobi R, Omidian M. Hypothesis: zinc can be effective in treatment of vitiligo. Indian J Dermatol. 2011;56(5):480–484.
- Elela MA, Hegazy RA, Fawzy MM, et al. Interleukin 17, interleukin 22 and FoxP3 expression in tissue and serum of non-segmental vitiligo: a case-controlled study on eighty-four patients. Eur J Dermatol. 2013;23(3):350–355.
- Lukinovic-Skudar, V. Autoimmune factors in the ethiopathogenesis of vitiligo. MOJ Anat Physiol. 2015;1(3): 60–62.
- Feily A. Vitiligo Extent Tensity Index (VETI) score: a new definition, assessment and treatment evaluation criteria in vitiligo. Dermatol Pract Concept. 2014;4(4):81–84.
- Al-Ghamdi K, Kumar A, Moussa N. The role of vitamin D in melanogenesis with an emphasis on vitiligo. Indian J Dermatol Venereol Leprol. 2013;79(6):750–758.
- Sehrawat M, Arora TC, Chauhan A, et al. Correlation of vitamin D levels with pigmentation in patients with vitiligo treated with NBUVB therapy. ISRN Dermatol. 2014;2014:493213.
- Aly D, Mohammed F, Sayed K, et al. Is there a relation between vitamin D and interleukin-17 in vitiligo? A cross-sectional study. Dermatology. 2017;233(6):413–418.
- Zhang JZ, Wang M, Ding Y, et al. Vitamin D receptor gene polymorphism, serum 25-hydroxyvitamin D levels, and risk of vitiligo: A meta-analysis. Medicine (Baltimore). 2018;97(29):e11506.
- Karagün E, Ergin C, Baysak S, et al. The role of serum vitamin D levels in vitiligo. Postepy Dermatol Alergol. 2016;33(4):300–302.
- Bassiouny DA, Shaker O. Role of interleukin-17 in the pathogenesis of vitiligo. Clin Exp Dermatol. 2011;36(3):292–297.
- Khan R, Gupta S, Sharma A. Circulatory levels of T-cell cytokines (interleukin [IL]-2, IL-4, IL-17, and transforming growth factor-beta) in patients with vitiligo. J Am Acad Dermatol. 2012;66(3):510–511.
- Wang LM, Zhang B, Li JJ, et al. The expression change of ROR-gamma-t, BATF, and IL-17 in Chinese patients with vitiligo with 308 nanometers excimer laser treatment. Dermatol Ther. 2018;31(3):e12598.
- Osman AM, Mukhtar MM, Bakheit KH, Hamdan HZ. Plasma Levels of interleukin-17, interleukin-23, and transforming growth factor-beta in Sudanese patients with vitiligo: a case-control study. Indian J Dermatol. 2015;60(6):635.
- Takci Z, Tekin Ö, Ertugru DT, et al. A case-control study: evaluation of vitamin D metabolism in patients with vitiligo. Turk J Med Sci. 2015;45(4):837–841.
- Mogaddam MR, Ardabili NS, Maleki N, et al. Evaluation of the serum zinc level in patients with vitiligo. Postepy Dermatol Alergol. 2017;34(2):116–119.
- Mirnezami M, Rahimi H. Serum zinc level in vitiligo: a case-control study. Indian J Dermatol. 2018;63(3):227–230.
- Liu ZZ, Lei TC. [Ultrastructural changes of epidermal calcium gradient and lipid lamellar membrane in depigmented skin lesions of patients with vitiligo]. Zhonghua Yi Xue Za Zhi. 2016;96(14):1108–1111. Article in Chinese.
- Kriegel MA, Manson JE, Costenbader KH. Does vitamin D affect risk of developing autoimmune disease?: a systematic review. Semin Arthritis Rheum. 2011;40(6):512–531.e8.
- Saleh HM, Abdel Fattah NS, Hamza HT. Evaluation of serum 25-hydroxyvitamin D levels in patients with vitiligo with and without autoimmune diseases. Photodermatol Photoimmunol Photomed. 2013;29(1):34–40.
- Peterlik M, Cross HS. Vitamin D and calcium deficits predispose for multiple chronic diseases. Eur J Clin Invest. 2005;35(5):290–304.
- Gardner JD, Calkins JB Jr, Garrison GE. ECG diagnosis: The effect of ionized serum calcium levels on electrocardiogram. Perm J. 2014;18(1):e119–120.
- Coppola G, Carità P, Corrado E, et al. ST segment elevations: always a marker of acute myocardial infarction?. Indian Heart J. 2013;65(4):412–423.
- Nunes JP, Martins CS. Myocardial infarction, hypovitaminosis D and vitiligo. Rev Port Cardiol. 2010;29(5):839–840.
- Muscogiuri G, Sorice GP, Ajjan R, et al. Can vitamin D deficiency cause diabetes and cardiovascular diseases? Present evidence and future perspectives. Nutr Metab Cardiovasc Dis. 2012;22(2):81–87.
- Tabarkiewicz J, Pogoda K, Karczmarczyk A, et al. The role of IL-17 and Th17 lymphocytes in autoimmune diseases. Arch Immunol Ther Exp (Warsz). 2015;63(6):435–449.
- Rosenkranz E, Maywald M, Hilgers RD, et al. Induction of regulatory T cells in Th1-/Th17-driven experimental autoimmune encephalomyelitis by zinc administration. J Nutr Biochem. 2016;29: 116–123.
- Jafarzadeh A, Esmaeeli-Nadimi A, Nough H, et al. Serum levels of interleukin (IL)-13, IL-17 and IL-18 in patients with ischemic heart disease. Anadolu Kardiyol Derg. 2009;9(2):75–83.
- Yesmin M, Hossain MS, Mia AR, et al. Serum zinc status among acute myocardial infarction male patients in Bangladesh. Mymensingh Med J. 2017;26(1):17-20.
- Robert M, Miossec P. Effects of interleukin 17 on the cardiovascular system. Autoimmun Rev. 2017;16(9):984–991.
- Arunachalam M, Dragoni F, Colucci R, et al. Non-segmental vitiligo and psoriasis comorbidity – a case-control study in Italian patients. J Eur Acad Dermatol Venereol. 2014;28(4):433–437.
- Durante A, Bronzato S. The increased cardiovascular risk in patients affected by autoimmune diseases: review of the various manifestations. J Clin Med Res. 2015;7(6): 379–384.
- Gupta Y, Ammini AC. Vitiligo, hypothyroidism and cardiomyopathy. Indian J Endocrinol Metab. 2012;16(3):463–465.
- Fairfax AJ, Leatham A. Idiopathic heart block: association with vitiligo, thyroid disease, pernicious anaemia, and diabetes mellitus. Br Med J. 1975;4(5992):322–324.
