 J Clin Aesthet Dermatol. 2020;13(12):18–20.
J Clin Aesthet Dermatol. 2020;13(12):18–20.
by Chris G. Adigun, MD, and Hannah Shoaf, MS
Dr. Adigun is with the Dermatology & Laser Center of Chapel Hill in Chapel Hill, North Carolina. Ms. Shoaf is with the Center on Science & Technology Policy at Duke University in Durham, North Carolina.
FUNDING: No funding was provided for this article.
DISCLOSURES: The authors report no conflicts of interest relevant to the content of this article.
ABSTRACT: Multiple cases have reported onychodystrophy secondary to acrylic nails. We present a case of onychodystrophy with psoriasiform nail changes, including onycholysis, splinter hemorrhages, hyperkeratosis, and nail plate thinning, caused by gel manicures. Histopathological analysis of the nail plate and subungual debris revealed neutrophils in the absence of fungal elements. Although the presence of neutrophils in the nail plate material in conjunction with characteristic psoriatic nail changes suggested a diagnosis of psoriasis, certain key features of nail psoriasis, including oil spots, salmon patches, and pitting, were notably absent. The development of these nail changes following gel manicure and pedicure application and the improvement of the onychodystrophy with topical and intralesional steroids support the diagnosis of psoriasiform onychodystrophy.
KEYWORDS: Acrylate, oncyhodystrophy, gel manicure, nail cosmetics, nail psoriasis
The first documented case of nail changes caused by acrylic nails was reported in 1955, when a patient was diagnosed with allergic contact dermatitis (ACD).1 Since the first case of ACD reported by Canizares, the majority of published cases have been a result of the application of sculptured manicures.2–6 Due to the diversity of nail cosmetics that are currently available, a variety of presentations of onychodystrophy can occur, but more recently, there has been an increase in reports of onychodystrophy secondary to photobonded acrylic nails, commonly known as gel manicures, which have become increasingly popular due to their attractive appearance, odorlessness, and durability.7–11 Sculptured nails are traditional powder-applied acrylic nails that polymerize upon combination of the acrylic powder and liquid on top of the nail plate.12 The application process of photobonded gel manicures requires the application of several layers of nail lacquer. First, a base lacquer is applied that contains acrylate monomers and oligomers in addition to the light absorbing activators benzophenone-3 and -4.7,12 The monomers then polymerize with the use of light from either an ultraviolet (UV) lamp or a light-emitting diode (LED) source, causing them to harden.12 Insufficient polymerization of acrylic monomers can lead to sensitization and consequential ACD of the nail unit.13 Furthermore, laboratory investigation using both ultrasound and reflectance confocal microscopy objectively demonstrate decreased nail plate thickness as a direct consequence of gel manicures.8
Several case studies have reported nail changes, such as subungual hyperkeratosis, onycholysis, and periungual dermatitis secondary to the application of artificial nails. In two cases reported by Mendonca et al,7 patients presented with psoriasiform changes in the nail and severe onychodystrophy shortly after receiving gel manicures. Contrary to previous case reports, the patients in Mendonca et al’s case report presented with nail changes in the absence of coinciding periungual dermatitis. Patch testing in some of these cases were subsequently performed to analyze the potential of a contact allergy.2,3,10 One of the most common acrylates that had confirmed allergenicity in the affected patients is 2-hydroxyethyl methacrylate (2-HEMA), which is universally found in the lacquers used in gel nails but inconsistently found in acrylic nails.12 Similar acrylates can be found in dental prostheses, intraocular lenses, and bone cement, among other biomedical products.14 In this report, we present a case of onychodystrophy with psoriasiform changes after a gel manicure and pedicure.
Case Report
A 43-year-old female patient presented with nail changes in her fingernails and toenails. She first noted the changes seven months prior to her initial evaluation after removal of her gel manicures and pedicures. At that time, she presented to her primary care physician (PCP), who then prescribed oral terbinafine. After three months of dosing, she had no improvement in her nails. Subsequently, she was prescribed topical efinaconazole 10% solution and oral itraconazole, of which she also completed three months of dosing without improvement in the condition of her nails. Prior to presenting to her PCP, she had a six-month history of routine gel manicures, with reapplication occurring approximately every 2 to 4 weeks to her fingernails. She continued the applications during the period of her antifungal therapy. Prior to presenting for dermatologic evaluation, she had been receiving application of acrylic gel nails to her fingernails and toenails for the preceding four months, with monthly reapplication. Her most recent removal, one month prior to presentation, revealed very disfigured fingernails and toenails. She complained of moderate pain in her fingers and toes. She denied any joint pain.
On physical examination, the fingernails exhibited distal onycholysis, splinter hemorrhages, notable plate thinning with near anonychia of her left first fingernail, and minimal subungual hyperkeratosis (Figure 1). There was also significant erythema and scaling of the distal digit continuous with the periungual region. Her toenails exhibited onycholysis, pronounced nail plate thickening, subungual hyperkeratosis, with erythema and edema of the periungual skin (Figure 2). There were no other skin findings.
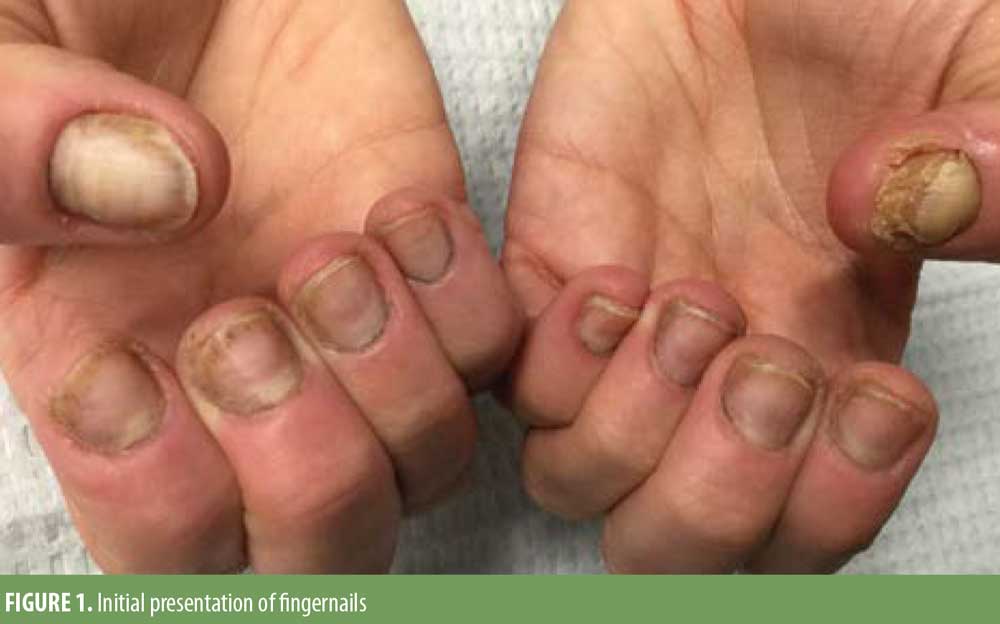
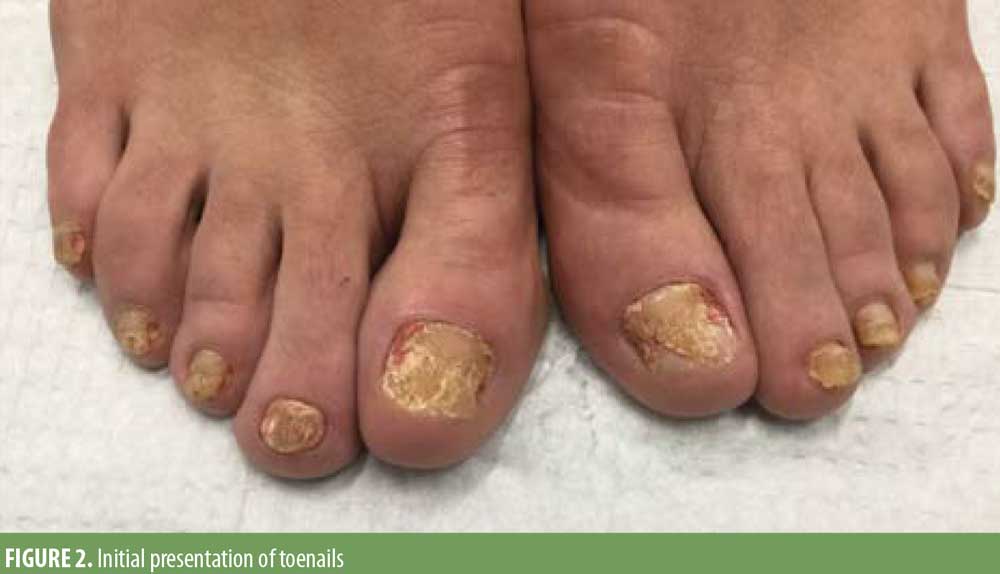
Generous samples were obtained from the right third fingernail and the left first toenail, including both nail plate and subungual debris. These samples were histopathologically analyzed by a dermatopathologist. Samples from both sources exhibited subungual hyperkeratosis with no signs of onychomycosis or infectious etiology. The sample from the left first toenail contained collections of neutrophils within the nail plate.
Given the history of gel manicure and pedicure exposure, the clinical examination, and histopathological findings, a diagnosis of psoriasiform onychodystrophy induced by gel manicure exposure was made. The patient was treated with intralesional triamcinolone 10mg/cc to all 20 digits, which was repeated every six weeks for six months. She was prescribed clobetasol 0.05% ointment, which she used twice daily. Her nails significantly improved over this treatment period (Figures 3 and 4). She had some clinical features of nail psoriasis. However, considering the lack of characteristic clinical findings of psoriasis in the nails or skin and the rapid improvement with topical and intralesional steroids, in conjunction with abstaining from gel manicure exposure, the diagnosis of psoriasiform onychodystrophy caused by components of the gel manicure was favored over psoriasis.
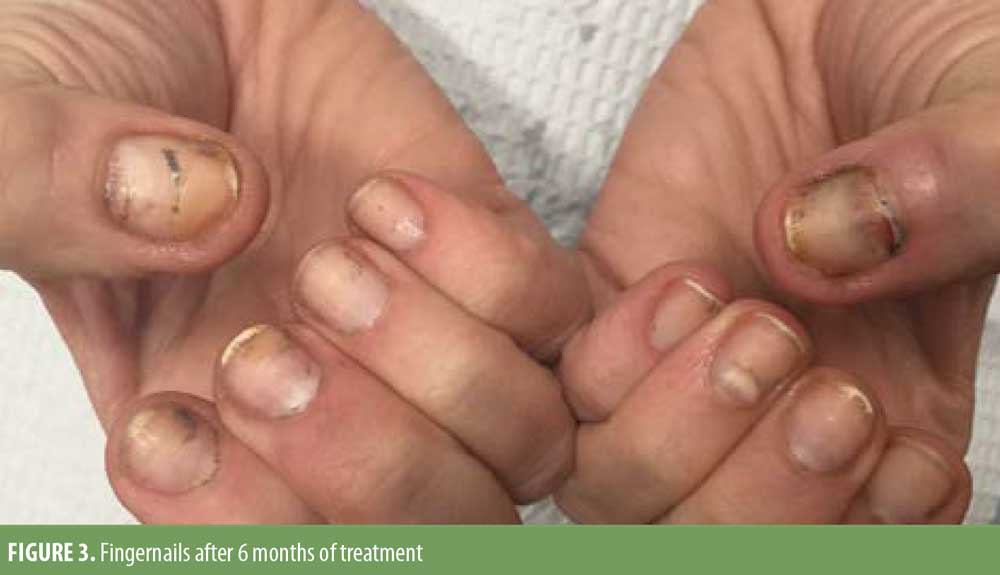
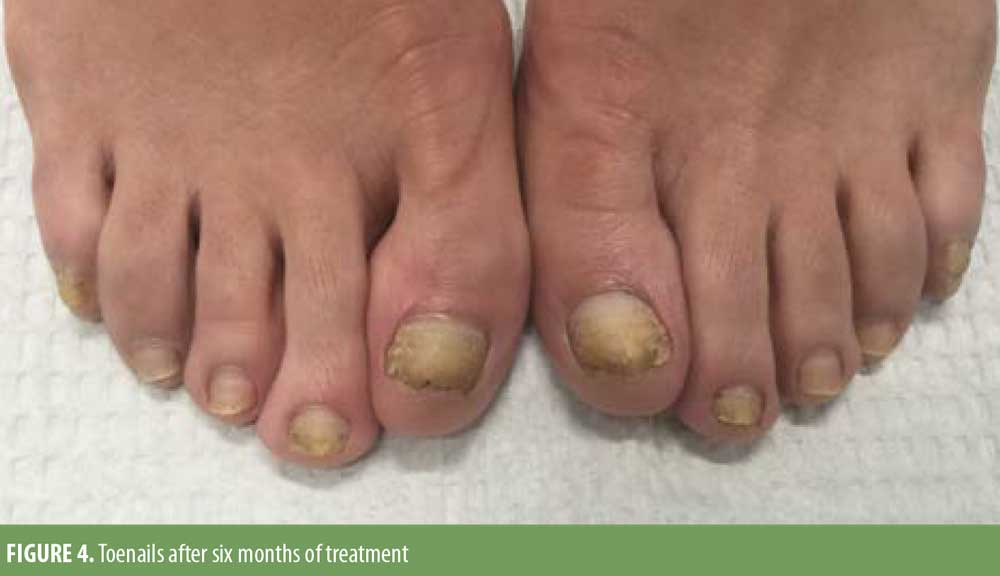
Discussion
Previous cases of nail dystrophy with psoriasiform nail changes have been reported. Mendonca et al7 demonstrated the distinction that in the absence of characteristic nail findings, such as pitting or salmon patches, a clinical diagnosis of psoriasis cannot be made. In a case report by Piraccini et al,15 a patient’s presentation with a similar gel manicure history suggested a diagnosis of psoriasis due to the periungual erythema surrounding the onycholytic area. The authors emphasized the challenge of distinguishing between psoriasis and ACD due to the shared findings of subungual hyperkeratosis and onycholysis. In this case report, the results of histopathological analysis of nail plate and subungual debris were suggestive of psoriasis given the presence of neutrophils within the nail plate in the absence of fungal elements. Although the presence of neutrophils can be suggestive of psoriasis, without characteristic clinical findings in this case it is not diagnostic of psoriasis.16 Consequently, the diagnosis of psoriasiform onychodystrophy was favored.
Given the increase in popularity of gel manicures and pedicures, several recommendations can be made to avoid the complications reported here and elsewhere in the literature. Due to the incidence of sensitization to acrylate monomers, allowing an adequate amount of time for complete polymerization is essential to avoid ACD. Nail technicians who perform manicures using acrylates should use protective gloves, masks, and eyewear to avoid occupational reactions. It is also critical that patients with known acrylate allergies disclose this information to all of their medical providers, including dentists and orthopedists, to avoid a potential reaction in the context outside of nail cosmetics.
Conclusion
We have described one case of psoriasiform onychodystrophy secondary to gel manicure and pedicure application, but given the widespread use of gel manicure products and well-documented reactions to acrylates present in these products, it is likely not an unusual presentation. Although this patient had some clinical and histopathological features of psoriasis, her lack of key clinical findings in concert with her gel manicure history did not fit the clinical diagnosis of psoriasis.
References
- Canizares O. Contact dermatitis due to the acrylic materials used in artificial nails. AMA Arch Derm. 1956;74:141–143.
- Alamri A, Lill D, Summer B, et al. Artificial nail wearing: unexpected elicitor of allergic contact dermatitis, oral lichen planus and risky arthroplasty. Contact Derm. 2019;81:210–211.
- Dekoven S, Holness DL. Contact dermatitis caused by methacrylates in nail products. Can Med Assoc J. 2017;189(37).
- Dickison P, Smith SD. Itching for nail fashion: chronic urticaria and chronic hand dermatitis secondary to acrylate and methacrylate allergy in gel nail varnish. Clin Exp Dermatol. 2017;43(1): 50–53.
- Alcántara-Nicolás FA, Pastor-Nieto MA, Sanchez-Herreros C, et al. Allergic contact dermatitis from acrylic nails in a flamenco guitarist. Occup Med (Lond). 2016;66:751–753.
- Tammaro A, Narcisi A, Abruzzese C, et al. Fingertip dermatitis: a spy for psoriasis. Int Wound J. 2014;13(5):1032–1033.
- Mendonca MMS, Lasenna C, Tosti A. Severe Onychodystrophy due to allergic contact dermatitis from acrylic nails. Skin Appendage Disord. 2015;1(2):91–94.
- Chen AF, Chimento SM, Hu S, et al. Nail damage from gel polish manicure. J Cosmet Dermatol. 2011;11(1):27–29.
- Vázquez-Osorio I, Espasandín-Arias M, García-Gavín J, Fernández-Redondo V. Allergic contact dermatitis due to acrylates in acrylic gel nails: a report of 3 cases. Actas Dermosifiliogr. 2014;105:430–432.
- Cravo M, Cardoso JC, Gonçalo M, Figueiredo A. Allergic contact dermatitis from photobonded acrylic gel nails: a review of four cases. Contact Derm. 2008;59(4):250–251.
- Rieder E, Tosi A. Cosmetically induced disorders of the nail with update on contemporary nail manicures. J Clin Aesthet Dermatol. 2016;9(4): 39–44.
- Constandt L, Hecke EV, Naeyaert J-M, Goossens A. Screening for contact allergy to artificial nails. Contact Derm. 2004;52(2):73–77.
- Lazarov A. Sensitization to acrylates is a common adverse reaction to artificial fingernails. J Eur Acad Dermatol Venereol. 2006;21(2):169–174.
- Gatica-Ortega M-E, Pastor-Nieto M-A, Mercader-García P, Silvestre-Salvador J-F. Allergic contact dermatitis caused by (meth)acrylates in long-lasting nail polish?-?are we facing a new epidemic in the beauty industry? Contact Derm. 2017;77(6):360–366.
- Piraccini BM, Alessandrini A, Magnano M. Psoriasiform nail lesions in a patient with artificial nails. G Ital Dermatol Venereol. 2015;150(6): 761–763.
- Cribier BJ. Psoriasis under the microscope. J Eur Acad Dermatol Venereol. 2006;20(s2):3–9.
