J Clin Aesthet Dermatol. 2025;18(12):42–44.
by Sophie Diong, MB, BCh, BAO; Catriona Gallagher, MD; Julianne Clowry, MD; Alan D. Irvine, MD, DSc; and Maeve A. McAleer, MB, BCh, BAO, PhD
Dr. Diong, Dr. Gallagher, Dr. Clowry, and Dr. McAleer are with the Department of Dermatology at St. James’s Hospital in Dublin, Ireland. Professor Irvine is with the Department of Dermatology at St. James’s Hospital in Dublin, Ireland, and Clinical Medicine at Trinity College Dublin in Dublin, Ireland.
FUNDING: No funding was provided for this article.
DISCLOSURES: The authors have no conflicts of interest relevant to the contents of this article.
ABSTRACT: People with amputations using limb prosthetics commonly develop dermatologic complications, such as impaired skin integrity and folliculitis, at the residuum-prosthesis interface (RPI). Dermatologic complications are the primary cause of dissatisfaction with prosthetics, hindering rehabilitation and leading to prosthesis abandonment. This has a deleterious impact on health-related quality of life (HRQOL). Positive outcomes have been associated with laser hair reduction (LHR) for those with traumatic lower limb amputations; however, this has not been studied in those with upper limb amputations or amputations due to other conditions. We performed a prospective study to assess the effects of skin conditions at the RPI on HRQOL and determine the potential benefit from LHR. Four patients were identified: 75% (n=3) with lower-limb amputations and 25% (n=1) with upper limb amputations. Amputation indications included infection (25%, n=1), congenital malformations (25%, n=1) and trauma (50%, n=2). Participants received 6 sessions of LHR, either alexandrite 755nm alone or in combination with Nd:YAG 1064nm laser. The Skindex-16 survey was performed along with 7 amputee-specific questions. Improvements in HRQOL were seen in all patients and subscales, with an overall average improvement of 50%. Functioning subscale improvement was greatest, at 60%. All patients (100%) were satisfied with LHR treatment. To our knowledge, this is the first study to examine the impact of LHR on the HRQOL of people with upper and lower limb prostheses. LHR is a minimally invasive technique to treat and prevent common dermatologic complications of the RPI, promoting improved self-confidence and prosthesis fit. This study identified an important role for dermatologists to engage with this community to improve their functional capacity and quality of life. Keywords: Laser surgery, amputation, dermatology, medical dermatology, surgical dermatology, quality of life
Introduction
Limb amputation is a significant life event, impacting a person’s quality of life and the ability to perform everyday activities. A prosthesis can radically improve a patient’s function, but it can also lead to complications, thus limiting its usefulness. Approximately ¾ of lower limb prosthesis users experience problems with skin health and integrity after amputation.1
Limb residua are hair-bearing sites that are susceptible to folliculitis, which increases with the sustained use of a prosthesis. Contributory factors include perspiration, localized friction, and hair depilation, which perpetuate a cycle of maceration and skin irritation, forming entry points for microorganisms.1 Underlying indications for amputation include peripheral vascular disease, trauma, and cancer, which may contribute to poor wound healing in these patients at baseline.2 Prosthesis-related skin complications further increase the risk of skin breakdown at the residuum. Prolonged wound healing may prevent the use of a prosthesis for an extended period of time, which can have a profoundly negative impact on patients’ daily functioning and quality of life.
The use of laser hair reduction (LHR) in medical dermatology has expanded in recent years. Although commonly used for aesthetic purposes, LHR has also been used to successfully manage diseases of the hair follicle, such as pilonidal sinus, hidradenitis suppurativa, and dissecting folliculitis.3 Medical therapies often only provide short-lived solutions, as the follicular unit remains intact. Laser-induced damage and epilation of hair follicles offer a more sustained management option for these conditions. LHR offers a minimally invasive technique to treat and prevent common dermatologic complications of the residuum-prosthesis interface (RPI). While positive outcomes have been associated with LHR for those with traumatic lower limb amputations,4 this treatment approach has not been studied in other amputee groups. We sought to investigate the potential benefits of LHR for patients with upper and lower limb amputation secondary to traumatic and nontraumatic causes.
We performed a single-center prospective study to assess the effects of skin conditions at the RPI on health-related quality of life (HRQOL) and to determine the potential benefits from LHR in those with upper or lower limb amputations secondary to either traumatic or nontraumatic causes. Ethical approval was obtained from the local Joint Research Ethics Committee.
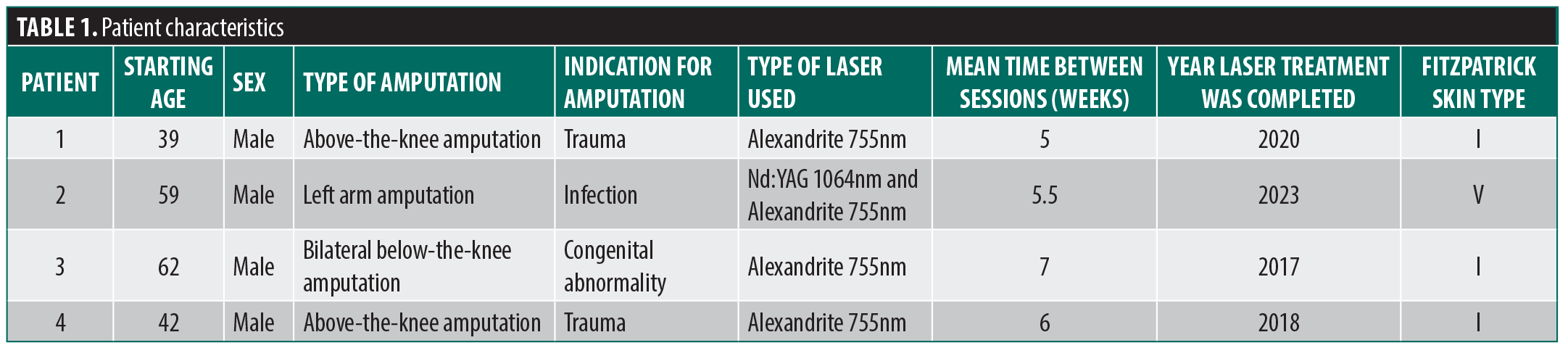
Patients referred for LHR on their residuum were reviewed using the electronic patient record system. Eight patients were identified, of whom 33% (n=3) did not complete their courses and 11% (n=1) could not be contacted. Only those who had completed a course of LHR on their residuum were included. The 4 patients included were male. Three patients had Fitzpatrick skin type I and one patient had Fitzpatrick skin type V. Of these, three had lower limb amputations and one had an upper limb amputation. Indications for amputation included infection (n=1), congenital malformation (n=1), and trauma (n=2). Participants received 6 sessions of LHR, at an average of 6-week intervals. Alexandrite 755nm was used alone or in combination with an Nd:YAG 1064nm laser, depending on the patient’s skin phototype. The patients with Fitzpatrick skin type I were treated with Alexandrite 755nm laser alone due to its high efficacy. The patient with Fitzpatrick skin type V was treated with a combination of Nd:YAG 1064nm and Alexandrite 755nm to maximize efficacy while minimizing potential complications.5 Time from treatment completion to the telephone questionnaire ranged from 6 weeks to 6 years (Table 1).
A telephone interview was conducted to assess improvements in HRQOL following LHR at the residuum. The questionnaires administered were the Skindex-16 survey alongside 7 amputee-specific questions (Table 2).4 The Skindex-16 is a validated model for evaluating the impact of skin conditions on quality of life. It consists of 16 questions scored on a seven-point Likert scale, from 0 (never bothered) to 6 (always bothered). A higher score implies a poorer quality of life.5 A similar adapted version of this questionnaire has been used to evaluate quality of life following LHR of the residuum in patients with amputations secondary to trauma.4
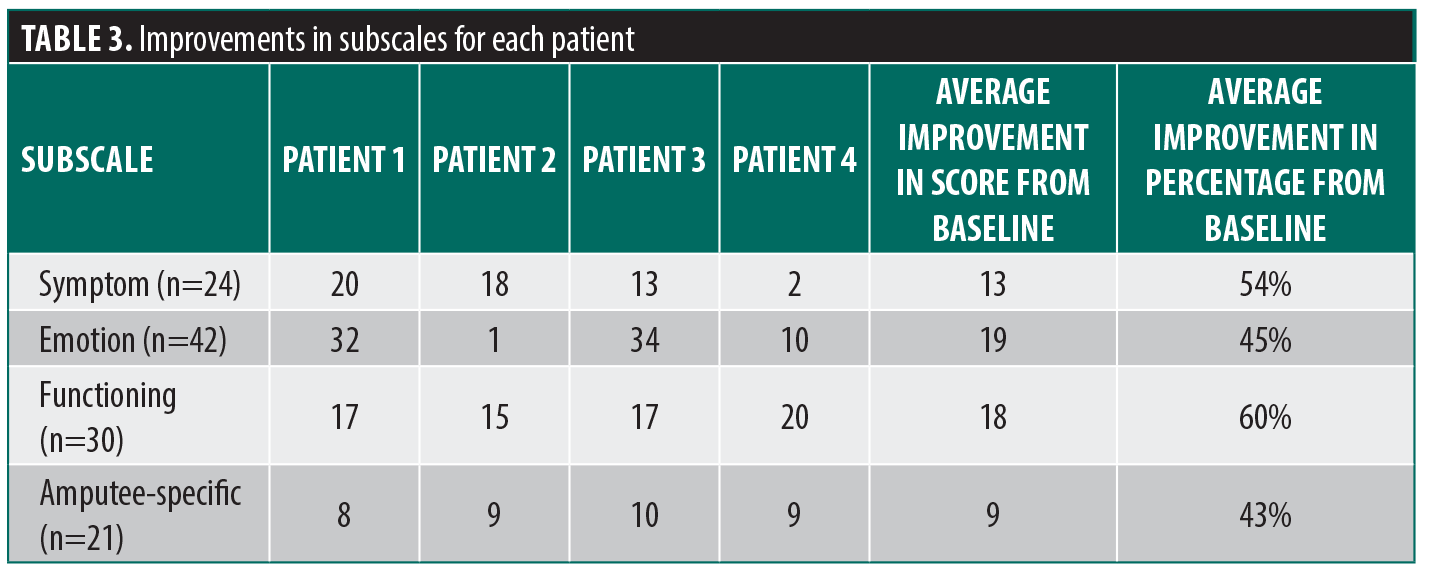
The average adapted Skindex-16 score before LHR was 75 of 117. After 6 sessions of LHR, the average score was reduced to 16 of 117, with an overall average improvement of 59 of 117. The greatest improvement was in the functioning subscale at 60.0%, with an average improvement of 18 of 30. This was followed by an average improvement of 54.2% (13 of 24) in the symptom subscale, 45.2% (19 of 42) in the emotions subscale, and 42.9% (9 of 21) for the amputee-specific subscale (Table 3). All patients (100%) were satisfied with their LHR treatment. No patients reported any severe adverse effects, including thermal burns or scarring.
This is the first study to examine the impact of LHR on the HRQOL of people with upper and lower limb prostheses secondary to traumatic and nontraumatic amputations. To our knowledge, only one previous study has explored LHR in people with amputations, focusing exclusively on traumatic lower limb amputations. In that study, statistically significant improvements in HRQOL were observed across all subscales of the Adapted Skindex-16 after an average of 3 sessions of LHR.4 Similarly, after 6 sessions of LHR, all our patients were satisfied with their treatment and improvements were seen in all subscales of the Adapted Skindex-16 questionnaire. Additionally, no laser-related complications were observed across the two distinct Fitzpatrick skin types studied, representing both lighter and darker phototypes. As LHR is not yet a widely used treatment modality for managing complications at the RPI, further studies are needed to identify ideal protocols.
People with amputations face higher rates of anxiety and depression compared to the general population even 2 years after amputation.6 In our study, the emotion subscale improved by 45%, providing evidence that LHR improves a patient’s outlook and feelings towards their residuum. Symptoms such as irritation and pain associated with the residuum improved by more than 50%. The functioning subscale saw the greatest improvement at 60%. This is a key finding, as a prosthesis may be the first step toward improved engagement in activities of daily living following amputation. Prosthesis usage among those who are unable to walk due to amputation allows independent movement and achieves HRQOL comparable to ambulatory amputees.7 A prosthesis serves not only a functional purpose, but is also a valuable tool in promoting psychological continuity, and facilitating the adaptation and assimilation of new self-representation.8 The amputee-specific subscale improved by 42.9%, highlighting the benefit LHR has on an amputee’s everyday life. Enabling people with amputations to continue comfortable and safe use of their prosthesis is paramount to rehabilitation and restoration of physical and mental health.
The interpretation of these results however should consider the constraints of the study design. The investigation was conducted at a single center with a limited cohort of four male participants, which may reduce external validity. Only two Fitzpatrick skin types were represented, preventing broader conclusions across the full spectrum of phototypes. Additionally, the use of a 23-item questionnaire, while structured, may not capture the full range of quality of life impacts associated with prosthetic residuum skin conditions.
In conclusion, LHR can be a transformative solution for people with amputations seeking to enhance their experience of using a prosthesis, and overall quality of life. By addressing the unique challenges related to hair growth on residual limbs or prosthetic attachment sites, LHR offers those with amputations the opportunity to mitigate potential complications associated with hair growth in these areas. Novel findings in this study include the substantial benefit of LHR for both upper and lower limb amputees secondary to traumatic and nontraumatic causes. While larger studies are required to further characterize ideal therapeutic parameters, this intervention remains a valuable addition to the healthcare and well-being of these individuals. Overall, this study identifies an important role for dermatologists to engage with limb prosthesis users to improve their functional capacity and quality of life.
References
- Ergözen S, Ercan E, Demir Y. Home-applied IPL epilation may prevent the problems due to hair follicle in amputees. Med Hypotheses. 2016;93:53-54.
- Lannan FM, Meyerle JH. The dermatologist’s role in amputee skin care. Cutis. 2019;103(2):86-90.
- Aleem S, Majid I. Unconventional uses of laser hair removal: a review. J Cutan Aesthet Surg. 2019;12(1):8-16.
- Miletta NR, Kim S, Lezanski-Gujda A, Rossi AM, Marquart JD. Improving health-related quality of life in wounded warriors: the promising benefits of laser hair removal to the residual limb-prosthetic interface. Dermatol Surg. 2016;42(10):1182-1187.
- Thomas MM, Houreld NN. The “in’s and outs” of laser hair removal: a mini review. J Cosmet Laser Ther. 2019;21(6):316-322.
- Roșca AC, Baciu CC, Burtăverde V, Mateizer A. Psychological consequences in patients with amputation of a limb: an interpretative-phenomenological analysis. Front Psychol. 2021;12:537493.
- Torbjörnsson E, Ottosson C, Boström L, et al. Health-related quality of life and prosthesis use among patients amputated due to peripheral arterial disease—a one-year follow-up. Disabil Rehabil. 2022;44(10):2149-2157.
- Lundberg M, Hagberg K, Bullington J. My prosthesis as a part of me: a qualitative analysis of living with an osseointegrated prosthetic limb. Prosthet Orthot Int. 2011;35(2):207-214.