 J Clin Aesthet Dermatol. 2023;16(4):38–42.
J Clin Aesthet Dermatol. 2023;16(4):38–42.
by Parvaneh Hatami, MD; Ali Sadeghinia, MD; Hamidreza Mahmoudi, MD; Maryam Daneshpazhooh, MD; Najme Hashemi, MD; Zeinab Aryanian, MD; and Nika Kianfar, MD, MPH
All authors are with Autoimmune Bullous Diseases Research Center, Tehran University of Medical Sciences in Tehran, Iran.
FUNDING: No funding was provided for this article.
DISCLOSURES: The authors report no conflicts of interest relevant to the contents of this article.
ABSTRACT: Background. Despite the emergence of novel medications, poor drug adherence is an obstacle toward disease management in patients with autoimmune bullous dermatoses (AIBDs).
Objectives. We sought to evaluate medication adherence among patients with AIBDs and determine the impact of health literacy on adherence.
Methods. We performed a cross-sectional survey of patients with AIBDs who attended Razi Hospital from May to October 2021. Drug adherence and health literacy were assessed using the Morisky Medication Adherence Scale-8 (MMAS-8; scored 0–8) and Health Literacy for Iranian Adults (HELIA; scored 0–100) questionnaires, respectively. Multivariable ordinal regression, including the covariates age, sex, education level, and annual income, were employed for analyses.
Results. Two hundred participants with a mean±standard deviation (SD) age of 50.3±13.5 years were recruited. The female:male ratio was 1.2. About half (53%) of the patients reported good adherence (MMAS-8 score of 8) to their AIBD medications. Moreover, limited health literacy, with a mean±SD score of 57.8±25.8, was noted. Multivariable ordinal regression indicated that literacy score was significantly associated with good drug adherence (odds ratio [OR]: 0.11 per 1 score of health literacy increase, 95% confidence interval [CI]: 0.09–0.14).
Conclusion. These findings showed suboptimal drug adherence and health literacy of patients with AIBDs. Improving patient health literacy might be a way to increase drug adherence.
Keywords: Adherence, medication adherence, autoimmune bullous disorders, health literacy
Autoimmune bullous dermatoses (AIBDs) are chronic, life-threatening diseases characterized by blisters of the skin and/or mucosa.1 The emergence of systemic corticosteroids has improved the prognosis of the disease. Nevertheless, their unwanted debilitating adverse events are major impediments to disease management, necessitating the use of immunosuppressant agents as steroid-sparing agents or new biologic medications.2
Adherence to treatment regimens is a crucial element of successful disease management. Treatment adherence is defined as the degree to which the patient’s treatment-related behavior is congruent with the physician’s recommendations.3 Numerous related studies assessing various chronic diseases have reported that many patients do not adhere to the prescribed instructions or that adherence may decrease over time.4 Nonadherence can result in disease worsening; poor health outcomes, such as the increased risk of hospitalization and mortality; and, eventually, increased unnecessary healthcare costs.5 Various factors associated with drug adherence have been identified, including demographic factors, financial situation, patient beliefs, and ineffective patient-physician communication.6,7
Health literacy has recently received increasing attention as a substantial predictor of drug adherence.8,9 Health literacy is defined as “the degree to which individuals have the capacity to obtain, process, and understand basic health information and services needed to make appropriate health decisions.”10 This meaning goes beyond the ability to read health-related information and includes effectively implementing the gathered information toward self-care and protection.10,11
The literature regarding the association of health literacy and drug adherence in pemphigus settings is still in its infancy. Therefore, we sought to explore the relationship between health literacy and drug adherence among patients with pemphigus. Moreover, the effect of probable factors on drug adherence was examined.
Methods
Study design and participants. A cross-sectional study was conducted at Razi Hospital, a tertiary care teaching hospital, from May to October 2021. Adult patients with histopathologically confirmed diagnosis of AIBDs attending the dermatology department seeking routine follow-up were recruited. A total of 200 patients consented to enroll during the investigation period and were interviewed by a single, trained investigator. The research was conducted in accordance with the Declaration of Helsinki, and informed consent was obtained from the participants. The Institutional Review Board (IRB) of the Tehran University of Medical Sciences Ethics Committee approved the study (IR.TUMS.MEDICINE.REC.1398.926).
Instruments. The data were collected through three instruments:
- A form containing sociodemographic and disease-related data
- The Persian version of the Morisky Medication Adherence Scale-8 (MMAS-8)12,13
- Health Literacy for Iranian Adults (HELIA)14
- The sociodemographic information of the patients (age, sex, education, annual income, marital status, and health insurance) and disease-related characteristics (type of disease, duration of disease, sites of involvement, comorbidities, drug complications, family history, and previous treatments) were self-reported by patients and completed by referring to their medical records.
The MMAS-8 is one of the most commonly used questionnaires for evaluating patient drug adherence, and its validation has been confirmed. The Persian version of the MMAS-8 was used in the present study. It consists of eight items; seven are recorded in the dichotomous responses as yes/no options, and one is recorded as a 5-point Likert scale response, ranging from 1 (always) to 5 (never).12,13 The scores for the items are categorized into three levels: high adherence (=8), moderate adherence (6–8), and low adherence (<6), as suggested by Morsiky et al.12 In this study, for more precise analysis, individuals with low and moderate adherence were classified as poor adherers, and those with high adherence were classified as good adherers.
The HELIA is a validated and reliable 33-item instrument developed to measure Iranian adults’ health literacy. According to this questionnaire, patients’ final health literacy score was calculated between 0 and 100. The questionnaire offers four health literacy levels by the scores calculated: excellent (>84), adequate (66–84), limited (50-66), and inadequate health literacy (<50).14
Sample size. Considering 95% confidence (0.05 error probability) with a power of 90 percent, the desired precision of 0.1, and the proportion of drug adherence of a previous study equal to 0.5,15 a total of 97 cases were needed. Two hundred cases were considered for enrollment in this study to increase the study’s power.
Statistical analysis. Statistical analysis was performed by IBM Statistical Package for Social Sciences (SPSS) software, version 20.0. Descriptive statistics were expressed as mean with standard deviation (SD) for quantitative variables and as numbers with percentage for qualitative ones. The differences between various levels of drug adherence were investigated employing one-way ANOVA test for quantitative variables and χ2 test for qualitative variables. To evaluate the association of good health literacy and drug adherence, we performed multivariable ordinal regression, including the covariates age, sex, education level, and annual income. P-value less than 0.05 was considered statistically significant.
Results
A total of 200 participants were enrolled in this study. There were 111 (55.5%) female patients and 89 (44.5%) male patients, with a mean age of 50.3±13.5 years. Regarding the disease subtype, 79.5 percent (n=159) of the patients had pemphigus vulgaris, nine percent (n=18) had pemphigus foliaceus, nine percent (n=18) had bullous pemphigoid, and 2.5 percent (n=5) had cicatricial pemphigoid.
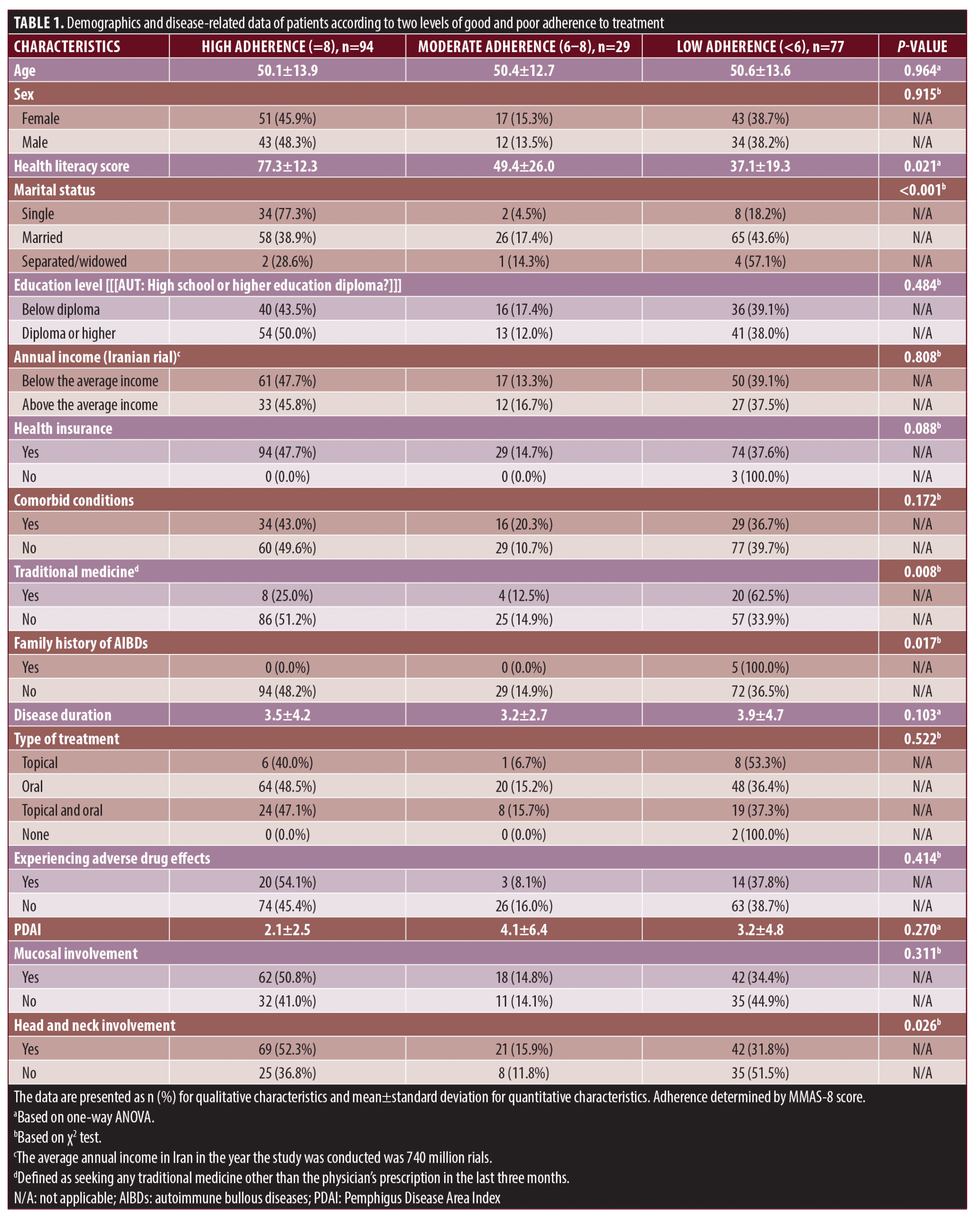
Based on the score of the MMAS-8 questionnaire, 47 percent (n=94) of the subjects were found to have good adherence to AIBD treatment, and the other 53 percent (n=106) had poor adherence. The demographics and disease-related data of the patients in both adherence groups are outlined in Table 1.
The average score of patients’ health literacy according to the HELIA questionnaire was 57.8±25.8. Of the patients, 30 percent (n=60) were categorized as not having adequate health literacy, 23 percent (n=46) as having limited health literacy, 34 percent (n=67) as having adequate health literacy, and 13 percent (n=27) as having excellent health literacy. Figure 1 illustrates the association of each classification of health literacy and drug adherence that emphasizes a better adherence in higher health literacy scores.

In multivariable ordinal regression adjusted for age, sex, education level, and annual income, health literacy score was significantly associated with good drug adherence (odds ratio [OR]: 0.11 per 1 score health literacy increase, 95% confidence interval [CI]: 0.09–0.14).
Discussion
In light of improvements in the treatment of AIBDs, prognosis has dramatically improved; however, patient adherence to AIBD medications is still a matter of great concern. The current study was conducted to investigate the extent of drug adherence and its association with health literacy in patients with AIBDs. The results of this study demonstrated that patients had an average health literacy score of 57.8±25.8, implying a limited health literacy level among patients with AIBDs, according to the HELIA questionnaire.14 Moreover, only half (53%) of the patients had good adherence to their AIBD medications.
Our estimates of adherence to AIBD treatment showed similarities and differences compared to other studies in this field. A study assessing 45 patients with AIBDs that employed a self-made questionnaire with no grading of adherence reported a drug adherence rate of 64 percent.16 Of note, the authors of this study found that relapse was significantly more frequent in nonadherent patients than adherent patients (62.5% vs. 17%).16 Another study, focusing on patients with pemphigus vulgaris, reported an adherence rate of 56 percent, which is in line with our findings.15 However, a recent paper assessing 28 patients with AIBDs reported that most patients (82%) had good adherence to treatment, having never stopped prescribed medications, even at the time of disease remission.4 The discrepancy among the results might be attributed to differences in the method of measuring adherence and the study populations in various regions. It has been well-documented that drug adherence plays a fundamental role in managing chronic disorders, and poor medication adherence can lead to serious health problems.5,17 Moreover, poor drug adherence is considered one of the most common causes of medication failure.18 Thus, identifying the determinants of drug adherence can be the key to better disease management. Accordingly, patients with limited or inadequate health literacy were less likely to have good adherence to their AIBD medications than patients with excellent or adequate health literacy.
The marital status of our patients was another factor associated with drug adherence. Good drug adherence was seen in 77.3 percent of single patients, compared to 38.2 percent of married patients. Considering this information, married patients might be less concerned about their health due to their busy lifestyles and family situations. There are discrepancies regarding the impact of marital status on drug adherence. Some authors have stated that adherence was higher in married patients,19 while others have stated that single patients had higher rates of adherence.20,21 We suppose this matter relies heavily on cultural and socioeconomic factors, leading to inconsistent results among different studies.
Our study results also indicated a significant relationship between seeking traditional medicine and drug adherence, as 75 percent of the patients who sought traditional medicine in the last three months had poor drug adherence. These patients might have little trust in their physician’s instructions, and their false beliefs might cause them to avoid taking the prescribed medications.4
This study detected no significant association between treatment application mode and drug adherence. Nevertheless, topical regimens had a lower adherence rate, compared to oral medications. The effect of treatment application on adherence is important, as treatment of pemphigus mainly relies on oral medications and infusions, while patients with pemphigoid primarily use topical and oral treatments. This finding needs to be further studied by assessing the distribution of different treatments in various AIBDs. In this study, we also found that patients with face and neck involvement had higher adherence levels than those who did not have involvement in these regions. These patients might be greatly worried about their appearance, so they hope to get relief sooner by adhering to medication. Previous research has shown that low adherence highly affects the development of disease- and medication-related complications.6,22,23 Therefore, poor adherence to AIBD medications might be associated with higher disease severity and could accelerate the development of glucocorticoid toxicity, as patients might need to take higher doses of the drug. Moreover, higher hospital admissions, mortality, and healthcare costs would be encountered in the long-term.
Drug adherence is a key point for the proper response to treatment. The best management plan will be doomed to failure if not done correctly. Drug adherence depends on numerous factors, some of which are modifiable, such as health literacy. According to the present study, improving patient awareness of the disease and treatments could increase their adherence to treatment. Therefore, physicians need to spend enough time explaining different aspects of the disease during visits and also provide patients with the necessary information about medication usage and potential side effects. Undoubtedly, patients with low income, low literacy levels, and more severe illnesses need more time and effort in this regard. Forming rehabilitation groups where patients share their experiences with AIBDs might also help increase patients’ health literacy.
Limitations. The authors acknowledge the limitations of the study. The cases were enrolled by convenient sampling from a university hospital, which might not represent the community. The data were gathered through self-report measuring that might bias the results of this study. Moreover, the health literacy measurement tool used in this study was specific to the Iranian population. However, this is one of few articles added to the literature that evaluated the association between health literacy and drug adherence in patients with AIBDs. Further studies from other centers with a wider range of patients are needed to underscore the findings reported here.
Conclusion
The present study showed a limited health literacy of Iranian patients with AIBDs, and that that these patients did not have a good drug adherence rate, which needs improvement. More effective patient-physician communication and disease management would be achieved by identifying factors affecting medication adherence. Dermatologists should also be aware of the relationship between health literacy and drug adherence in patients with AIBDs.
Data availability statement
The data that support the findings of this study are available on request from the corresponding author. The data are not publicly available due to ethical considerations and the privacy of research participants.
References
- Beek NV, Zillikens D, Schmidt E. Bullous autoimmune dermatoses–clinical features, diagnostic evaluation, and treatment options. Dtsch Arztebl Int. 2021;118(24):413–420.
- Mazaherpour E, Kianfar N, Dasdar S, et al. Applicability of glucocorticoid toxicity index in pemphigus: comparison between two groups of rituximab-treated and rituximab-naïve patients. Dermatol Ther. 2022;35(12):e15902.
- Osterberg L, Blaschke T. Adherence to medication. N Engl J Med. 2005;353(5):487–497.
- James J, Sadasivan J, George A. Medication adherence of patients with pemphigus and Bullous pemphigoid disorders in a tertiary care teaching hospital – a prospective-observational study. Indian J Pharm Pract. 2021;14:268–273.
- Roh YH, Koh YD, Noh JH, et al. Effect of health literacy on adherence to osteoporosis treatment among patients with distal radius fracture. Arch Osteoporos. 2017;12(1):42.
- Shi S, Shen Z, Duan Y, et al. Association between medication literacy and medication adherence among patients with hypertension. Front Pharmacol. 2019;10:822.
- Asgari MR, Bouraghi H, Mohammadpour A, et al. The role of psychosocial determinants in predicting adherence to treatment in patient with hypertension. Interv Med Appl Sci. 2019;11(1):8–16.
- Gönderen Çakmak HS, Uncu D. Relationship between health literacy and medication adherence of Turkish cancer patients receiving oral chemotherapy. Asia Pac J Oncol Nurs. 2020;7(4):365–369.
- Dore-Stites D, Lopez MJ, Magee JC, et al. Health literacy and its association with adherence in pediatric liver transplant recipients and their parents. Pediatr Transplant. 2020;24(5):e13726.
- Institute of Medicine (US) Committee on Health Literacy. Health Literacy: A Prescription to End Confusion. Nielsen-Bohlman L, Panzer AM, Kindig DA, eds. National Academies Press (US); 2004.
- Berkman ND, Sheridan SL, Donahue KE, et al, Low health literacy and health outcomes: an updated systematic review. Ann Intern Med. 2011;155(2):97–107.
- Morisky DE, Ang A, Krousel-Wood M, Ward HJ. Predictive validity of a medication adherence measure in an outpatient setting. J Clin Hypertens (Greenwich). 2008;10(5):348–354.
- Moharamzad Y, Saadat H, Nakhjavan Shahraki B, et al. Validation of the Persian version of the 8-Item Morisky Medication Adherence Scale (MMAS-8) in Iranian hypertensive patients. Glob J Health Sci. 2015;7(4):173–183.
- Montazeri A, Tavousi M, Rakhshani F, et al. Health Literacy for Iranian Adults (HELIA): development and psychometric properties. Payesh Health Mon. 2014;13(5):589–599.
- Tirado-Sánchez A, Bonifz A, Ponce-Olivera RM, Espinosa-Díaz S. Prevalence of adherence to dermatological treatments among patients with pemphigus vulgaris and its relationship with complications and death: a single-center, cross-sectional study. Research. 2014;1.
- Kv A, Prathap P, Asokan N. Drug adherence in patients with autoimmune vesiculobullous disorders – a cross sectional study. Int J Dermatol. 2020;59(2):e41–e43.
- Palumbo R. Discussing the effects of poor health literacy on patientsfacing HIV: a narrative literature review. Int J Health Policy Manag. 2015;4(7):417–430.
- Cooper J, Hall L, Penland A, et al. Measuring medication adherence. Popul Health Manag. 2009;12(1):25–30.
- Zaghloul SS, Goodfield MJ. Objective assessment of compliance with psoriasis treatment. Arch Dermatol. 2004;140(4):408–414.
- Gokdemir G, Ari S, Köşlü A. Adherence to treatment in patients with psoriasis vulgaris: Turkish experience. J Eur Acad Dermatol Venereol. 2008;22(3):330–335.
- Mayo-Gamble TL, Mouton C. Examining the Association between health literacy and medication adherence among older adults. Health Commun. 2018;33(9):1124–1130.
- da Rocha MR, dos Santos DS, de Moura KR, et al. Health literacy and adherence to drug treatment of type 2 diabetes mellitus. Escola Anna Nery. 2019;23(2): e2018032.
- Jagadeesan S, Das A, Karunakaran A, et al. A pilot study to evaluate the patient adherence to antifungal therapy in dermatophytosis: a possible contributory factor to the current epidemic-like situation in India. Clin Exp Dermatol. 2022;47(6):1190–1191.
- Baskaradoss JK. Relationship between oral health literacy and oral health status. BMC Oral Health. 2018;18(1):172.
