 Dear Editor:
Dear Editor:
Stenotrophomonas maltophila (S. maltophila) is a Gram-negative bacterium present in most aquatic and humid environments and in soil and plants. This free-living organism exhibits a high degree of resistance to antibiotics and usually goes undetected in routine cultures. S. maltophila is responsible for a range of infections, including respiratory tract infections, bacteremia, endocarditis, and, less commonly, skin and soft-tissue infections.1 S. maltophila is a known nosocomial pathogen and an emerging cause of serious drug-resistant infections. To our knowledge, we present the first report of a case of nail infection caused by S. maltophila.
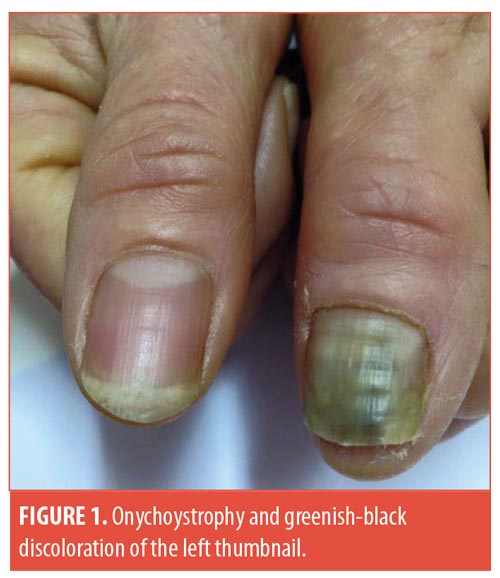 A 60-year-old woman with a past medical history of essential hypertension and type 2 diabetes, treated with telmisartan and metfomin, was referred to our department for onychodystrophy and a greenish-black discoloration of the left thumbnail, which had appeared about six weeks earlier (Figure 1). The patient said that the color changed gradually, and she did not recall any history of trauma nor contact with soil or plants. She did not report pain or other symptoms affecting her nails or fingers. Upon clinical examination, the nail showed signs of onycholysis, including abnormal thickness and dystrophy with a conspicuous, deep black-green discoloration. Onychoscopy revealed irregular black-green discoloration and the presence of a scaly surface. Blood tests were performed for a full blood count, liver function, kidney function, and glycemia; results were all within normal ranges. Nail scrapings were sent off for bacterial and fungal cultures. Fungal identification was negative. However, the bacterial culture confirmed the presence of S. maltophila. Since it is highly unusual to find an infection of S. maltophila in an immunocompetent patient, we opted to repeat the bacterial culture exam; the result was confirmed for a second time. The antibiogram showed sensitivity to ciprofloxacin, so the patient was treated with ciprofloxacin 500mg twice a day for one week. Three weeks after treatment, we noticed a remarkable improvement in the clinical condition.
A 60-year-old woman with a past medical history of essential hypertension and type 2 diabetes, treated with telmisartan and metfomin, was referred to our department for onychodystrophy and a greenish-black discoloration of the left thumbnail, which had appeared about six weeks earlier (Figure 1). The patient said that the color changed gradually, and she did not recall any history of trauma nor contact with soil or plants. She did not report pain or other symptoms affecting her nails or fingers. Upon clinical examination, the nail showed signs of onycholysis, including abnormal thickness and dystrophy with a conspicuous, deep black-green discoloration. Onychoscopy revealed irregular black-green discoloration and the presence of a scaly surface. Blood tests were performed for a full blood count, liver function, kidney function, and glycemia; results were all within normal ranges. Nail scrapings were sent off for bacterial and fungal cultures. Fungal identification was negative. However, the bacterial culture confirmed the presence of S. maltophila. Since it is highly unusual to find an infection of S. maltophila in an immunocompetent patient, we opted to repeat the bacterial culture exam; the result was confirmed for a second time. The antibiogram showed sensitivity to ciprofloxacin, so the patient was treated with ciprofloxacin 500mg twice a day for one week. Three weeks after treatment, we noticed a remarkable improvement in the clinical condition.
Discussion. S. maltophila is a multidrug-resistant, opportunistic, nosocomial pathogen seen most commonly among immunocompromised hosts. The risk factors for S. maltophila infections are well-known and include underlying solid or hematological malignancy, human immunodeficiency virus, organ transplantation, cystic fibrosis, immunosuppressant therapy, prolonged hospitalization, intravenous catheter use, and indwelling catheter (urinary or biliary). S. maltophila is able to form biofilm and colonize humid surfaces; indeed, it has several mechanisms that award it resistance to many antibiotics. This bacterium has been implicated in acute respiratory tract infection, bacteremia, endocarditis, meningitis, ocular infections, enteritis, urinary infection, and skins and soft tissue infections.2,3 Associated skin infections include cellulitis, gangrenous cellulitis, ectyma gangrenosum, metastatic nodular lesions, and infected mucocutaneous ulcer, particularly in immunocompromised individuals. To our knowledge, no cases have been reported in the literature of nail infection from S. maltophila. Worldwide, S. maltophila is an emerging, multidrug-resistant pathogen, and, indeed, the prevalence of these infections in the general population is increasing among immucompetent individuals.4 Management of S. maltophila infections continues to be a challenge due to the limited effective antimicrobial treatment options due to its multifaceted bacterial virulence and extensive resistance to most antibiotics.
With regard,
Alessio Gambardella, MD; Gaetano Licata, MD; and Giuseppe Argenziano, MD
Drs. Gambardella, Licata, and Argenziano are with the Dermatology Unit in the Department of Mental and Physical Health and Preventive Medicine at the University of Campania Luigi Vanvitelli in Naples, Italy.
Disclosures. The authors have no conflicts of interest relevant to the content of this article.
References
- Adegoke A, Stenstrom T, Okoh A. Stenotrophomonas maltophila as an emerging ubiquitous pathogen: looking beyond contemporary antibiotic therapy. Front Microbiol. 2017;8:2276.
- Chang YT, Lin CY, Chen YH, Hsueh PR. Update on infections caused by Stenotrophomonas malthophila with particular attention to resistance mechanisms and therapeutic options. Front Microbiol. 2015;6:893.
- Kash N, Vin H, Danialan R, et al. Stenotrophomonas maltophila with Histopathological features mimicking cutaneous gamma/delta T-cell lymphoma. Int J Infect Dis. 2015;30:7–9.
- Booke JS. Stenotrophomonas maltophila: an emerging global opportunistic pathogen. Clin Microbiol Rev. 2012;25(1):2–41.
