J Clin Aesthet Dermatol. 2026;19(3–4 Suppl 1):S24–S27.
by Arielle Ades, DNP, FNP-BC
Mrs. Ades is with Mandel Dermatology, Boulder, Colorado.
Funding: No funding was provided for this article.
Disclosures: The author has no relevant conflicts of interest.
Background: Acne vulgaris is highly prevalent among young adults and is associated with psychosocial distress, yet the relationship between clinical severity and quality of life (QoL) in this population remains incompletely understood. Objective: To evaluate changes in acne severity and dermatology-related QoL among young adults aged 18 to 22 years and to explore whether improvement in clinical grading corresponds with changes in patient-reported outcomes. Methods: A pre-post observational study was conducted with 16 participants. At baseline (Week 0) and after 8 weeks of treatment, acne severity was assessed using the Global Acne Grading System (GAGS), and QoL was measured with the Dermatology Life Quality Index (DLQI). Descriptive statistics summarized demographic characteristics. Paired t-tests compared pre- and post-treatment scores, and correlation analysis examined the relationship between changes in GAGS and DLQI. Results: Both acne severity and dermatology-related QoL significantly improved over the 8-week treatment period; however, changes in GAGS scores were not significantly correlated with changes in DLQI scores, indicating that perceived QoL improvement did not directly mirror clinical acne improvement. Conclusion: Among young adults with acne, meaningful improvements in both clinical severity and QoL were observed following routine treatment. The lack of correlation between these changes suggests that QoL might be influenced by factors beyond visible lesion reduction, underscoring the importance of incorporating patient-reported outcomes into acne management. Keywords: Acne vulgaris, quality of life, Dermatology Life Quality Index (DLQI), Global Acne Grading System (GAGS), young adults, psychological impact, patient-reported outcomes
Introduction
Acne is one of the most common inflammatory dermatoses treated worldwide.1 Acne vulgaris is a common dermatological condition characterized by the presence of papules, pustules, blackheads, and cysts that primarily affects the face, chest, and back. It results from a complex interaction of excess sebum production, follicular hyperkeratinization, Cutibacterium acnes proliferation, and inflammation.2 A common complication of acne is postinflammatory hyperpigmentation, which can cause additional psychological and social distress.3 Acne is a multifactorial condition influenced by genetics, hormones, and environmental factors.
Acne is one of the most common dermatological conditions affecting young adults. While acne is primarily a physical condition, its effects extend beyond the skin. Acne can significantly impair quality of life (QoL), affecting both physical and psychological wellbeing.4 Skin appearance, especially on the face, can have a significant impact on an individual’s self-esteem and relationships with others and can contribute to overall QoL.3 The chronic and visible nature of acne contributes to psychosocial comorbidities and disturbances in emotional and social functioning.5 Normal healthy skin plays an essential role in maintaining the physical, mental, and social wellbeing of individuals.6 Feeling self-conscious, unattractive to others, and envious of people with clear skin are highly ranked self-reported feelings toward acne.7 Psychiatric comorbidities specifically are well documented among individuals with acne.2 Acne-related pain or scarring can affect daily functioning, further reducing overall QoL.8 Studies have demonstrated elevated rates of depressive symptoms and suicidality among patients with acne compared to other dermatologic conditions.2 Another study concluded that the effects acne has on certain health-related QoL (HRQoL) items are predicting factors on whether a patient will seek dermatological help altogether.9
QoL is a multidimensional construct encompassing physical, psychological, and social wellbeing and is commonly assessed through patient-reported measures. Patient-reported outcome measures are a useful way to capture lived experiences of people living with acne.10 These measures are valuable tools for assessing HRQoL.11 Depression, anxiety, low self-esteem, poor self-image, decreased QoL, and feelings of social isolation can develop in individuals with acne.12 These effects can be compounded by internal and external stressors that are common in young adulthood. Despite being common and medically benign, acne is associated with significant psychological burden and has been linked to systemic comorbidities.13 Although associations between acne and psychological wellbeing have been described, the extent of this relationship among young adults remains unclear.
Young adults, typically defined as individuals aged 18 to 30 years, navigate significant developmental transitions involving independence, identity formation, and social integration. This stage involves ongoing physical, cognitive, emotional, and social development. Young adults might be particularly vulnerable to social pressures and self-image concerns, making it important to understand how acne affects their emotional and psychological wellbeing. Understanding these effects can highlight the importance of timely and effective acne treatment. Although acne is well studied overall, the impact of acne and scarring on QoL in young adults is less clearly defined.14 Longer disease duration has been associated with greater emotional impact.12 Acne can affect emotional wellbeing and act as a barrier to social interactions, contributing to mood disturbances.15 Without a clear understanding of this relationship, healthcare providers might struggle to offer comprehensive treatment approaches that address both the physical and mental aspects of acne. This study aims to evaluate changes in acne severity and QoL among young adults undergoing 8 weeks of acne treatment.
Methods
This study employed a single-group pretest–post-test design to evaluate changes in QoL and acne severity over an 8-week treatment period. Correlational analyses, using the Spearman rank correlation test, were conducted to examine the relationship between acne severity and QoL at baseline, at follow-up, and for changes over time. Participants were recruited by the investigator from a private dermatology practice located in Boulder, Colorado. At the initial visit, patients’ acne was graded using the Global Acne Grading System (GAGS), and they completed the Dermatology Life Quality Index (DLQI) survey. Patients returned 8 weeks later, at which time their acne was graded again using the GAGS, and they completed the DLQI a second time. Pre- and post-treatment results were then compared using paired t-tests and correlation analyses.
The participant population included young adults between the ages of 18 and 22 years who were being treated for acne at a private dermatology practice in Boulder, Colorado. A narrower age range than is typical for young adults (18–30 years) was selected to control variation. Exclusion criteria included individuals who were not patients of the dermatology practice, patients younger than 18 years or older than 22 years, pregnancy or breastfeeding, and any inability to complete the DLQI survey due to language or cognitive barriers. Convenience sampling was used to recruit participants from those presenting to the practice during the study period. At the end of the medical visit, eligible patients were verbally informed about the study by the investigator. The patient was given an iPad, along with their medical record number, to complete the electronic consent form followed by the DLQI. Patients who consented were provided a paper copy of the consent form before leaving the office. The target recruitment goal was approximately 30 participants, depending on eligibility and enrollment during the study period.
The GAGS was used to operationally define acne in this study. The GAGS assigns a numerical severity score based on lesion type and distribution. Scores classify acne as mild, moderate, severe, or very severe.16 Each patient was scored using the GAGS during the initial visit through physical examination. The GAGS is a validated tool for assessing acne severity and is widely used in both clinical research and outpatient dermatology settings.16
To evaluate the psychological effects of acne on the patient population, the DLQI was used to survey each patient at the time of their initial and follow-up visits. Participants completed the DLQI electronically on a provided iPad. QoL was operationally defined and determined through a sum score calculated from the DLQI. The DLQI consists of 10 items assessing symptoms, daily activities, leisure, work or school, personal relationships, and treatment burden.17 After the scores were calculated, interpretations were made based on the sum score for each patient. A sum score of 0 to 1 indicates no effect, 2 to 5 a small effect, 6 to 10 a moderate effect, 11 to 20 a very large effect, and 21 to 30 an extremely large effect. The DLQI is one of the most widely used dermatology-specific instruments. It is a reliable and valid tool to assess patient-perceived impact of skin diseases.17
Data was collected at both the initial and follow-up visits. At the initial visit, participants completed the DLQI survey using a provided iPad. Acne severity was assessed by the provider using the standardized GAGS. This assessment served as the baseline measure. The follow-up visit occurred 8 weeks after the initial visit. Acne severity was assessed at this time by the same provider, and participants again completed the DLQI.
All participants received standard dermatologic care for their acne, which included topical and/or oral treatments, depending on the severity of their condition as determined by the provider. Treatment protocols followed evidence-based dermatologic guidelines, with personalized adjustments made to suit individual patient needs. Specific treatment regimens were not standardized across participants, as the primary focus was on tracking the progression of acne and its impact on QoL.
The primary outcome of interest was the change in QoL, as measured by the DLQI, from the time of the initial visit to the follow-up visit. DLQI and GAGS scores were treated as continuous variables for analysis, consistent with prior research. Paired t-tests were conducted to compare DLQI and GAGS scores at baseline and 8 weeks. A Spearman rank correlation was also used to explain the relationship between the GAGS and DLQI scores at baseline and 8 weeks. Descriptive statistics included age, sex, and race. All descriptive and inferential statistics were computed through SPSS version 31 (IBM Corp.).
This study was conducted in accordance with ethical guidelines for human research. All participants were required to provide informed consent prior to participation. The study was reviewed and approved by the Simmons University Institutional Review Board. Site approval from the participating practice was obtained. Participants were informed that participation was voluntary, would not affect their clinical care, and that all data would remain confidential. No vulnerable populations were involved.
Results
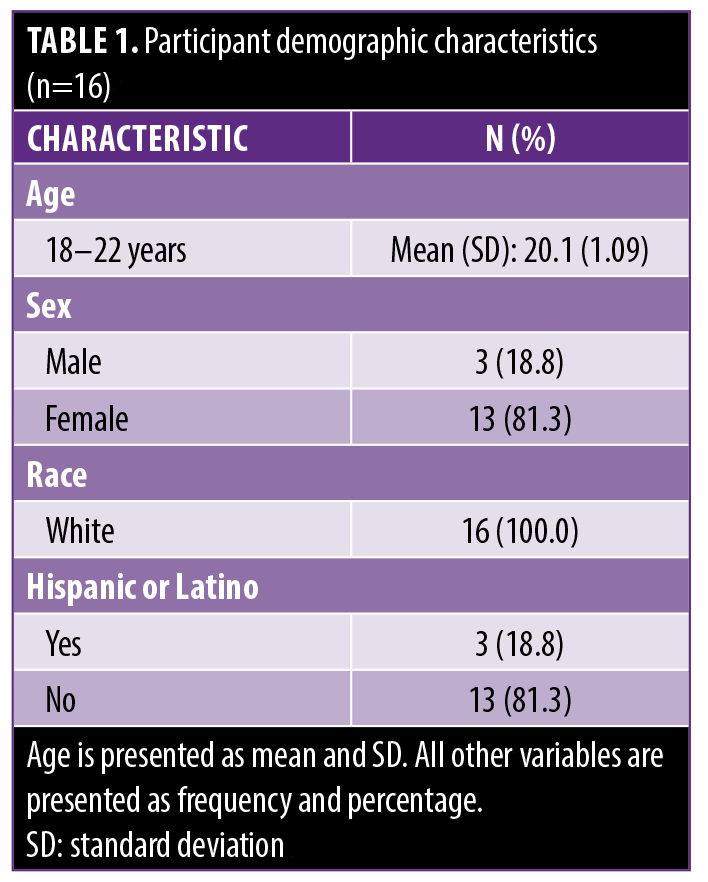
The following results describe changes in acne severity and QoL over an 8-week treatment period. Sixteen participants completed the study. The mean age was 20.1 years (standard deviation [SD]: 1.09; range: 18–22). Most participants were female (81.3%) and White (100%); 18.8% identified as Hispanic or Latino. Participant demographic characteristics are summarized in Table 1.
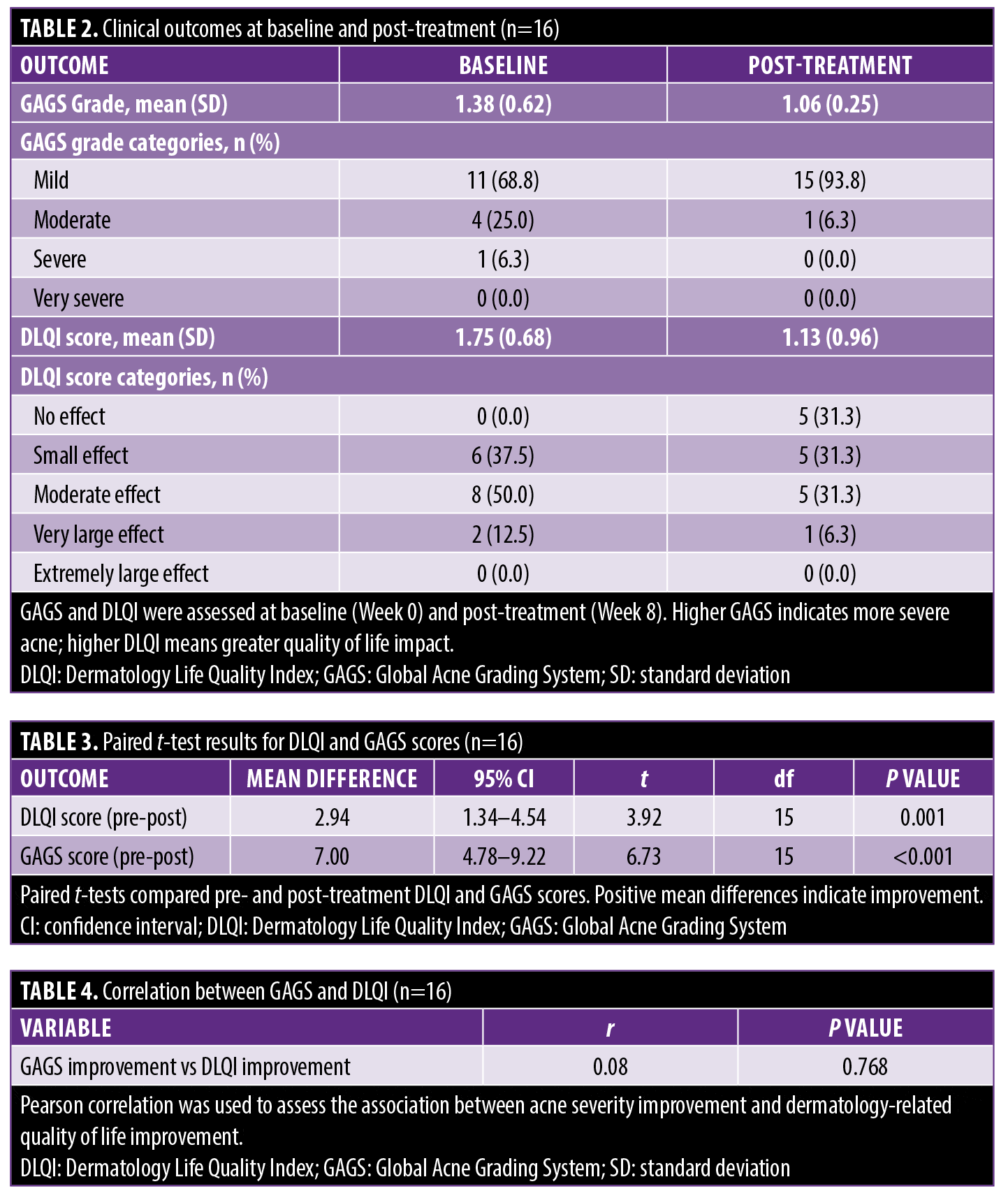
Baseline GAGS grades ranged from mild to severe, with most participants classified as mild (68.8%). After 8 weeks of treatment, 93.8% of participants were classified as mild, and no participants remained in the severe category. Mean GAGS score significantly decreased from baseline (mean: 1.38; SD: 0.62) to post-treatment (mean: 1.06; SD: 0.25), indicating an improvement in acne severity.
At baseline, most participants reported either a small (37.5%) or moderate effect (50.0%) of acne on QoL. After treatment, 31.3% reported no effect, and the proportion reporting a very large effect decreased from 12.5% to 6.3%. Mean DLQI scores also significantly decreased from baseline (mean: 1.75; SD: 0.68) to post-treatment (mean: 1.13; SD: 0.96), indicating improvement in dermatology-related QoL. Clinical outcomes at baseline and post-treatment are presented in Table 2.
Paired t-tests were conducted to evaluate changes in acne severity and dermatology-related QoL from baseline (Week 0) to post-treatment (Week 8). DLQI scores significantly decreased from baseline (mean: 7.00; SD: 3.03) to post-treatment (mean: 4.06; SD: 3.57), with a mean reduction of 2.94 points (95% confidence interval [CI]: 1.34–4.54; t=3.92; df=15; P=0.001). Similarly, GAGS scores significantly decreased from baseline (mean: 16.00; SD: 6.69) to post-treatment (mean: 9.00; SD: 5.11). The mean reduction was 7.00 points (95% CI: 4.78–9.22; t=6.73; df=15; P<0.001), indicating substantial improvement in acne severity following treatment. Paired t-test results are presented in Table 3.
A Pearson correlation was conducted to examine whether improvement in acne severity was associated with improvement in dermatology-related QoL. There were no significant changes in GAGS and DLQI (r=0.08, P=0.768), indicating that reductions in acne severity did not correspond to proportional changes in QoL. Pearson correlation results are presented in Table 4.
Discussion
This study evaluated changes in acne severity and dermatology-related QoL among young adults undergoing 8 weeks of acne treatment. Both acne severity and QoL significantly improved from baseline to follow-up, indicating that the treatment period was associated with meaningful clinical and patient-reported benefits. Changes in acne severity were not significantly correlated with changes in QoL, suggesting that improvements in perceived wellbeing might not directly mirror clinical improvements in acne.
The significant reduction in GAGS scores aligns with expected clinical improvement following dermatologic treatment, particularly given that all participants received evidence-based acne management. Improvements in DLQI scores indicate that even modest clinical improvement might translate into perceived enhancement in daily functioning and emotional wellbeing. The absence of a correlation between acne severity and QoL improvement suggests that QoL might be influenced by factors beyond visible acne alone. Young adults might respond more strongly to subjective improvements, reassurance from clinical care, or psychosocial support rather than only lesion reduction. This distinction highlights the multidimensional nature of acne’s impact and suggests that treatment success might not be captured fully by clinical grading alone.
These findings are consistent with prior studies showing that acne negatively affects emotional wellbeing, self-esteem, and social function among adolescents and young adults. Several studies have demonstrated that even mild acne can greatly impact perceived QoL, while other research has reported that acne severity does not always correlate with QoL scores. This pattern aligns with the present study, in which QoL improved over time but was not directly associated with changes in GAGS scores. Other research has similarly suggested that psychosocial factors, such as embarrassment, social avoidance, and peer comparison, might influence QoL independently of clinical severity. In this context, the present findings reinforce the importance of evaluating both objective and patient-reported measures in acne care.
The lack of association between acne severity and QoL improvement was an unexpected finding, particularly given the significant reduction in both measures. Several explanations could account for this discrepancy. Young adults might experience heightened psychosocial sensitivity to acne because of developmental factors related to identity formation, peer comparison, and social engagement. Additionally, QoL improvements might result from reassurance, regular follow-up, or perceived support rather than from changes in lesion count alone. Finally, individual differences in coping strategies or self-perception might influence QoL outcomes independently of measured acne severity.
Limitations. This study had several limitations. The small sample size and convenience sampling from a single dermatology practice limit generalizability, particularly given the lack of racial diversity in the sample. A notable limitation was the difficulty obtaining follow-up visits, resulting in a smaller final sample and potential response bias among those who returned. Treatment regimens were not standardized, which might have introduced variability in clinical outcomes. Additionally, the DLQI is a self-reported measure and could be influenced by factors outside of acne severity. These limitations should be considered when interpreting the findings.
Conclusion
The findings from this study highlight the importance of addressing both clinical severity and patient-perceived impact when treating acne in young adults. Since QoL does not consistently improve in parallel with acne severity, dermatology providers should consider incorporating routine psychosocial assessment and patient-reported measures into acne care. Early and effective treatment might prevent not only physical progression, but also emotional distress, and discussions about expectations and coping strategies can be beneficial. These results support a holistic, patient-centered approach to acne management.
Future research should examine these relationships in larger and more diverse populations and use standardized treatment protocols. Longitudinal studies with longer follow-up periods could clarify how acne severity and quality of life change over time. Qualitative research could provide deeper insight into how young adults interpret and cope with acne beyond clinical severity. Further work is warranted to explore which psychosocial factors mediate QoL improvements during acne treatment.
References
- Smith H, Layton AM, Thiboutot D, et al. Identifying the impacts of acne and the use of questionnaires to detect these impacts: a systematic literature review. Am J Clin Dermatol. 2021;22(2):159–171.
- Cengiz GF, Gürel G. Difficulties in emotion regulation and quality of life in patients with acne. Qual Life Res. 2020;29(2):431–438.
- Darji K, Varade R, West D, et al. Psychosocial impact of postinflammatory hyperpigmentation in patients with acne vulgaris. J Clin Aesthet Dermatol. 2017;10(5):18–23.
- Marron SE, Chernyshov PV, Tomas-Aragones L. Quality-of-life research in acne vulgaris: current status and future directions. Am J Clin Dermatol. 2019;20(4):527–538.
- Lenczowski E, Pappo Lake E. More than skin deep. J Dermatol Nurses Assoc. 2018;10(1S):S23–S24.
- Salman A, Kurt E, Topcuoglu V, Demircay Z. Social anxiety and quality of life in vitiligo and acne patients with facial involvement: a cross-sectional controlled study. Am J Clin Dermatol. 2016;17(3):305–311.
- Tan J, Frey MP, Thiboutot D, et al. Identifying the impacts of acne: a Delphi survey of patients and clinicians. J Cutan Med Surg. 2020;24(3):259–266.
- Tan J, Beissert S, Cook-Bolden F, et al. Impact of facial atrophic acne scars on quality of life: a multi-country population-based survey. Am J Clin Dermatol. 2022;23(1):115–123.
- Chernyshov PV, Petrenko A, Kopylova V. What health-related quality of life factors influence the decision of patients with acne to visit a dermatologist? J Clin Aesthet Dermatol. 2018;11(7):21–25.
- Yoon J, Homsi HA, Barbieri JS. Analysis of content and phrasing of health-related quality-of-life patient-reported outcome measures used in patients with acne. JAMA Dermatol. 2022;158(9):1072.
- Hopkins ZH, Thiboutot D, Homsi HA, et al. Patient-reported outcome measures for health-related quality of life in patients with acne vulgaris. JAMA Dermatol. 2022;158(8):900–911.
- Hazarika N, Archana M. The psychosocial impact of acne vulgaris. Indian J Dermatol. 2016;61(5):515–520.
- Stamu‐O’Brien C, Jafferany M, Carniciu S, Abdelmaksoud A. Psychodermatology of acne: psychological aspects and effects of acne vulgaris. J Cosmet Dermatol. 2020;20(4):1082–1090.
- Tan J, Beissert S, Cook-Bolden F, et al. Evaluation of psychological well-being and social impact of atrophic acne scarring: a multinational, mixed-methods study. JAAD Int. 2022;6:43–50.
- Kostecka M, Kostecka J, Szwed-Gułaga O, et al. The impact of common acne on the well-being of young people aged 15-35 years and the influence of nutrition knowledge and diet on acne development. Nutrients. 2022;14(24):5293.
- Doshi A, Zaheer A, Stiller MJ. A comparison of current acne grading systems and proposal of a novel system. Int J Dermatol. 1997;36(6):416–418.
- Basra MKA, Fenech R, Gatt RM, et al. The Dermatology Life Quality Index 1994-2007: a comprehensive review of validation data and clinical results. Br J Dermatol. 2008;159(5):997–1035.