J Clin Aesthet Dermatol. 2021;14(11):41–43.
by Chandrashekar BS, MD, DNB; Sree Lalitha Vadlamudi, DDVL, FRGUHS; and Chaithra Shenoy, MD, FRGUHS
All authors are with the Academy of Cutaneous Science in Bangalore, India.
FUNDING: No funding was provided for this article.
DISCLOSURES: The authors report no conflicts of interest relevant to the content of this article.
ABSTRACT: Background. Chemical peels are an integral part of dermatology practice for the treatment of acne, photoaging, and pigmentary dyschromias. Oral isotretinoin is considered the gold standard in the management of acne. Combining both is not currently recommended, due to the increased risk of complications like dryness, erythema, post-inflammatory hyperpigmentation, and scarring.
Objective. We sought to assess the safety and efficacy of superficial chemical peels in patients with acne taking isotretinoin and those not taking oral isotretinoin.
Methods. A comparative, retrospective analysis of three superficial chemical peels was performed; the analysis included 60 patients and 214 sessions that took place between August 2017 and January 2018. Of these, 47 patients were on oral isotretinoin (Group A) and 13 were not on isotretinoin (Group B). In Group A, a salicylic acid-mandelic acid peel (SMP) was performed on 22 patients, a glycolic acid peel was performed on 18 patients, and a modified Jessner’s peel was performed on seven patients. In Group B, an SMP on eight, glycolic acid peel on four, and modified Jessner’s peel on one patient(s), respectively, were performed. Complications, if any, were noted, and incidence rates were compared by photographic assessment.
Results. One patient in Group A and one patient in Group B had complications (persistent hyperpigmentation). The difference in the incidence of complications was insignificant between the two groups for all three superficial peels. Furthermore, it was noticed that patients in the isotretinoin group experienced faster and better improvement compared to those in the non-isotretinoin group.
Conclusion. In our study, the use of isotretinoin did not result in any complications; hence, we encourage combination therapy to achieve enhanced and faster resolution of acne.
Keywords: Chemical peel, acne, isotretinoin
Acne is a disorder of pilosebaceous units. It is a self-limiting disease, yet can lead to disfiguring scars and pigmentary alterations. Oral isotretinoin has been extensively used in the medical management of acne vulgaris in the past decade.2–4 Given at a dose of 0.5 to 2 mg/kg body weight,5 the molecule has a significant sebosuppressive effect. Moreover, the combination of low-dose oral isotretinoin along with superficial chemical peeling (CP) with beta-hydroxy acid, has been shown to be more beneficial.6 Superficial CP has not shown any adverse effects, unlike medium to deep CP, which has been associated with adverse effects, such as delayed wound healing and increased incidence of scarring when combined with systemic isotretinoin.6–10 We conducted this study to compare the safety of chemical peels for acne vulgaris and acne-induced pigmentation in patients on oral isotretinoin versus patients not on oral isotretinoin.
Methods
A comparative, single-center retrospective analysis was performed and included patients who had undergone one of three types of superficial chemical peels—salicylic acid-mandelic acid peel, modified Jessner’s peel, and glycolic acid peel—between August 2017 and January 2018.
Sixty patients aged 15 to 45 years who were treated with superficial chemical peel for acne and acne-induced pigmentation were included in the study. Two groups were created based on the use of oral isotretinoin or lack thereof. Group A included 47 patients receiving 0.5mg/kg per day of oral isotretinoin combined with topical treatment. Group B included 13 patients who were on topical treatment only. Topical treatment included antibiotics, benzoyl peroxide, and retinoids. A total of 214 sessions of chemical peels were done (i.e., 3 to 4 sessions of each peel). In Group A, a salicylic acid (20%)-mandelic acid (20%) peel (SMP) was performed on 22 patients, a glycolic acid (20%, 35%) peel was performed on 18 patients, and a modified Jessner’s peel (three coats) was performed on seven patients. In Group B, a SMP on eight, a glycolic acid (20%, 35%) peel on four, and modified Jessner’s peel (three coats) on one patient(s), were performed. Complications, if any, were noted for each patient, and incidence rates were compared by photographic assessment.
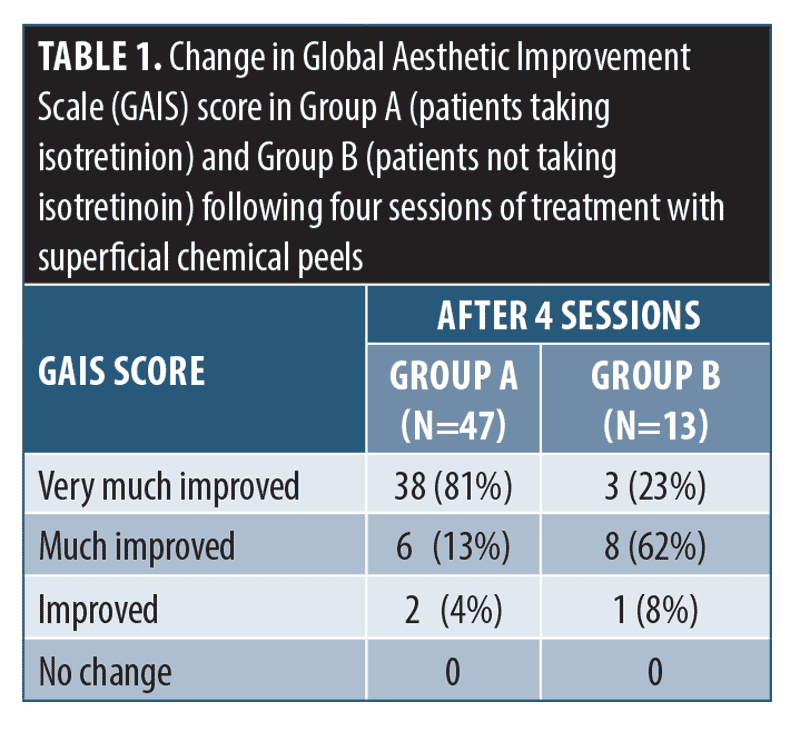
Assessment. Photographs were taken at baseline before each session, and at the end of four sessions (Figures 1 and 2). A subjective assessment of photographs was done by a single physician. These were assessed clinically for erythema, dryness, pigmentary changes, and allergic reactions at the end of each session. The improvement was scored using Global Aesthetic Improvement Scale (GAIS) (Table 1).


Results
Of 60 patients, there were 41 women and 19 men. The study participants were aged 15 to 40 years, with a mean age of 27.5 years. Transient erythema, which subsided within a few minutes, was seen in 12 patients (8 from Group A and 2 from Group B). Only two patients experienced persistent hyperpigmentation (>2 weeks), including one patient from Group A following SMP and one patient from Group B following glycolic acid (35%) peel, which is insignificant. Visible desquamation was seen with glycolic mandelic acid peels in eight patients belonging to Group A and two patients belonging to Group B.
Dryness or burning/stinging sensations were not present in any patient of either group. Clinically, a significant reduction in acne and acne-induced pigmentation was observed in both the groups after four sessions. Patients in Group A had faster improvement compared to Group B based on GAIS scores (Table 1).
Discussion
Isotretinoin is the only treatment that acts on all major factors that are involved in the etiology of acne. It influences the progression of cell cycle, cellular differentiation, cell survival, and apoptosis.11 It reduces the sebum production significantly, influences comedogenesis, reduces the surface and ductal propionibacterium acnes, and also exerts anti-inflammatory action. A significant reduction in sebum production occurs at a dose of 0.5 to 1.0 mg/kg/day within six weeks.
Chemical peeling is an outpatient cosmetic procedure, which is minimally invasive and commonly used for the treatment of conditions like acne, photoaging, and pigmentary disorders.
The salicylic acid peel, a beta-hydroxy acid peel, has a potent sebosuppressive effect along with both keratolytic properties and anti-inflammatory properties; it infiltrates into pilosebaceous layers, showing a self-neutralizing capability with minimal dermal infiltration, and assists in faster resolution of acne with minimal scarring and post-inflammatory hyperpigmentation.1
Glycolic acid is an beta-hydroxy acid. Chemical peel with glycolic acid has shown only transient adverse effects, like burning sensation or erythema and moderate pain, which are considered to be minor.12
According to the standard guidelines, performing procedures in patients who are currently on oral isotretinoin or those who have recently completed the treatment with oral isotretinoin is unsafe. It is recommended to discontinue isotretinoin six months prior to performing cosmetic procedures, as it may lead to hypertrophic scarring and keloid formation by delaying wound healing.13 However, these adverse effects are associated only with isotretinoin when combined with medium to deep CP and not with the superficial CP, which is safer, only causing adverse effects such as erythema and mild hyperpigmentation that are transient and neglible.12
Many studies have reported favorable results in patients who underwent chemical peel while taking oral isotretinoin. Two cohort studies performing chemical peel using trichloroacetic acid 35% (10 patients) and sequential salicylic acid 20% peels (30 patients) done every two weeks for 16 weeks resulted in desired cosmetic outcomes in combination with isotretinoin use, without adverse effects on wound healing.1,14 Forty-five resorcinol peels done on 20 patients who were simultaneously being treated with low-dose isotretinoin showed cosmetic improvement of aging in a manner that was statistically significant compared to in patients not on oral isotretinoin.6
In another study, 60 consecutive patients were randomized and administered either oral isotretinoin (20 mg/d) alone for 16 weeks or oral isotretinoin (20 mg/d) together with 20% salicylic acid peels every two weeks for 16 weeks for moderate to severe facial acne. Better efficacy was seen with combination treatment of isotretinoin and peel. There were no adverse events of scarring or delayed wound healing in either treatment arm.11
In our study, in Group A, all patients were started on 10 to 20 mg of isotretinoin once daily along with chemical peels done at intervals of two to three weeks. In Group B , superficial CPs were done at intervals of two to three weeks and they were not on oral isotretinoin. Visible desquamation was seen with glycolic and mandelic acid peels in eight patients belonging to Group A and two patients belonging to Group B. A large majority of patients did not develop any side effect due to peeling; visible desquamation was seen with glycolic acid peel but not the other two peel types. Dryness was seen more often with SMPs (13.3%) and transient erythema in 15% was seen with both SMP and GA peels. There was no significant statistical difference in these changes in either of the groups.
Persistent hyperpigmentation was observed in one of 47 patients belonging to the group receiving isotretinoin and in one of 13 patients who were not receiving isotretinoin, which is insignificant. This would have occurred as a result of either poor sun protection or non-adherence to topical medication following the peel. The reversible transient side effect was erythema. Isotretinoin patients did not have increased side effects compared to those not on isotretinoin, including excessive dryness or burning and pigmentary alterations, as believed earlier; neither was there any evidence of delayed healing.
Conclusion
Chemical peels along with oral isotretinoin treatment can be performed and appear to be safe. In our study, there were no significant persistent complications and there appeared to be a better outcome with isotretinoin. Nevertheless, more trials and studies are necessary to ascertain that better results in patients taking isotretinoin may be achieved. If this is successfully demonstrated, administration of isotretinoin in higher doses can also be considered in the future.
References
- Kar BR, Tripathy S, Panda M. Comparative study of oral isotretinoin versus oral isotretinoin + 20% salicylic acid peel in the treatment of active acne. J Cutan Aesthet Surg. 20a13;6(4):204–208.
- Ellis CN, Krach KJ. Uses and complications ofisotretinoin therapy. J Am Acad Dermatol. 2001;45(5):S150–S157.
- Kalil CL, Fachinello FZ, Lamb FM, Comunello LN. Use of oral isotretinoin in photoaging therapy. Skinmed. 2008;7(10:10–14.
- Rabello-Fonseca RM, Azulay DR, Luiz RR, et al. Oral isotretinoin in photoaging: clinical and histopathological evidence of efficacy of an off-label indication. J Eur Acad Dermatol Venereol. 2009;23(2):115–123.
- Rathi SK. Acne vulgaris treatment: the current scenario. Indian J Dermatol. 2011;56(1):7–13.
- Hernandez-Perez E, Khawaja HA, Alvarez TY. Oral isotretinoin as part of the treatment of cutaneous aging. Dermatol Surg. 2000;26(7):649–652.
- Obagi ZE, Alaiti S, Obagi S, et al. Standardizing the evaluation of treatment outcomes after skin rejuvenation: the qualitative scoring system. Aesthetic Plast Surg. 2000;24(3):165–170.
- Rubenstein R, Roenigk HH Jr., Stegman SJ, Hanke CW. Atypical keloids after dermabrasion of patients taking isotretinoin. J Am AcadDermatol. 1986;15(2 Pt 1):280–285.
- Duffy DM. Avoiding complications with chemical peels. In: Rubin MG. Chemical Peels (Procedures in Cosmetic Dermatology series). Amsterdam, the Netherlands: Elsevier; 2006: 137–170.
- Zhang AY, Obagi S: Diagnosis and management of skin resurfacing related complications. Oral Maxillofac Surg Clin North Am. 2009;21(1):1–12, v.
- Layton A. The use of isotretinoin in acne. Dermatoendocrinol. 2009;1(3):162–169.
- Gerber PA, Kukova G, Bölke E, et al. Severe hyperpigmentation and scarring following glycolic acid peel treatment in combination with low-dose isotretinoin. Eur J Med Res. 2014;19(1):60.
- Mysore V, Mahadevappa OH, Barua S, et al. Standard guidelines of care: Performing procedures in patients on or recently administered with isotretinoin. J Cutan Aesthet Surg. 2017;10(4):186–194.
- Picosse FR, Yarak S, Cabral NC, Bagatin E. Early chemabrasion for acne scars after treatment with oral isotretinoin. Dermatol Surg. 2012;38(9):1521–1526.
- Mahadevappa OH, Mysore V, Viswanath V, et al. Surgical outcome in patients taking concomitant or ecent intake of oral isotretinoin: a multicentric study-ISO-AIMS study. J Cutan Aesthet Surg. 2016;9(2):106–114.
