J Clin Aesthet Dermatol. 2026;19(2):55–57.
by Zane Sejdiu, BS; Romina Garakani, BS; Stephen Ansah-Addo, MD; Kelly McCoy, MD; Farhaan Hafeez, MD; and Andrew C. Krakowski, MD
Mr. Sejdiu and Ms. Garakani are with the Drexel University College of Medicine in Philadelphia, Pennsylvania and the Department of Dermatology at St. Luke’s Health Network in Easton, Pennsylvania. Drs. Ansah-Addo, McCoy, Hafeez, and Krakowski are with the Department of Dermatology at St. Luke’s Health Network in Easton, Pennsylvania.
FUNDING: No funding was provided for this article.
DISCLOSURES: The authors have no conflicts of interest relevant to the contents of this article.
ABSTRACT: Dermatitis herpetiformis (DH) is an autoimmune blistering disease associated with celiac disease, classically presenting as intensely pruritic erythematous vesicles and papules on the elbows, knees, buttocks, and scalp. Involvement of the dorsal hands is extremely rare, complicating diagnosis. We report a unique case of DH confined solely to the dorsal hands in a 68-year-old woman with a five-year history of recurrent, pruritic vesicles initially misdiagnosed as hand eczema. Direct immunofluorescence confirmed the diagnosis of DH with granular immunoglobulin (Ig) A deposition along the dermo-epidermal junction, and serologic testing revealed elevated tissue transglutaminase IgA. This case highlights an uncommon presentation of DH and emphasizes the need to consider it in chronic, unexplained dorsal hand eruptions to prevent misdiagnosis and delayed treatment. Keywords: Dermatitis herpetiformis, tissue transglutaminase, celiac disease
Introduction
Dermatitis herpetiformis (DH) is a chronic autoimmune disease closely related to celiac disease (CD). It classically presents as groups of intensely pruritic erythematous papules and vesicles, predominantly found on extensor surfaces such as the elbows, knees, scalp, and buttocks.1,2 DH is often underrecognized; its pruritic nature frequently leads to excoriations, crusting, and postinflammatory hyperpigmentation that may obscure its classic vesiculopapular morphology, leading to diagnostic challenges. Direct immunofluorescence (DIF) is the key in diagnosing DH, and mainstay treatments include gluten avoidance and dapsone.1,2
While DH predominantly impacts extensor surfaces, atypical presentations are possible and can impose significant diagnostic challenges.3-5 We present a unique and rare case of DH confined solely to the dorsal hands.
Case Report
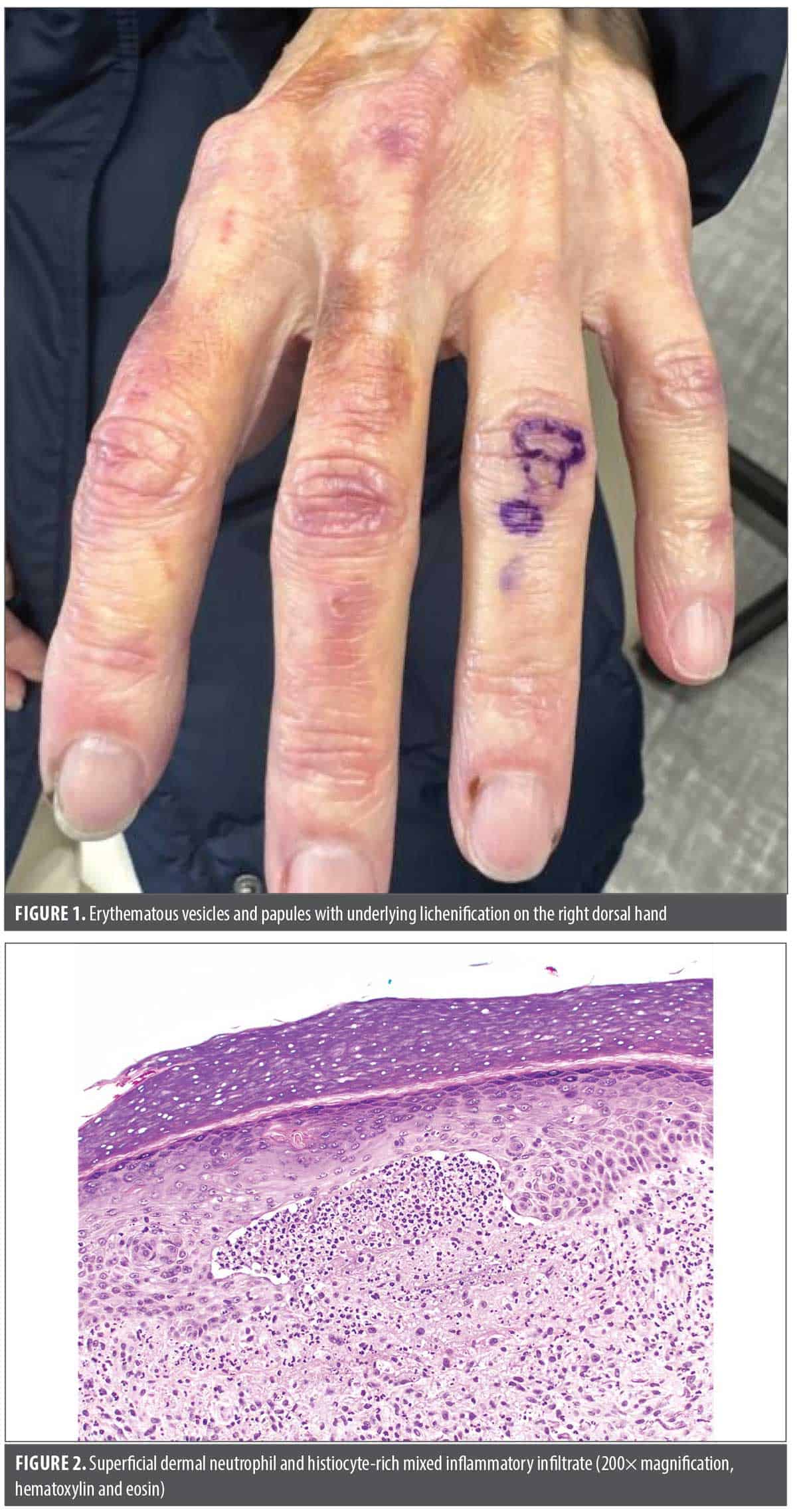
A 68-year-old woman presented to clinic with intensely pruritic vesicles and papules with underlying erythema confined to the bilateral dorsal hands (Figure 1). She worked in a hardware store and, over the past five years, had experienced intermittent crops of similar lesions confined to the same location. She had been told this was “hand eczema” secondary to her frequent handwashing. On physical exam, the patient’s vesicles and erythema were noted to be localized to the interphalangeal spaces, which raised concern for a possible underlying connective tissue disorder. No other rash was present. Screening antinuclear antibody (ANA) test and a myositis panel were negative.
A punch biopsy of the dorsal hand was performed. Histopathology revealed a subepidermal neutrophilic pustule and superficial dermal mixed inflammatory infiltrate with numerous neutrophils and histiocytes (Figure 2). DIF revealed strong granular immunoglobulin (Ig) A deposition along the dermo-epidermal junction. Tissue transglutaminase (tTg) IgA autoantibody level was elevated, while the epidermal tissue transglutaminase (eTg) IgA autoantibody level was negative. Subepithelial autoimmune blistering variant testing (laminin 332, p200, and collagen VII) and cutaneous immunofluorescence assays (cell surface antibody IgG, basement membrane IgG, primate esophagus IgG, primate split skin IgG) were negative. Further serologic testing revealed negative ANA, rheumatoid factor (RF), cyclic citrullinated peptide (CCP), Sjogren’s antibodies, and anti-double stranded DNA.
At follow-up, the patient noted a direct relationship between ingestion of gluten-containing food and drink with flares of her rash and intense pruritus. Given her overall presentation, she was diagnosed with DH. The patient has since noted significant clinical improvement with 25 mg of oral dapsone daily and by following a gluten-free diet.
Discussion
DH is an autoimmune disease first described by Louis Duhring in 1884.1 DH classically presents as an intensely pruritic polymorphic rash consisting of small vesicles, papules, and erythema distributed symmetrically on the elbows, knees, scalp, buttocks, sacral area, face, and groin.1,2 Given the intense pruritus, the rash commonly also presents with erosions, postinflammatory hyperpigmentation, and crust.1,2 Mucosal involvement of DH is rare but has been reported in the literature.2
Atypical cutaneous manifestations of DH have been documented in the literature. Unusual presentations of DH are more common in children, who can present with palmoplantar purpura or petechiae.3-5 Often, these acral purpuric manifestations of DH are accompanied by more typical-appearing lesions on the body.3-5 Somewhat uniquely, our patient demonstrated isolated involvement confined to her bilateral dorsal hands.2
The relationship between DH and CD is well established, with up to 75% of patients with DH exhibiting small bowel villous atrophy, even in the absence of gastrointestinal symptoms.1,2 Although many patients with DH lack the classical symptoms of CD, such as diarrhea and weight loss, the cutaneous findings often serve as the primary indicator of underlying gluten sensitivity.1 Even if patients with DH do not report gastrointestinal symptoms, they should be tested for CD, as untreated CD carries risk of anemia, osteoporosis, and increased risk
of malignancy.1,2
Both DH and CD share an IgA-mediated pathophysiology.1,2 Diagnostic confirmation of DH relies on DIF, which remains the gold standard. DIF can confirm DH by demonstrating granular deposition of IgA at the dermo-epidermal junction and/or within dermal papillae.1,2 Histopathology alone is often insufficient for diagnosis, as subepidermal blistering with neutrophilic infiltrates can be seen in multiple conditions, making perilesional skin biopsy for DIF crucial.1,2
Transglutaminase plays a central role in the pathogenesis of gluten intolerance.1,2,6 While tTg is the major autoantigen targeted in CD, eTg is the autoantigen most closely linked to DH.2 Approximately 50% of patients with DH are positive for IgA anti-eTg, as was the case in
this patient.2,6
This report expands the spectrum of DH presentations, highlighting a case of DH presenting solely on the dorsal hands. This underscores the importance of considering DH in atypical presentations, particularly when patients present with a chronic, relapsing, pruritic vesicular rash with or without gastrointestinal symptoms. Heightened clinical vigilance and thorough work-up are critical to the successful diagnosis and management of patients.
References
- Reunala T, Hervonen K, Salmi T. Dermatitis herpetiformis: an update on diagnosis and management. Am J Clin Dermatol. 2021;22(3):329-338.
- Bolotin D, Petronic-Rosic V. Dermatitis herpetiformis. Part I. Epidemiology, pathogenesis, and clinical presentation. J Am Acad Dermatol. 2011;64(6):1017-1024.
- Pierce DK, Purcell SM, Spielvogel RL. Purpuric papules and vesicles of the palms in dermatitis herpetiformis. J Am Acad Dermatol. 1987;16(6):1274-1276.
- Tu H, Parmentier L, Stieger M, et al. Acral purpura as leading clinical manifestation of dermatitis herpetiformis: report of two adult cases with a review of the literature. Dermatology. 2013;227(1):1-4.
- McGovern TW, Bennion SD. Palmar purpura: an atypical presentation of childhood dermatitis herpetiformis. Pediatr Dermatol. 1994;11(4):319-322.
- Hull CM, Liddle M, Hansen N, et al. Elevation of IgA anti-epidermal transglutaminase antibodies in dermatitis herpetiformis. Br J Dermatol. 2008;159(1):120-124.