J Clin Aesthet Dermatol. 2026;19(1–2 Suppl 1):S10–S12.
by Rachel Cohen, NP-C, DCNP
Ms. Cohen is with Jay L. Cohen, MD, PC in Needham, Massachusetts.
Funding: No funding was provided for this article.
Disclosures: The author reports no conflicts of interest relevant to the contents of this article.
ABSTRACT: Preventive medicine has become the foundation of modern healthcare, emphasizing early intervention and lifestyle modification to avert disease and promote longevity. Despite this paradigm shift, dermatology remains largely episodic, focused on treating visible pathology rather than conditioning the skin for resilience and disease prevention. This article introduces the concept of skin fitness, a structured, proactive model that applies the principles of physical training—progression, consistency, and recovery—to dermatologic health. By integrating evidence-based topical agents, procedures, and assessment metrics, skin fitness aims to extend “skin span,” enhance patient adherence, and position dermatology within the broader preventive and performance-based healthcare framework. Keywords: Skin barrier function, neocollagenesis, skin neoplasms, prevention and control, epidermal renewal, dermal remodeling, laser resurfacing, retinoids, keratinocyte proliferation
Introduction
Prevention has become the gold standard in medicine, from exercise in cardiology to strength training in orthopedics. Yet, dermatology continues to operate primarily within a reactive framework, addressing disease and aesthetic concerns only after they become clinically evident. Despite remarkable advances in treating visible signs of aging and skin disease, most patients still engage with dermatologic care episodically, seeking solutions for dryness, photoaging, and lesions once they appear. This approach is analogous to treating cardiovascular disease without ever considering exercise.
To modernize dermatologic care, we must reframe the skin as a trainable system, one that, like muscle or bone, can be conditioned for strength, endurance, and disease resistance.
The Concept of Skin Fitness
Skin fitness is proposed as a proactive, structured model that applies the principles of training—progression, consistency, and recovery—to the skin. Traditional skincare emphasizes maintenance through hydration, cleansing, and protection. While these measures are essential, they are largely supportive rather than reparative.
Skin fitness represents a conditioning framework designed to progressively enhance the skin’s performance and longevity. This approach recognizes the dynamic adaptability of the skin and leverages active interventions to restore, strengthen, and preserve its function over time. Just as exercise builds cardiovascular and musculoskeletal resilience, skin fitness seeks to build cutaneous resilience by training the skin to perform and recover more efficiently.
This distinction mirrors the difference between meeting a daily step count and engaging in structured aerobic exercise: one maintains health, while the other builds resilience. Skin fitness emphasizes gradual strengthening of the skin barrier, collagen network, and cellular turnover to prevent decline before it begins.
The Science Behind a Training Approach
The concept of skin fitness is supported by evidence demonstrating that the skin can adapt and strengthen through controlled, repeated stimuli:
Topical retinoids stimulate collagen production, normalize keratinocyte differentiation, and decrease keratinocyte and melanocyte atypia, reversing photodamage and improving cellular function.1,2
Antioxidants, including topical vitamin C and oral nicotinamide, reduce oxidative stress and ultraviolet-mediated carcinogenesis.3
Fractional laser resurfacing and other energy-based modalities promote neocollagenesis and can reduce actinic keratoses.4 A recent study demonstrated that nonablative fractional laser resurfacing was associated with a decreased risk of subsequent keratinocyte carcinoma (KC) development in patients with a history of a facial KC.5
Injectables, such as poly-L-lactic acid and neuromodulators, help maintain dermal structure and support tissue homeostasis.6
These interventions parallel the principles of progressive overload and recovery in exercise physiology, wherein controlled stress induces adaptive improvement.
The Skin Fitness Framework
Phase I: Foundation—barrier optimization. A successful skin fitness program begins with restoring and strengthening the skin barrier, which is the body’s first line of defense against environmental stressors and a key regulator of internal homeostasis. When compromised, the barrier becomes susceptible to dryness, irritation, and impaired cellular function. Conversely, an intact barrier minimizes transepidermal water loss and prevents penetration of harmful substances.
Given the abundance of skincare formulations, establishing a “gold standard” for barrier repair can be challenging. A simple, restorative regimen centered on cleansing, toning, periodic exfoliation, and daily photoprotection is recommended. In early stages, emollient-rich moisturizers support recovery until homeostasis is restored, at which point external moisturization becomes less needed.
Attempting aggressive treatments before establishing barrier integrity is analogous to running before learning to walk. Without foundational stability, the skin cannot properly adapt or recover from higher-intensity interventions. Once barrier resilience is demonstrated through improved tolerance, reduced reactivity, and restored hydration, the program progresses to active conditioning.
Phase II: Active training—conditioning and repair. In the active phase, performance ingredients, such as retinoids and antioxidants, are gradually introduced, followed by resurfacing procedures to promote long-term regeneration. Retinoids are advanced progressively in concentration and frequency to minimize inflammation and dryness, improving tolerance and adherence.
This stage typically spans approximately three months, corresponding to three keratinocyte maturation cycles, allowing the skin to adapt and strengthen before moving to higher-intensity interventions.
Phase III: Performance enhancement—advanced interventions. Once the skin demonstrates resilience and tolerance, in-office procedures are introduced. While CO₂ laser resurfacing remains the gold standard for rejuvenation, its downtime can limit accessibility. As an alternative, medium-depth chemical peels or fractional laser treatments—performed in a series of 3 to 5 sessions at one-month intervals—can effectively stimulate dermal remodeling with reduced recovery time.
Resurfacing not only enhances firmness and elasticity through neocollagenesis but might also reduce KC risk by removing the epidermal layer where these malignancies originate. This process parallels high-intensity interval training: brief, controlled stress triggers micro-injury and repair, producing stronger, more resilient tissue. Similarly, fractional resurfacing creates microthermal zones that activate regenerative pathways, “training” the skin to recover more efficiently.
Each procedure is followed by a recovery phase, employing gentle cleansing, recovery hydrators, and strict photoprotection. For appropriate patients, injectables such as neurotoxins or biostimulators can further enhance results and maintain structural integrity.
Phase IV: Assessment, adaptation, and maintenance. Like any effective training program, skin fitness relies on continuous evaluation and adaptation. Progress is measurable through objective parameters, such as barrier recovery time, elasticity, firmness, pigmentation evenness, and patient-reported outcomes. Skin analysis tools can be helpful for providing further insight into the quality of the skin as well as objectively monitoring progress.
By reframing skincare in a structured, trackable format, clinicians can communicate the value of consistency and progression, reinforcing adherence and long-term engagement.
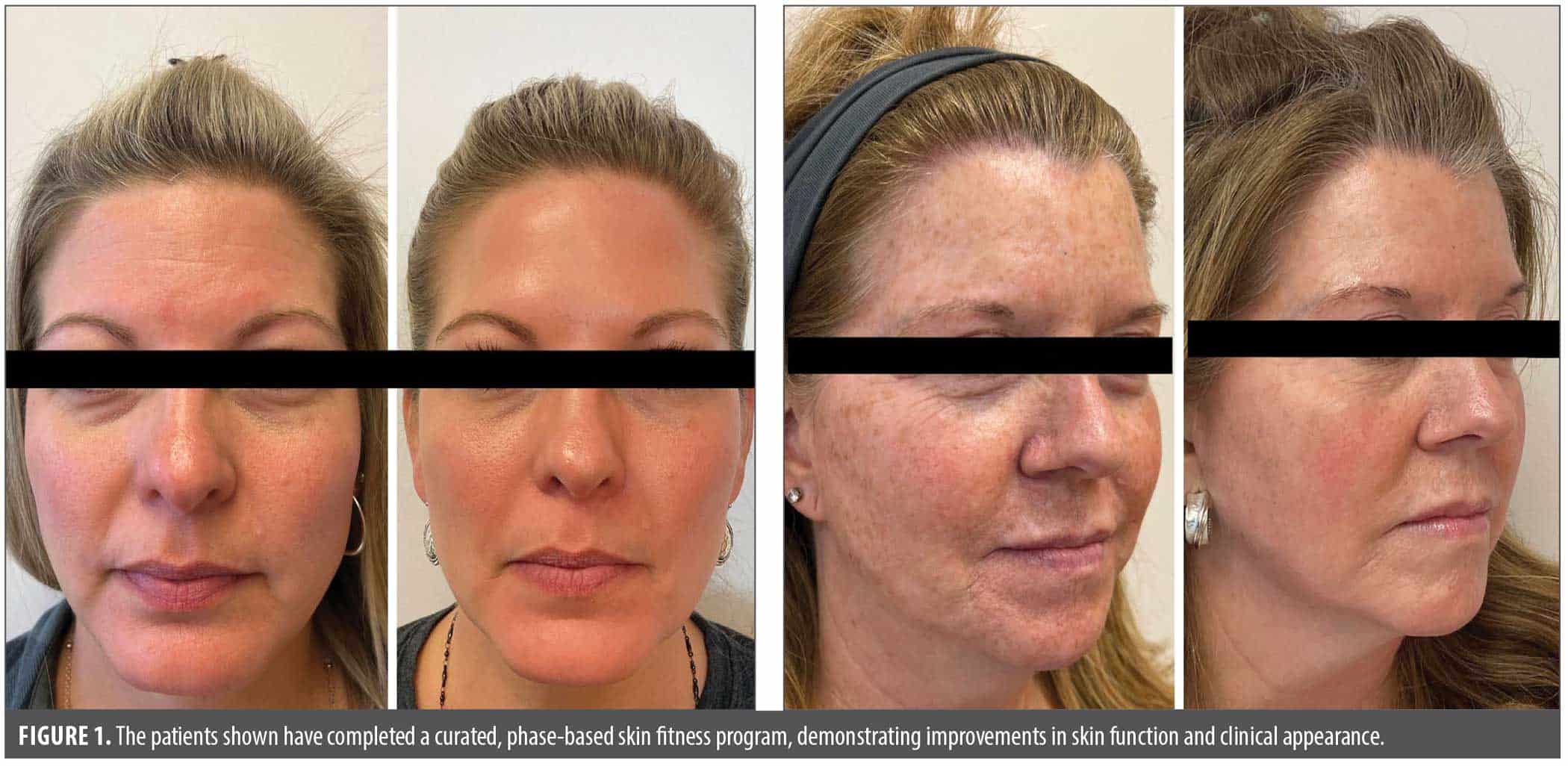
Discussion
The skin fitness model bridges the gap between reactive dermatology and preventive medicine. It aligns with the broader healthcare movement emphasizing disease prevention, performance optimization, and longevity. Conceptually, it reframes skin care not as a cosmetic endeavor but as a medical discipline rooted in physiology and adaptation.
Clinically, skin fitness might enhance patient adherence by offering a clear roadmap of progression and measurable outcomes. Scientifically, it underscores the potential of cumulative, proactive intervention in reducing photoaging, carcinogenesis, and inflammatory skin disorders. Future studies are warranted to validate “training-based” protocols and quantify their long-term impact on skin health and disease prevention.
Conclusion
Just as cardiology embraces exercise and orthopedics embraces strength training, dermatology should now embrace skin fitness. The future of skin health lies in proactive conditioning—training the skin to perform, recover, and resist decline. By redefining dermatologic care through this lens, we can transform both patient outcomes and public perception, positioning dermatology at the forefront of preventive, performance-based medicine.
References
- Kligman AM, Grove GL, Hirose R, Leyden JJ. Topical tretinoin for photoaged skin. J Am Acad Dermatol. 1986;15(4 Pt 2):836–859.
- Chien AL, Kang S. Photoaging. UpToDate. Updated 22 Jul 2025. Accessed 23 Oct 2025. https://www.uptodate.com/contents/photoaging
- Chen AC, Martin AJ, Choy B, et al. A Phase 3 trial of nicotinamide for skin-cancer chemoprevention. N Engl J Med. 2015;373(17):1618–1626.
- Hantash BM, Mahmood MB. Fractional photothermolysis for skin rejuvenation. Dermatol Surg. 2007;33(5):525–534.
- Benson TA, Hibler BP, Kotliar D, Avram M. Nonablative fractional laser treatment is associated with a decreased risk of subsequent facial keratinocyte carcinoma development. Dermatologic Surg. 2023;49(2):149–154.
- Beer K. A double-blind, randomized study of poly-L-lactic acid for facial volume restoration. Dermatol Surg. 2007;33(Suppl 2):S168–S175.
From Skincare to Skin Fitness: A Performance Framework for Dermatologic Practice
Categories:
J Clin Aesthet Dermatol. 2026;19(1–2 Suppl 1):S10–S12.
by Rachel Cohen, NP-C, DCNP
Ms. Cohen is with Jay L. Cohen, MD, PC in Needham, Massachusetts.
Funding: No funding was provided for this article.
Disclosures: The author reports no conflicts of interest relevant to the contents of this article.
ABSTRACT: Preventive medicine has become the foundation of modern healthcare, emphasizing early intervention and lifestyle modification to avert disease and promote longevity. Despite this paradigm shift, dermatology remains largely episodic, focused on treating visible pathology rather than conditioning the skin for resilience and disease prevention. This article introduces the concept of skin fitness, a structured, proactive model that applies the principles of physical training—progression, consistency, and recovery—to dermatologic health. By integrating evidence-based topical agents, procedures, and assessment metrics, skin fitness aims to extend “skin span,” enhance patient adherence, and position dermatology within the broader preventive and performance-based healthcare framework. Keywords: Skin barrier function, neocollagenesis, skin neoplasms, prevention and control, epidermal renewal, dermal remodeling, laser resurfacing, retinoids, keratinocyte proliferation
Introduction
Prevention has become the gold standard in medicine, from exercise in cardiology to strength training in orthopedics. Yet, dermatology continues to operate primarily within a reactive framework, addressing disease and aesthetic concerns only after they become clinically evident. Despite remarkable advances in treating visible signs of aging and skin disease, most patients still engage with dermatologic care episodically, seeking solutions for dryness, photoaging, and lesions once they appear. This approach is analogous to treating cardiovascular disease without ever considering exercise.
To modernize dermatologic care, we must reframe the skin as a trainable system, one that, like muscle or bone, can be conditioned for strength, endurance, and disease resistance.
The Concept of Skin Fitness
Skin fitness is proposed as a proactive, structured model that applies the principles of training—progression, consistency, and recovery—to the skin. Traditional skincare emphasizes maintenance through hydration, cleansing, and protection. While these measures are essential, they are largely supportive rather than reparative.
Skin fitness represents a conditioning framework designed to progressively enhance the skin’s performance and longevity. This approach recognizes the dynamic adaptability of the skin and leverages active interventions to restore, strengthen, and preserve its function over time. Just as exercise builds cardiovascular and musculoskeletal resilience, skin fitness seeks to build cutaneous resilience by training the skin to perform and recover more efficiently.
This distinction mirrors the difference between meeting a daily step count and engaging in structured aerobic exercise: one maintains health, while the other builds resilience. Skin fitness emphasizes gradual strengthening of the skin barrier, collagen network, and cellular turnover to prevent decline before it begins.
The Science Behind a Training Approach
The concept of skin fitness is supported by evidence demonstrating that the skin can adapt and strengthen through controlled, repeated stimuli:
Topical retinoids stimulate collagen production, normalize keratinocyte differentiation, and decrease keratinocyte and melanocyte atypia, reversing photodamage and improving cellular function.1,2
Antioxidants, including topical vitamin C and oral nicotinamide, reduce oxidative stress and ultraviolet-mediated carcinogenesis.3
Fractional laser resurfacing and other energy-based modalities promote neocollagenesis and can reduce actinic keratoses.4 A recent study demonstrated that nonablative fractional laser resurfacing was associated with a decreased risk of subsequent keratinocyte carcinoma (KC) development in patients with a history of a facial KC.5
Injectables, such as poly-L-lactic acid and neuromodulators, help maintain dermal structure and support tissue homeostasis.6
These interventions parallel the principles of progressive overload and recovery in exercise physiology, wherein controlled stress induces adaptive improvement.
The Skin Fitness Framework
Phase I: Foundation—barrier optimization. A successful skin fitness program begins with restoring and strengthening the skin barrier, which is the body’s first line of defense against environmental stressors and a key regulator of internal homeostasis. When compromised, the barrier becomes susceptible to dryness, irritation, and impaired cellular function. Conversely, an intact barrier minimizes transepidermal water loss and prevents penetration of harmful substances.
Given the abundance of skincare formulations, establishing a “gold standard” for barrier repair can be challenging. A simple, restorative regimen centered on cleansing, toning, periodic exfoliation, and daily photoprotection is recommended. In early stages, emollient-rich moisturizers support recovery until homeostasis is restored, at which point external moisturization becomes less needed.
Attempting aggressive treatments before establishing barrier integrity is analogous to running before learning to walk. Without foundational stability, the skin cannot properly adapt or recover from higher-intensity interventions. Once barrier resilience is demonstrated through improved tolerance, reduced reactivity, and restored hydration, the program progresses to active conditioning.
Phase II: Active training—conditioning and repair. In the active phase, performance ingredients, such as retinoids and antioxidants, are gradually introduced, followed by resurfacing procedures to promote long-term regeneration. Retinoids are advanced progressively in concentration and frequency to minimize inflammation and dryness, improving tolerance and adherence.
This stage typically spans approximately three months, corresponding to three keratinocyte maturation cycles, allowing the skin to adapt and strengthen before moving to higher-intensity interventions.
Phase III: Performance enhancement—advanced interventions. Once the skin demonstrates resilience and tolerance, in-office procedures are introduced. While CO₂ laser resurfacing remains the gold standard for rejuvenation, its downtime can limit accessibility. As an alternative, medium-depth chemical peels or fractional laser treatments—performed in a series of 3 to 5 sessions at one-month intervals—can effectively stimulate dermal remodeling with reduced recovery time.
Resurfacing not only enhances firmness and elasticity through neocollagenesis but might also reduce KC risk by removing the epidermal layer where these malignancies originate. This process parallels high-intensity interval training: brief, controlled stress triggers micro-injury and repair, producing stronger, more resilient tissue. Similarly, fractional resurfacing creates microthermal zones that activate regenerative pathways, “training” the skin to recover more efficiently.
Each procedure is followed by a recovery phase, employing gentle cleansing, recovery hydrators, and strict photoprotection. For appropriate patients, injectables such as neurotoxins or biostimulators can further enhance results and maintain structural integrity.
Phase IV: Assessment, adaptation, and maintenance. Like any effective training program, skin fitness relies on continuous evaluation and adaptation. Progress is measurable through objective parameters, such as barrier recovery time, elasticity, firmness, pigmentation evenness, and patient-reported outcomes. Skin analysis tools can be helpful for providing further insight into the quality of the skin as well as objectively monitoring progress.
By reframing skincare in a structured, trackable format, clinicians can communicate the value of consistency and progression, reinforcing adherence and long-term engagement.
Discussion
The skin fitness model bridges the gap between reactive dermatology and preventive medicine. It aligns with the broader healthcare movement emphasizing disease prevention, performance optimization, and longevity. Conceptually, it reframes skin care not as a cosmetic endeavor but as a medical discipline rooted in physiology and adaptation.
Clinically, skin fitness might enhance patient adherence by offering a clear roadmap of progression and measurable outcomes. Scientifically, it underscores the potential of cumulative, proactive intervention in reducing photoaging, carcinogenesis, and inflammatory skin disorders. Future studies are warranted to validate “training-based” protocols and quantify their long-term impact on skin health and disease prevention.
Conclusion
Just as cardiology embraces exercise and orthopedics embraces strength training, dermatology should now embrace skin fitness. The future of skin health lies in proactive conditioning—training the skin to perform, recover, and resist decline. By redefining dermatologic care through this lens, we can transform both patient outcomes and public perception, positioning dermatology at the forefront of preventive, performance-based medicine.
References
Share:
Recent Articles:
Lawrence Eichenfield, MD: Insights from the TRuE-AD3 Pediatric Atopic Dermatitis Trial
Tristan Hasbargen, PA-C: Setting Expectations for a Long-Term Approach to Repigmentation
David Rosmarin, MD: Efficacy of Ruxolitinib Cream in Progressive and Stable Vitiligo
Ted Lain, MD, MBA: Reviewing Results of the THRIVE-AA1 Trial in Severe Alopecia Areata
Leon Kircik, MD: Maximizing Bioavailability and Patient Outcomes With Oral Acne Therapy
Categories:
Recent Articles:
Christopher Bunick, MD, PhD: Providing Rapid Itch Relief for Patients With Atopic Dermatitis
Letter to the Editor: March 2026
The Impact of Dupilumab on Psychological Wellbeing in Moderate-to-Severe Atopic Dermatitis Patients: A Phase IV Clinical Trial
Expanding the Topical Therapeutic Landscape for Atopic Dermatitis: A Systematic Review
A Multicenter Trial Evaluating the Safety and Efficacy of a Serum Containing Plant Adaptogens in Patients With Mild-to-Moderate, Persistent Centrofacial Erythema Associated With Rosacea
Pumping Up Dermatologic Drug Reformulation: A Review of How Proton Pump Inhibitors May Revolutionize Scleroderma Treatment
Mohs Surgeons’ Postoperative Care Practices for Secondary Intention Healing: A National Survey
Lichenoid Drug Eruption From Cetirizine Treated With Upadacitinib and Dupilumab
David Cotter, MD, PhD: Patient Presentation and Clinical Trial Data for Prurigo Nodularis
James Song, MD, FAAD: Assessing Systemic GPP Treatment With Targeted Therapy
Tags: