J Clin Aesthet Dermatol. 2025;18(11):30–36.
by Christina Huang, BS; Ayush Sangari, MD; Aditya Sood, MD; Rosie Balk, MA; Anne L. Housholder, MD, MPH; and Benjamin K. Stoff, MD, MA
Ms. Huang is with Sidney Kimmel Medical College at Thomas Jefferson University in Philadelphia, Pennsylvania. Dr. Sangari is with Renaissance School of Medicine, Stony Brook University in Stony Brook, New York. Dr. Sood is with the Department of Medicine at the Zucker School of Medicine at Northwell Health in Queens, New York. Ms. Balk is with the American Academy of Dermatology in Rosemont, Illinois. Dr. Housholder is with the Department of Dermatology at the University of Cincinnati College of Medicine in Cincinnati, Ohio. Dr. Stoff is with the Department of Dermatology at Emory University School of Medicine and the Emory Center for Ethics in Atlanta, Georgia.
FUNDING: No funding was provided for this article.
DISCLOSURES: The authors report no conflicts of interest relevant to the content of this article.
ABSTRACT: Objective: Dermatologists face multiple ethical challenges, but prior publications have studied these through case-based reporting. This study evaluates what ethical issues dermatologists find most pressing through a qualitative analysis of open-ended survey responses from dermatologists. Methods: We surveyed American Academy of Dermatology (AAD) members via email (n=3999) and asked respondents to describe, in one paragraph, a recent case or scenario that was ethically challenging in their practice of dermatology. Participants also answered multiple-choice questions about which types of ethical issues they found most challenging and common, as well as several other general queries about ethics in dermatology. We then conducted qualitative analysis on the free responses (n=188) and inductively found themes and subthemes. Results: Ethical dilemmas faced by AAD members reflect numerous subthemes. The most reported ethical challenges were requests for insurance dishonesty, insurance barriers, unscheduled patients, overutilization of procedures, inappropriate medication or paperwork requests, and patient disrespect. To our knowledge, this study is the first to demonstrate the range of reported ethical challenges faced by dermatologists through qualitative analysis. Limitations: As a qualitative study, the results are not fully representative of all ethical issues faced in dermatology and do not quantify their prevalence. Conclusion: These results could direct future wider-scale, quantitative studies to gain further understanding of the ethical challenges dermatologists face and how those challenges may vary based on practice demographics. Wider ethical analysis, particularly of the financial aspects of modern dermatologic care, may benefit the dermatology workforce. Keywords: Dermatoethics, insurance, conflicts of interest, healthcare overutilization, billing
Introduction
Dermatologists face a myriad of ethical challenges. Technical advancements, from targeted biologic therapies to teledermatology, continuously improve patient outcomes and access to care.1,2 However, medical costs and disparities in access raise concerns about justice.3,4 Meanwhile, barriers to care imposed by insurance companies force healthcare providers to balance treatment benefits and cost while considering the best interests of their patients.5,6
A variety of high-impact dermatology journals have featured articles about ethical dilemmas for many years.7 However, case studies or theoretical scenarios are often presented with insightful prescriptive analysis but without data regarding which ethical dilemmas dermatologists find most common or pressing in current practice. Qualitative analyses of ethical surveys in other medical specialties, including dermatopathology, have yielded insight.8,9
To investigate ethical issues faced by dermatologists, the Professionalism and Ethics Committee (PEC) of the American Academy of Dermatology (AAD) created and administered an anonymous survey about ethics to a random sample of AAD members. We conducted qualitative analyses on free-text responses describing recent ethically challenging scenarios that respondents reported.
Methods
The survey was designed and approved by the PEC of the AAD. The study did not require institutional review board review from Emory University, as the deidentified data were already collected by the AAD. Our survey was adapted from a prior survey instrument used to investigate ethical issues affecting members of the American Society for Dermatopathology (ASDP) and underwent multiple cycles of revision by the PEC. This survey was then distributed via email by the AAD Strategic Research and Analytics Division to a random sample of 3999 fellows and associates of the AAD. Our final survey prompted respondents to briefly describe (in one paragraph) a recent case or scenario that was ethically challenging in their practice of dermatology. Respondents were further queried about which types of ethical issues they found most challenging and common, as well as several other general aspects of ethics in dermatology. Demographic information was also collected.
For the free-text portion of the survey, responses were coded using MAXQDA software (Version 2022.2; VERBI) by two authors (Huang, Sangari) with experience in qualitative research. A codebook was created inductively based on survey responses and revised through multiple versions for consistency. The codebook was also reviewed by another author (Sood) and the senior author (Stoff). Any differences between researchers in free-response interpretation were resolved by the senior author. Segments from the free responses that pertained to subthemes were tagged and recorded, and the number of segments that corresponded with each individual subtheme was recorded. If applicable, a segment could be tagged with more than one corresponding subtheme. Responses to other survey items by those who completed the free-response section were also summarized descriptively.
Results
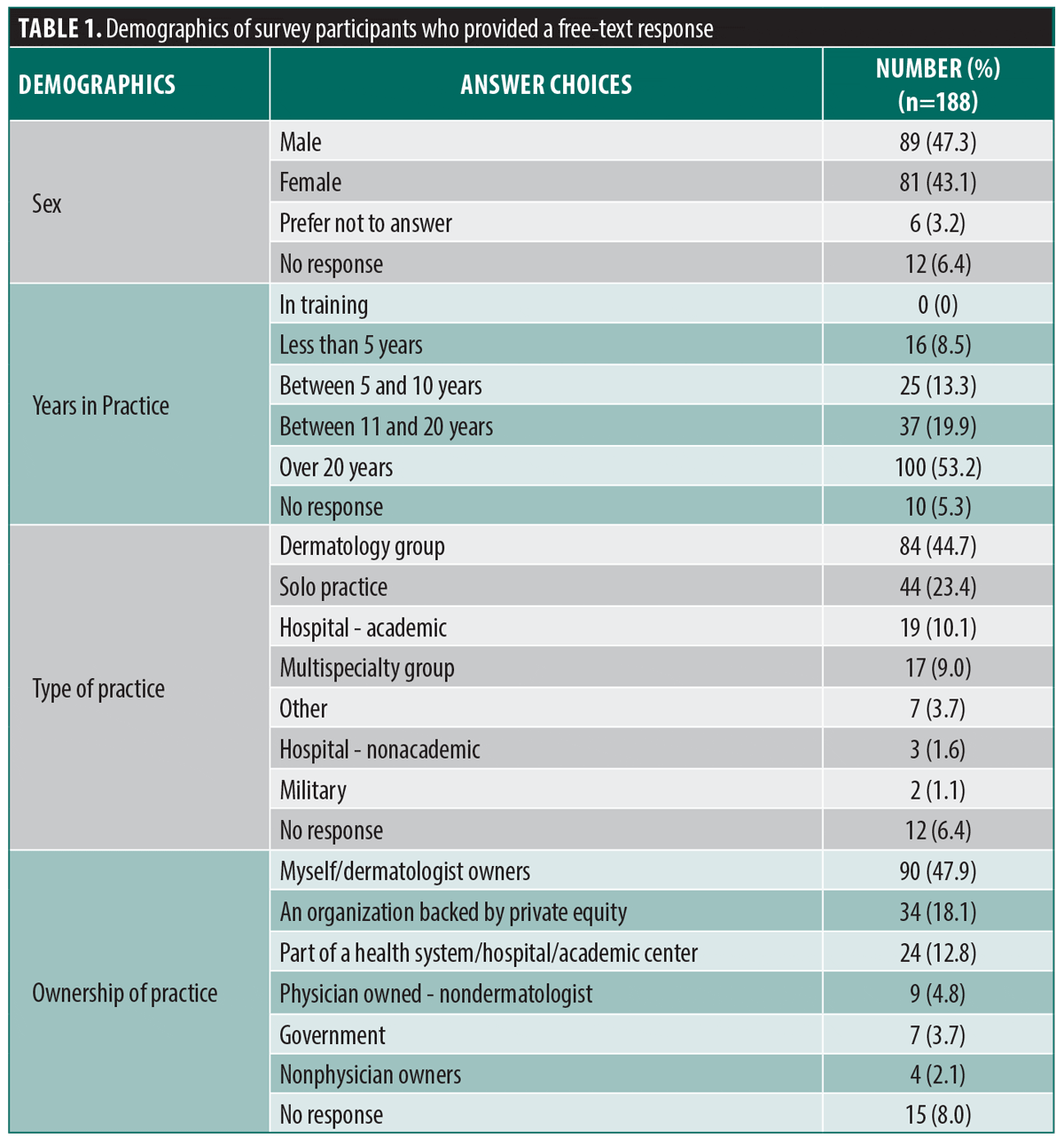
The survey was sent to 3999 AAD members via email, and of the 357 responses to the survey (survey response rate: 8.9%), there were 188 free-text responses (free-response rate for survey respondents: 52.6%). The demographics of those who offered free-text responses are summarized in Table 1.
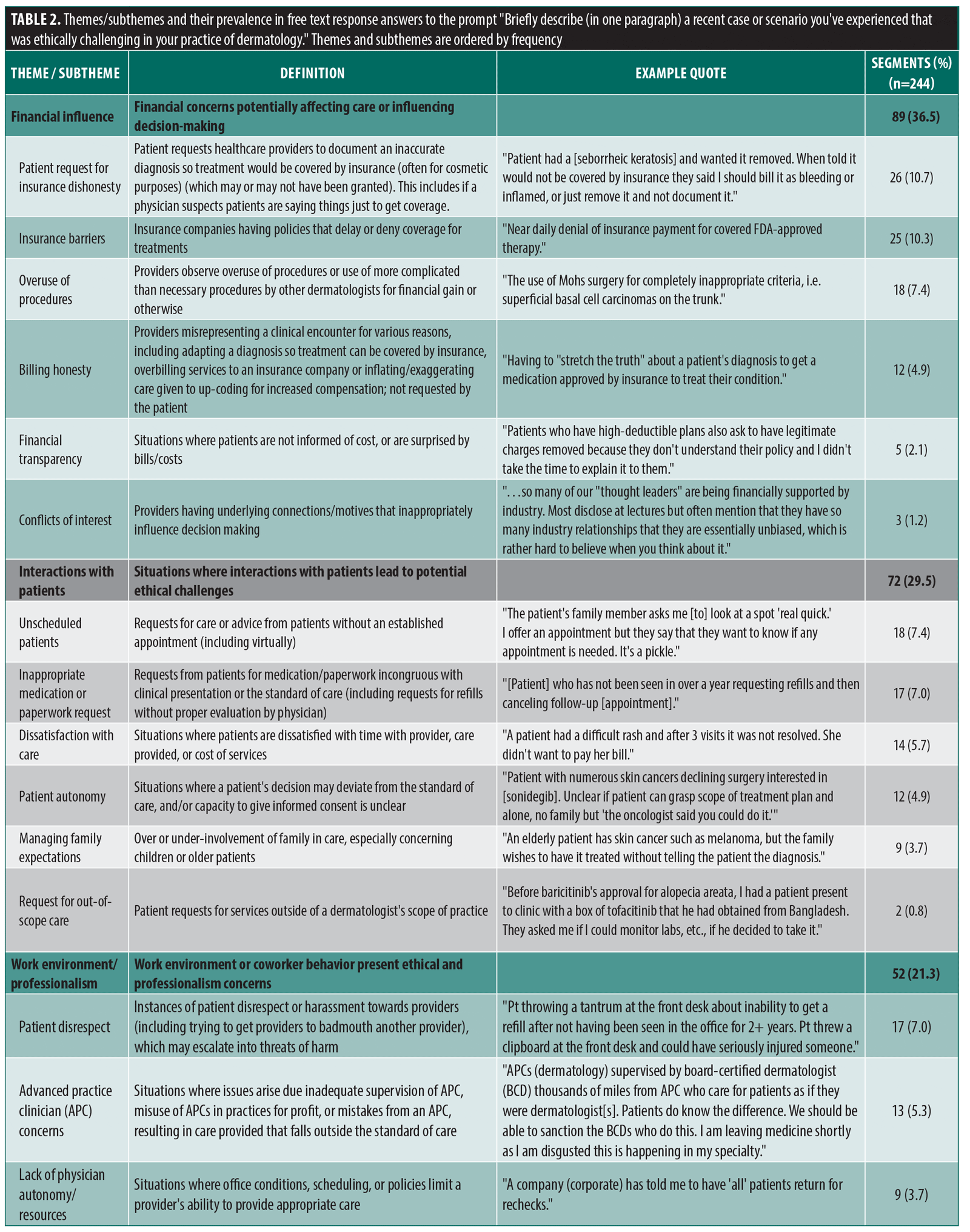
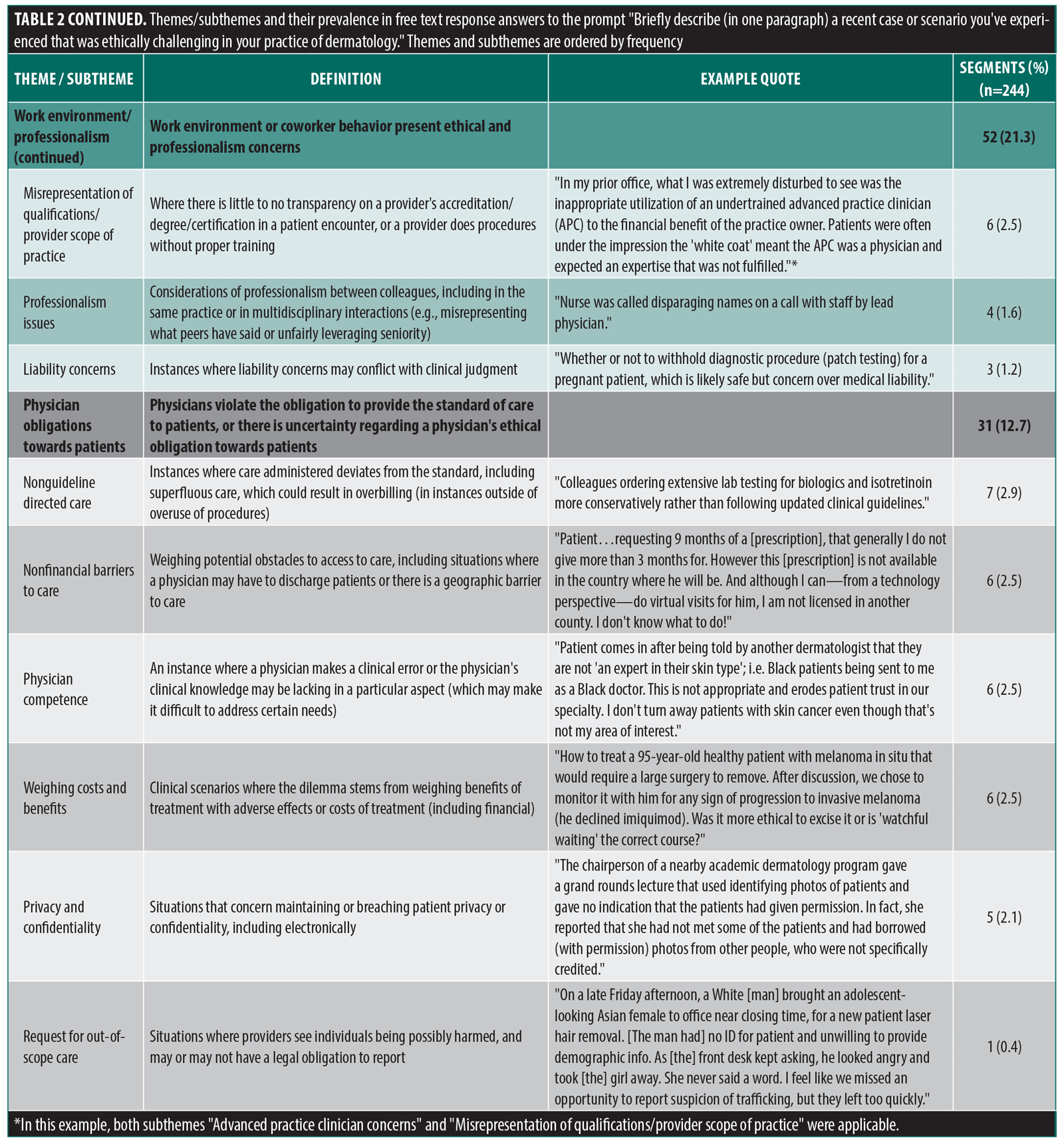
Through qualitative analysis of the 188 free responses from survey participants, we found 244 segments that referred to ethical challenges dermatologists recently encountered. Table 2 summarizes the results of the qualitative analysis.
Four overarching themes were detected in the free responses: financial influence on dermatology, interactions with patients, work environment and professionalism, and physician obligations towards patients. Additionally, we identified a total of 24 subthemes. Of note, the subthemes most prevalent in free responses about ethical dilemmas were:
- Requests for insurance dishonesty (n=26, 10.7% of segments)
- Insurance barriers (n=25, 10.3%)
- Unscheduled patients (n=18, 7.4%)
- Overutilization of procedures (n=18, 7.4%)
- Inappropriate medication or paperwork requests (n=17, 7.0%)
- Patient disrespect (each n=17, 7.0%)
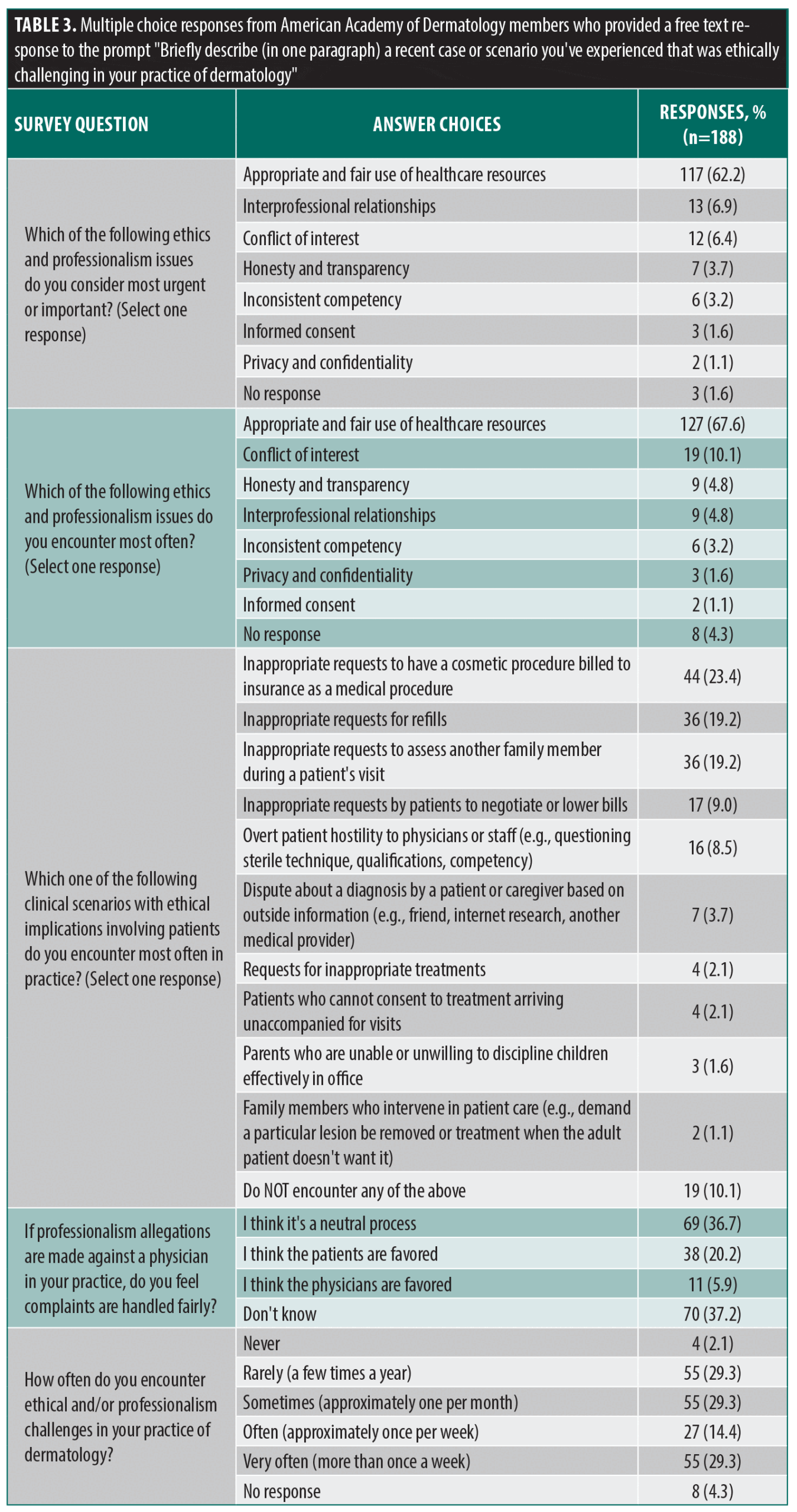
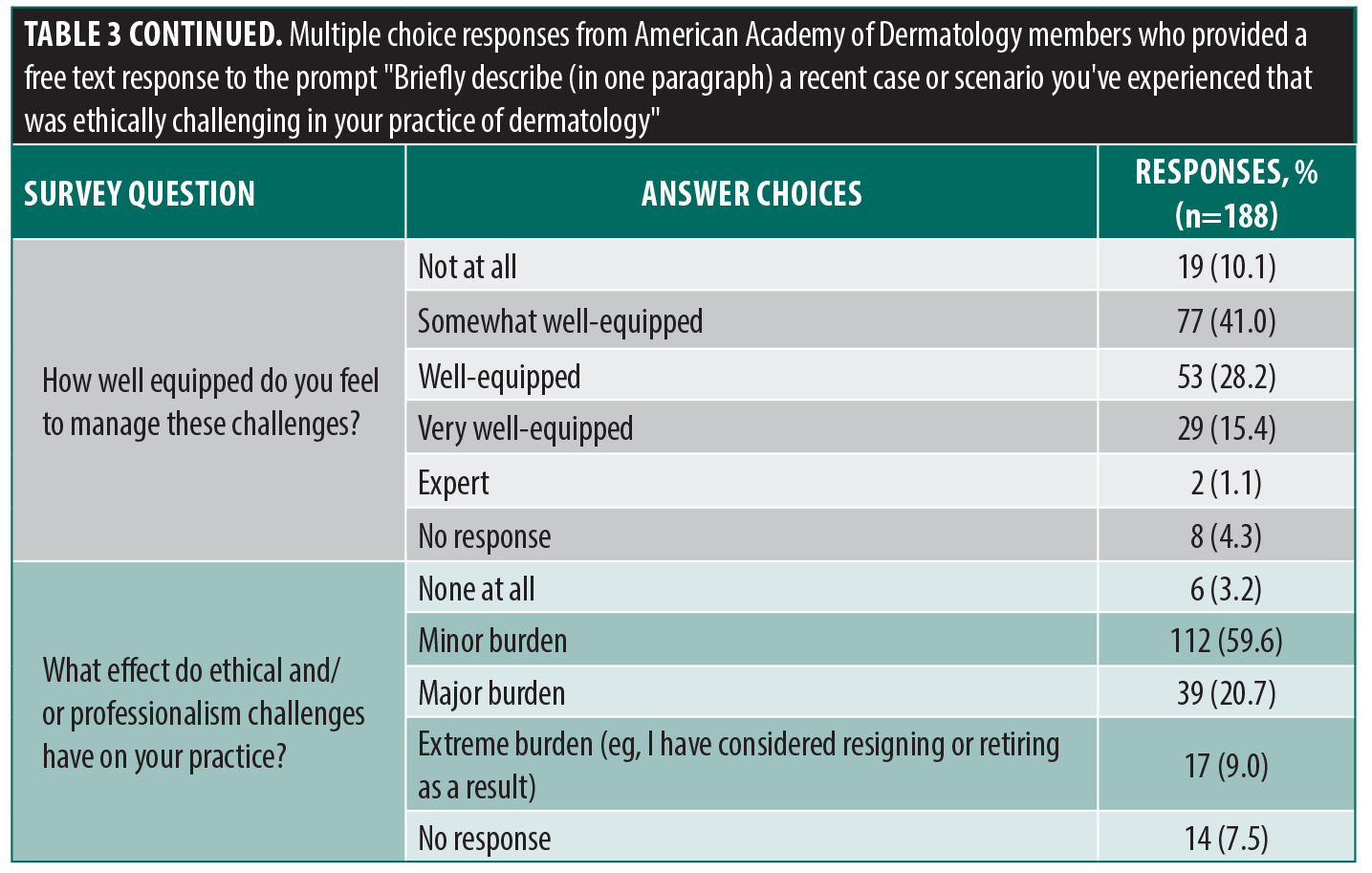
Table 3 shows ethical dilemmas that respondents considered most urgent and encountered most often, respectively. It also summarizes respondents’ perceptions of the process of resolution of professionalism allegations in their practice, frequency of ethical/professionalism dilemmas, capacity to resolve ethical issues, and overall burden of challenging ethical scenarios.
Discussion
This qualitative analysis of AAD member responses highlights multiple ethical challenges in dermatology with associated nuances. Use of qualitative methods facilitates the analysis of rich data from respondents’ own words, allowing inductive detection of subthemes that may have not been captured in a more quantitative multiple-choice survey format.
Dermatologists most often cited financial influence as an ethical challenge, with patient requests for insurance dishonesty and barriers imposed by insurance companies being the first and second most common subthemes, respectively. Patients may feel financial pressure because of the cost of healthcare or the nature of their health insurance plans, leading to requests for dermatologists to help with this burden through certain billing practices (e.g., requesting a benign seborrheic keratosis removal for cosmetics purposes to be documented as medically necessary). The ethical concern raised by patient requests for insurance dishonesty links to a separate subtheme, billing honesty, where some dermatologists make documentation changes to facilitate billing. Notably, in billing honesty segments, some actions were intended to lower out-of-pocket cost for patients (n=8), such as in the case of “stretching the truth” to obtain coverage of a medication, as opposed to overbilling to inflate compensation (n=4). Several case discussions have explored ethical implications of “stretching the truth” for insurance coverage in dermatology.6,10
In cases of patient requests for insurance dishonesty, 19 of 26 segments specifically noted patients requesting coverage for cosmetic procedures. The importance of this issue is also highlighted in multiple-choice responses as well, with 23.4% of respondents noting that “inappropriate requests to have a cosmetic procedure billed to insurance as a medical procedure” was the issue most encountered in their practice from the given choices. Between patient requests for insurance dishonesty and barriers by insurance companies, many challenging ethical scenarios in dermatology appear to result from interactions with third-party payers.11,12 Dermatologists have begun exploring ways to use new technology, such as large language models, to advocate to insurance companies on the behalf of patients.13
Overuse of procedures was another concern under financial influence. Nine out of 18 segments about overuse of procedures specifically noted inappropriate use of Mohs micrographic surgery, the use of which has increased greatly in the last few decades.14 Mohs appropriate use criteria (AUC) was created to help guide judgment on whether Mohs surgery is indicated in specific clinical scenarios.15 However, responses in the survey suggest that, even with AUC, some dermatologists may still inappropriately use Mohs or not favor treatment options that could be more appropriate in certain situations.
The next most prevalent theme was interactions with patients, a broad category that included different types of clinical interactions with patients resulting in ethical dilemmas. Many dermatologists report getting curbside requests from family members of the patient during appointments, which has been explored in prior ethical analysis.16 Scenarios under this theme often involve situations where a patient requests something that could violate medical ethical norms, such as requesting evaluations without proper time/resources or providing refills without proper consultation in an appointment or regular follow-up. However, the patient-physician relationship could become strained depending on the dermatologist’s response, as described in recent ethics case analyses.17,18 In these situations, training on how to preserve the patient-physician relationships in challenging situations and advocacy for maintaining high ethical standards could be helpful.
Segments coded under work environment/professionalism reflect concerns dermatologists have with their work environment, including interactions with administrators, advanced practice clinicians (APC), peers, and patients. Hostile environments related to patient disrespect were most prevalent, where situations could range from merely uncomfortable to feeling physically unsafe. Dermatologists also reported dilemmas regarding inadequate supervision or overuse of APCs for profit. Others noted instances where there is a lack of physician autonomy and adequate resources. To preliminarily investigate whether concerns of physician autonomy/resources differed across practice settings (e.g., private equity-backed dermatology group practices vs. independent group practices vs. hospital-based group practices), we also looked at the practice settings for healthcare providers who reported this as an issue after coding and how the practice was owned. The nine segments reporting physician autonomy/resources came from nine different dermatologists. We found that five belonged to dermatology groups, while one each was in hospital, solo dermatology, corporate clinic, and academic outpatient settings, respectively. Four reported their practice was owned by private equity, two reported the practice was hospital-owned, and two were self or dermatologist owned. However, this sample size was too limited to be meaningful, and further studies are required to comprehensively investigate how concerns vary across different practice settings.
Finally, the subtheme “physician obligation toward patients” explores duties dermatologists have in their role that could be ethically challenging. Dermatologists discussed witnessing a failure to follow standard-of-care guidelines. This was attributed to superfluous care aimed at increasing billing, physician unfamiliarity with recent care guidelines, or other unspecified reasons. In addition, dermatologists reported challenging scenarios related to decision-making when weighing the costs and benefits of different treatments for patients with no easy answer. In such situations, familiarity with the ethical frameworks of medical decision-making can aid dermatologists in their approach to patient management.19 Out of all the identified themes in this analysis, issues pertaining to physician obligation are central to traditional principle-based medical ethics, of which even experienced clinicians might benefit from periodic review.
Compared to analogous studies in dermatopathology, this study identified similar themes of ethical challenges. Financial influence was identified as a major concern by both dermatologists and dermatopathologists, though the specific ethical challenges faced were different. For example, dermatopathologists reported overuse of stains and diagnostic overcall as major ethical challenges, whereas dermatologists did not report these concerns.9 The survey study in dermatopathology also reported appropriate and fair utilization of healthcare as a major ethical concern, with overuse of immunohistochemistry being one major contributor.20 This parallels concerns about overutilization of procedures in dermatology reported in our survey.
In our survey, nearly 30% of respondents reported that professionalism/ethical issues created a major to extreme burden, and around 50% felt not equipped at all or only somewhat equipped to handle ethical dilemmas. These results emphasize that ethical challenges have serious implications for clinical practice and providers, possibly contributing to dermatologist burnout.21 In addition, having improved systems in place for reporting and managing challenging scenarios could reduce the burden felt by dermatologists.
Qualitative analysis, despite independent analyses and multiple rounds of revision to increase consistency, is inherently subjective. For some responses, the context of an ethical dilemma could be inferred based on what is often encountered in clinical practice but was not explicitly stated. Furthermore, there can be overlap of themes as multiple factors coincide in a given clinical scenario. For example, our subtheme “dissatisfaction with care” is grouped under the theme “interactions with patients,” but financial burden of healthcare on the patient could factor into ethical challenges as well, making it also relevant to the theme “financial influence.” Although our sample was representative, the response rate for this study was relatively low, and it is unlikely that thematic saturation has been achieved for this complex topic. However, qualitative research is not intended to be broadly representative but rather to explore a novel area of study and generate a rich set of topics for further investigation. Finally, awareness that survey data is being collected for research could influence respondents.22
Conclusion
Our study is the first to demonstrate the range of reported ethical challenges faced by dermatologists, highlighting areas for future exploration. Based on these results, a wider-scale, quantitative study could be helpful to gain a more comprehensive understanding of everyday ethical challenges dermatologists face and how those challenges may vary based on demographic information. This study suggests that wider ethical analysis, particularly of the financial aspects of modern dermatologic care, may benefit the dermatology workforce.
References:
- Maddukuri S, Patel J, Lipoff JB. Teledermatology addressing disparities in health care access: a review. Curr Dermatol Rep. 2021;10(2):40-47.
- de Ruiter CC, Rustemeyer T. Biologics can significantly improve Dermatology Life Quality Index (DLQI) in psoriatic patients: a systematic review. Psoriasis (Auckl). 2022;12:99-112.
- Pala P, Bergler-Czop BS, Gwiżdż JM. Teledermatology: idea, benefits and risks of modern age – a systematic review based on melanoma. Postepy Dermatol Alergol. 2020;37(2):159-167.
- Santoro FA, Rothe MJ, Strober BE. Ethical considerations when prescribing biologics in dermatology. Clin Dermatol. 2012;30(5):492-495.
- Krausz AE, Manning JR, Vinelli GL, Ciocon DH. Navigating barriers to patient access and reimbursement in Mohs micrographic surgery. Dermatol Surg. 2020;46(5):599-604.
- Weston G, Rothe MJ, Kels BD, Grant-Kels JM. The good, the bad, and the ugly of medication coverage: Is altering a diagnosis to ensure medication coverage ethical? Int J Womens Dermatol. 2016;2(2):67-68.
- Grant-Kels JM, Bercovitch L. Why a new section dedicated to ethics in the JAAD? J Am Acad Dermatol. 2011;64(2):432-433.
- MacKenzie CR, Meltzer M, Kitsis EA, Mancuso CA. Ethical challenges in rheumatology: a survey of the American College of Rheumatology membership. Arthritis Rheum. 2013;65(10):2524-2532.
- Sood A, Brahmbhatt M, Flowers N, Yeung H, Vong G, Stoff BK. Challenging ethical scenarios reported by American Society of Dermatopathology members: a qualitative analysis. J Cutan Pathol. 2022;49(2):191-196.
- Jadoo SA, Lipoff JB. Prescribing to save patients money: ethical considerations. J Am Acad Dermatol. 2018;78(4):826-828.
- Sedghi T, Gronbeck C, Aiudi DA, Grant-Kels JM. Assessing the ethics of prior authorization denials and step therapy policies in dermatology. J Am Acad Dermatol. 2024;90(4):877-878.
- Jayakumar KL, Lipoff JB. Balancing patient care with profitability: ethical considerations. J Am Acad Dermatol. 2017;77(2):382-384.
- Agarwal A, Stoff B. Ethics of using generative pretrained transformer and artificial intelligence systems for patient prior authorizations. J Am Acad Dermatol. 2024;90(5):1121-1122.
- Asgari MM, Olson JM, Alam M. Needs assessment for Mohs micrographic surgery. Dermatol Clin. 2012;30(1):167-175.
- Connolly SM, Baker DR, Coldiron BM, et al. AAD/ACMS/ASDSA/ASMS 2012 appropriate use criteria for Mohs micrographic surgery: a report of the American Academy of Dermatology, American College of Mohs Surgery, American Society for Dermatologic Surgery Association, and the American Society for Mohs Surgery. J Am Acad Dermatol. 2012;67(4):531-550.
- Sangari A, Sood A, Stoff BK. What to do when you are curbsided by your patient’s plus one. J Am Acad Dermatol. 2024;90(3):671-672.
- Gitin A, Samia AM, Grant-Kels JM, Saikaly SK. Ethical issues surrounding a patient requesting inappropriate care. J Am Acad Dermatol. 2024;90(2):450-451.
- Baranowski MLH, Chisolm S, Stoff BK. Patient requests to alter the medical record. J Am Acad Dermatol. 2019;81(4):1032.
- Sood A, Sangari A, Stoff BK. Recommending expensive treatments: An ethical analysis. J Am Acad Dermatol. 2022.
- Brahmbhatt M, Yeung H, Vong G, et al. Ethical and professionalism issues in dermatopathology: a cross-sectional survey of American Society of Dermatopathology Members. J Cutan Path. 2021;48(6):750-757.
- Nagler AR, Shinkai K, Kimball AB. Burnout among all groups of physicians—mitigation strategies for dermatologists. JAMA Dermatol. 2020;156(10):1049-1050.
- Anderson C. Presenting and evaluating qualitative research. Am J Pharm Educ. 2010;74(8):141