J Clin Aesthet Dermatol 2023;16(8 Suppl 1):S18–S22
J Clin Aesthet Dermatol 2023;16(8 Suppl 1):S18–S22
Daniel M. Siegel, MD, MA, FAAD, FACMS, and Leon Kircik, MD
Dr. Siegel is with SUNY Downstate Health Sciences University in Brooklyn, New York. Dr. Kircik is with Icahn School of Medicine at Mount Sinai in New York, New York.
Funding: Funding for this article was provided by Verrica Pharmaceutical in West Chester, Pennsylvania.
Financial Disclosures: Dr. Siegel: has been a consultant for Verrica Pharmaceutical in West Chester, Pennsylvania; he reports no other conflicts of interest relevant to the content of this article. Dr. Kircik has been a consultant, speaker, advisory board member, and/or investigator for and received honoraria and/or grant funding from the following companies: Abbott Laboratories, Abbvie, Ablynx, Aclaris, Acambis, Allergan, Inc., Almirall, Amgen, Inc., Anacor Pharmaceuticals, Anaptys, Arcutis, Arena, Assos Pharma, Astellas Pharma US, Inc., Asubio, Bausch Health, Berlex Laboratories (Bayer HealthCare Pharmaceuticals), Biogen-Idec, Biolife, Biopelle, BMS, Boehringer-Ingleheim, Breckinridge Pharma, Cassiopea, Centocor, Inc., Cellceutix, Cipher, Coherus, Colbar, Combinatrix, Connetics Corporation, Coria, Dermavant, Dermira, Dermik Laboratories, Dow Pharmaceutical Sciences, Inc., Dr. Reddy’s Lab, Dusa , Embil Pharmaceuticals, Eli Lilly, EOS, Exeltis, Ferndale Laboratories, Inc., Foamix, Ferrer, Galderma, Genentech, Inc., GlaxoSmithKline, PLC, Glenmark, Health Point, LTD, Idera, Incyte, Intendis, Innocutis, Innovail, Isdin, Johnson & Johnson, Kyowakirin Laboratory Skin Care Inc., Leo, L’Oreal, 3M, Maruho Medical International Technologies, Merck, Medicis Pharmaceutical Corp., Merz, Nano Bio, Novartis AG, Noven Pharmaceuticals, Nucryst Pharmaceuticals Corp., Obagi, Onset, OrthoNeutrogena, PediaPharma, Pfizer, Promius, PuraCap, PharmaDerm, QLT, Inc., Quinnova, Quatrix, Regeneron, Sanofi, Serono (Merck Serono International SA), SkinMedica, Inc., Stiefel Laboratories, Inc., Sun Pharma, Taro, TolerRx, Triax, UCB, Valeant Pharmaceuticals Intl., Verrica Pharmaceutical, Warner-Chilcott, XenoPort, and/or ZAGE.
ABSTRACT: It is important for dermatologists who treat molluscum contagiosum (MC) to be aware of documentation and coding requirements for reimbursement by insurance payors when treating patients with molluscum contagiosum (MC). For example, treating 15 or more MC lesions in one patient during a single visit is coded differently than treating fewer lesions. Additionally, MC reimbursement codes are specific to the area of the body being treated. In general, coding for MC destruction should be as specific as possible, with detailed documentation and photographs. This article reviews procedures for determining reimbursement and provides guidance on accurately documenting and coding medical services for treatment of MC to optimize reimbursement from insurance carriers.
The American Medical Association’s Current Procedural Terminology (CPT®) code set is a system of nomenclature used by healthcare providers, health insurance providers, and medical review boards in the United States to uniformly identify medical, surgical, and diagnostic services provided to patients.1 Use of the CPT coding system is mandated by most American health insurance providers; thus, it is imperative that, when submitting for reimbursement, dermatologists understand how to properly code and document the services they provide for their patients, including those services provided for the treatment of molluscum contagiosum (MC). Incorrectly coding an MC procedure(s) and/or inaccurately or incompletely documenting the services provided to patients can negatively impact reimbursement to the dermatologist. In this article, methods of reimbursement determination are explained, and guidance for properly and accurately coding and documenting treatment services for MC is provided.
Resource-based Relevant Value System
The Resource-Based Relevant Value System (RBRVS) Data Manager is an important database service that is available by subscription.2 A slightly different interface is used by the Resource-Based Relative Value Update Committee of the American Medical Association (RUC), which has an advisory function with respect to the Centers for Medicare and Medicaid Services (CMS). A committee with broad representation from the house of medicine, the RUC makes recommendations to CMS for valuation of CPT codes. Using the database, various codes and procedures can be searched and the relative value unit (RVU) for that treatment appears. The RVU does not define physician compensation in a direct way; instead, the RVU number is multiplied by the conversion factor for that year to arrive at a monetary amount. To this end, clinical vignettes are sometimes used, which describe a hypothetical case, diagnosis, treatment, and other relevant information. Vignettes specify what steps and information are needed for “pre-service,” “intra-service,” and “post-service.” As a general rule, the pre-service notes are to record everything that is done prior to the procedure and may include evaluation, patient history, review of records, discussion of medical risks, informed consent, patient education, procedural preparation (e.g., set-up of equipment, gloves, lighting, drapes), and preparation of nondisposable equipment (e.g., scissors). By contrast, the “intra-service” describes the procedure itself. Finally, “post-service” should describe patient instructions following the procedure, the use of any dressings or antibiotic ointments applied, patient communications, and charting.2
Case Vignette 1
A patient comes to the clinic with MC, and the dermatologist and patient discuss treatment options. That can be coded as an office visit. If the patient returns the following week for a procedure, that would be coded as a procedure but not an office visit, even if the patient has questions in advance of the procedure. Now imagine that the dermatologist notices this same patient has sunburn and discusses it with the patient during the same visit in which the MC procedure is performed. The dermatologist recommends a specific type of sunscreen. This may be counted as a significant and separate service and may be coded separately, even though both this visit and the MC procedure occurred during the same clinic visit.
Direct Practice Expenses
Direct Practice Expenses are also captured in billing, and in dermatology, supporting healthcare professionals are deemed by the database to be an amalgamation of Registered Nurse, Licensed Practical Nurse, and Medical Therapy Assistant.3 Their value on a national basis is $0.455 a minute, which is a cost that the dermatology practice incurs when providing the service. Medical supply direct inputs are described in the database, ranging from destructive products (liquid nitrogen, for example), disposables, and so on. Durable equipment is also figured in, such as surgical instruments, cryosurgery equipment, examination table, lighting, and so on. Utilization is captured by frequency data, (i.e., the number of times various specific codes have been used by year). Other data include the top-five most frequently used diagnostic codes reported on the same day of service, places of service, and specialties.
National Correct Coding Initiative (NCCI)
The NCCI was launched by CMS to promote correct coding methodology and reduce coding errors that might lead to inappropriate payment of Medicare Part B claims.4 Information on this initiative is available on the NCCI website. A very helpful feature of the website is the NCCI FAQs page, which provides insight into how the NCCI would be applied to real-world coding examples.5 The Correct Coding Initiatives (CCI) report reveals whether certain pairs of codes can be reported together. The CCI spreadsheet is an extensive document that shows which pairs of codes are mutually exclusive. For example, CPT Codes 17110 and 17111 are mutually exclusive. Medically unlikely edits (MUEs) refer to a service claim edit made against a procedure code for services considered to be unlikely or improbable when offered by one provider on one day to one patient. To limit errors and reduce fraud, automated claims processing systems look for specific MUEs, though not all codes have an MUE. In general, an MUE states the maximum units of service a provider would likely report under most circumstances for one patient on one day.
CPT modifiers supplement coding to add extra relevant information about a service or procedure. To this end, a modifier does not change or amend the CPT code but simply fills in more information about it. Modifier-25 is perhaps one of the best-known CPT modifiers and could be defined as describing a significant and separately identifiable evaluation and management service carried out by the same healthcare provider on the same day as another procedure or service. Modifier-25 allows a dermatologist to use time efficiently and perform an evaluation or management service on the same day as a procedure; this can also save the patient another visit to the clinic. However, it is important to note that the evaluation and management service must be significant and separate. To qualify as significant, this evaluation or management service would necessitate another visit to the clinic if it were not carried out that same day (Case Vignette 1). From a self-audit perspective, if the physician, after looking over his or her documentation, removes all documentation relating to the procedure, including pre- and post-service work as noted above, an evaluation and management would only be appropriate to report if the remaining note could stand on its own for an evaluation and management service.
Modifier-59 can be applied when two distinct and independent services or procedures are carried out on the same patient on the same day. Modifier-59 does not deal with evaluation and management, as Modifier-25 does. The main distinction between Modifier-25 and Modifier-59 is that Modifier-25 must be used together with a CPT code that is designated as evaluation or management. Modifier-59 can be used with procedures to refer to a distinct service (Case Vignette 2).
Modifier-59 basically confirms that two or more independent procedures are carried out on the same day. For example, a biopsy and destruction of an MC lesion done on the same day could be billed either as a biopsy or a destruction but not both (Case Vignette 3).
If one lesion was biopsied while one or more other lesions were destroyed (if such management is advisable when there is a question of diagnosis), using Modifier-59 informs the payer that it was necessary to do these two different procedures on the same patient on the same day on different lesions on different sites. The physician may not perform a biopsy and a destructive procedure on the same lesion on the same day. Typically, treatment of MC is based on clinical examination, though a biopsy may be performed if the diagnosis is uncertain or in cases with medicolegal concerns, such as possible child abuse. It is important for a dermatology practice to be up to date on the NCCI and MUE edits, and to blend these with common sense and meticulous documentation. CPT Codes 17110 and 17111 cover skin benign destruction services, except in cases in which a more specific code exists. When billing, the most precise code available should be used. It is acceptable and good coding practice to mix and match codes as appropriate to cover what was carried out. A good rule of thumb is to document what was done, to perform exactly what was documented, and to report what was medically necessary using the appropriate CPT and ICD-10 codes. Careless errors in coding can compromise practice efficiency and put the provider at risk for financial penalties.
Case Vignette 2
A patient comes to the clinic for treatment of MC lesions on several parts of the body, including the arms, penis, and anus. Coding can be done for specific body regions. This means that one of the procedures becomes the main code and the others use Modifier-59. If the dermatologist fails to apply Modifier-59, the payer may apply it themselves or reject the claim, but it is easy to submit it with the Modifier-59 in place to minimize payment delays.
Case Vignette 3
A patient comes to the clinic with a suspicious lesion. The dermatologist is doing a biopsy and a destruction at the same site same day. The dermatologist then sends the specimen to the laboratory. At this point, the dermatologist may bill for the biopsy or a destruction but not both on the same lesion on the same patient on the same day. If the lesion is persistent, a further destruction may be performed any time if the biopsy was reported initially. If destruction is reported on the first encounter, further destruction of the same lesion is not reportable within the 10-day global period but is after that time period. If the dermatologist did not perform the curettage and cautery at that time, it could be performed later if there is residual lesion in need of further treatment after getting biopsy confirmation. MC lesions are usually small, and further treatment typically will not be needed for a biopsied lesion. Any lesions treated on a subsequent visit would be reported with appropriate CPT codes.
Forward Deployed Inventory
Forward deployed inventory is not just a healthcare term—it refers to any inventory that is held by an organization but only purchased upon use. In a dermatology practice, this includes products kept in the office that are only paid for when they are used. In other words, the dermatology practice may have products on hand that it has not yet purchased and need not purchase until it uses them. This has been compared to the mini-bar model in a hotel where one purchases only what one consumes. Forward deployed inventory in the dermatology office offers some business advantages: the practice does not need to invest in purchasing an inventory, and it only pays for what it needs when it needs it. It also allows delivery of new items based on actual need, so that the inventory is frequently replenished. A well-managed forward deployed inventory does not typically have shortfalls, but one downside is the ambiguity surrounding whether it is the insurer or the patient who pays for these items. For example, CMS will not pay for product if a procedure is billed with a lesion destruction code; the product is considered to be included as part of the lesion destruction code. However, this may not always be the case, and private insurers may do things differently. Another potential drawback to forward deployed inventory is “shrinkage,” which refers to theft of inventory.
J Codes
J codes are a set of special codes that identify certain drugs, particularly injectables, and other items often used by dermatologists. For instance, there are specific J codes for the drugs used in photodynamic therapy. However, there are no J codes that can be used with MC lesion destructive therapies because any products used in this context are considered to be included in the lesion destruction code.
J codes are Level II billing codes that are used for supplies, drugs, and medical devices. While they do not cover topical products used in conjunction with an MC lesion destruction code, they may cover other topical or injectable products in other procedures. They are issued for new drugs and other products as they come to market. J codes are often based on unit dosing, particularly if the product is available in a single-use, prefilled applicator. Note that CMS will not reimburse on J codes in destruction procedures, but private payers may reimburse on J codes, particularly if they see economic benefit in making a specific product available with long-term cost effectiveness. Dermatologists should take into consideration that sometimes patients leave the office with a prescription, which they then fill, utilizing their own insurance for payment or paying out of pocket. However, administering a product in the office may offer certain advantages, such as ensuring proper application and treatment adherence. Some private insurance companies may see sufficient advantage to that so that products are reimbursed for office use.
“Simple” Versus “Extensive” in MC Treatment
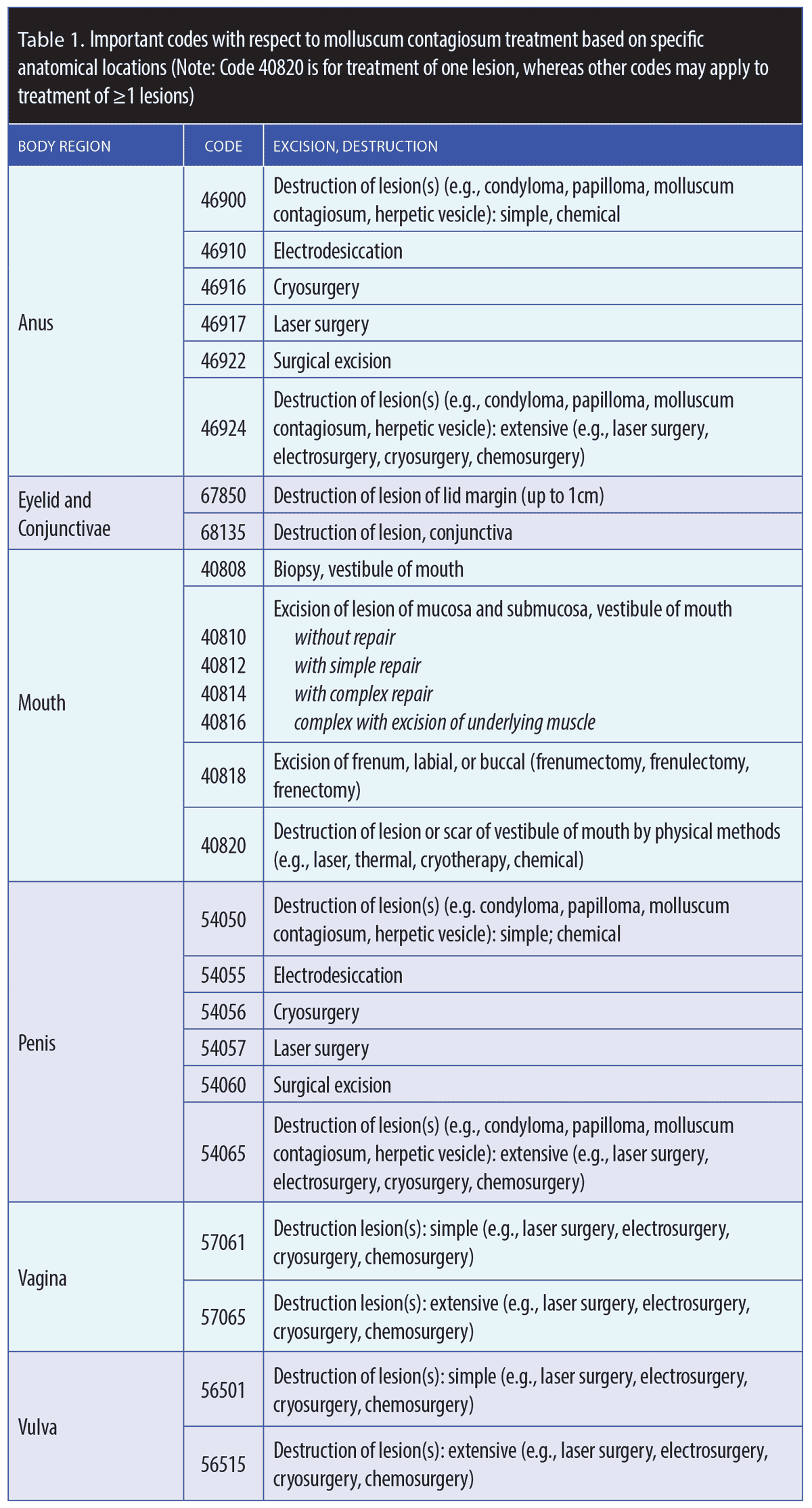
When coding for MC of skin, the number of lesions is important for reporting the correct code. When performing destructions in other areas (Table 1), it is crucial to distinguish between simple and extensive procedures. The CPT uses these terms but does not define them. Simple does not mean single or a few, although that may not seem intuitive, and the required number of lesions needed to satisfy the designation of extensive remains murky. A general rule of thumb, however, is if the number of lesions being treated can be easily counted, that’s considered simple, whereas if the treated lesions are too numerous to count, that’s considered extensive. A procedure that is complicated or unusual may also likely be categorized as extensive, regardless of the actual lesion count. One reason for this ambiguity is that these codes are old, dating back to the early days of CPT, and are used to document low-volume procedures, which means they likely have not undergone review and updating by the RUC. It is worth noting that private payers will sometimes reimburse for certain products or procedures for which the CMS will not pay, provided the dermatologist can provide solid documentation supporting their use.
Certain codes are mutually exclusive. For example, CPT Codes 17110 and 17111 cannot be used in reference to the same patient on the same day, and repeat treatment of the lesions in the same area over the following 10 days would not be separately reportable. The global time period for these codes is10 days, meaning neither of these two codes may be used again in reference to the same patient within a 10-day window. If more lesions were treated on a separate area of the skin within the global period, the dermatologist may need to indicate that the procedure or service performed during the postoperative period was unrelated to the original procedure. This circumstance may be reported by using Modifier-79 (Unrelated Procedure or Service by the Same Physician or Other Qualified Health Care Professional During the Postoperative Period). Frequent use of this approach may increase the risk of audits. This applies to the other code families as well. When using multiple modalities on noncutaneous surfaces, it is appropriate to use site-specific codes when available. For example, in Case Vignette 2, lesions of “the arms, penis, and anus” are being treated. The arm lesions would be reported using Code 17110 (1–14 lesions) or Code 17111 (≥15 lesions), along with one of Codes 46900, 46910, 46916, 46917, 46922 or 46924 for anal lesions and one of Codes 54050, 54055, 54056, 54057, 54060, or 54065 for the penile lesions. If one mixes modalities for a given site, only one of the discrete modalities should be reported if they are separated out as they are for the anus and penis. This is analogous to the skin destruction codes where any method can be a mix of modalities. If the lesions are extensive as noted above, the appropriate extensive codes should be reported.
The best strategy is to be as specific as possible in coding, document thoroughly, and provide photos so a reviewer can understand the evidence the dermatologist is providing as to why, for example, the lesions are being called extensive.
Proper Documentation
Documentation is another crucial component of properly coding all services for reimbursement, including those provided for MC treatment. To make documentation bulletproof, particularly if making the case for “extensive” lesions, dermatologists should document the site(s) treated, specify the product(s) and modalities used, detail each step of treatment, and provide photographs. If a dermatologist is coding for extensive lesions, that exact word—extensive—should be used, rather than synonyms. Most auditors are not physicians, and they rely on descriptions in the chart matching those associated with the CPT code. If the dermatologist can provide adequate documentation to defend the coding, the auditor is likely to be satisfied. For example, one might write, “extensive widespread lesions too numerous to count” or “extensive lesions becoming almost confluent in the site.” If multiple site codes are used, make sure documentation refers to each site specifically. The more codes reported for a single diagnosis on a given patient on a given day would likely correlate with an increased risk of audit. Creative coding, such as reporting multiple codes in the same body region (e.g., mixes of codes 46900–46924) can make you a person of interest, as can billing penis destruction codes for woman or vaginal or vulva codes for a man.
Coding Destructive Modalities in MC Treatment
The destructive modalities for MC lesions of the skin per CPT Code 2021 are defined as the “ablation of benign tissues” by any method, with or without curettement, including local anesthesia and not usually requiring closure. When it comes to coding, skin lesion destructions are reimbursed at set dollar amounts, regardless of modality used, to encourage providers to use the most cost-efficient means to remove MC, but this distinction changes for some noncutaneous sites. Most dermatologists are familiar with, and frequently use, Codes 17110 and 17111—the so-called “skin codes”—for the destruction of benign lesions. The Code 17110 is a base code, meaning it pays for treating multiple lesions (up to 14) in one session. If a dermatologist is treating 15 or more lesions, then Code 17111 is used, which pays somewhat more. Note again that Codes 17110 and 17111 are mutually exclusive, meaning they cannot both be used for the same patient on the same day. However, some body locations have their own destruction codes, and it is generally advisable to use the more specific anatomically based code if appropriate. When it comes to coding, the general rule of thumb is the more specific the code, the better (Table 1).
If a dermatologist is treating multiple MC lesions in regions that CPT coding categorizes as anatomically distinct, multiple codes may be applied. However, when multiple treatments are carried out in one anatomical region, only one code may be applied. For example, codes pertaining to the vulva are grouped under simple or extensive, and there are different code groupings for vulva versus vagina (i.e., a dermatologist treating MC in the vulvar region and the vagina may use both codes). When linking to an ICD-10 diagnostic code, B08.1 is the only code for the diagnosis of MC, and this code is anatomic-site agnostic, meaning one does not need site specificity, unlike many other skin diseases.
All destruction codes have qualified healthcare provider “work” defined to include application of a product. Qualified healthcare providers include physicians, nurse practitioners, and physician assistants, but it is not clear if nonqualified healthcare providers are allowed to apply the chemical products. State regulations define the scope of practice for various healthcare providers, so dermatologists should check with their individual state medical boards.
Conclusion
It can be challenging to keep up with billing and coding; however, understanding these systems makes a practice more efficient. While Codes 17110 and 17111 are the “skin codes,” the most specific anatomical codes available should be used when reporting MC treatment services, of which there are several if lesions are treated in these areas. Terminology should be auditor-friendly and consistent. Extensive lesions must be documented in detail, ideally with photographs. J codes can be reported for supplies and drugs, but there are currently no J codes that may be separately reported for topical products used in conjunction with a destruction code for MC. It is good coding practice to document each treatment step and modality precisely when treating patients with MC, and to provide photographic documentation as well.
Acknowledgments
The authors wish to acknowledge LeQ Medical in Angleton, Texas, for their support in preparing this manuscript.
References
- American Medical Association. CPT® overview and code approval. https://www.ama-assn.org/practice-management/cpt/cpt-overview-and-code-approval. Accessed 2 Aug 2023.
- American Medical Association. RBRVS overview. https://www.ama-assn.org/about/rvs-update-committee-ruc/rbrvs-overview#:~:text=The%20resource%2Dbased%20relative%20value,CMS)%20and%20most%20other%20payers.&text=In%20this%20system%2C%20payments%20are,Physician%20work. Accessed 2 Aug 2023.
- American Medical Association. 2021 RVS Update Process. https://www.ama-assn.org/system/files/ruc-update-booklet.pdf. Accessed 2 Aug 2023.
- United States Centers for Medicare and Medicaid Services. National Correct Coding Initiative. CMS.gov. Medicare Web site. https://www.cms.gov/medicare-medicaid-coordination/national-correct-coding-initiative-ncci#:~:text=The%20Centers%20for%20Medicare%20%26%20Medicaid,Part%20B%20and%20Medicaid%20claims. Published 2021. Accessed 2 Aug 2023.
- United States Centers for Medicare and Medicaid Services. NCCI FAQs. CMS.gov. National Correct Coding Initiative Edits Web site. https://www.cms.gov/medicare-medicaid-coordination/national-correct-coding-initiative-ncci/ncci-medicare/medicare-ncci-faq-library. Published 2021. Accessed 2 Aug 2023.