J Clin Aesthet Dermatol. 2026;19(3–4 Suppl 1):S20–S22.
by Timothy Kelly, CRNP
Mr. Kelly is with Dedicated Dermatology, East Stroudsburg, Pennsylvania.
Funding: No funding was provided for this article.
Disclosures: Writing support was provided by Arcutis Biotherapeutics Inc.
ABSTRACT: This case series describes the treatment of 2 patients with chronic plaque psoriasis refractory to conventional topical corticosteroid therapy. Both patients declined additional topical and systemic treatments and were subsequently treated monotherapy with a 1,064nm neodymium-doped yttrium aluminium garnet laser (Aerolase Neo Elite; Aerolase, Tarrytown, New York). When pruritus returned and worsened, both subjects trialed roflumilast cream 0.3% as combination therapy alongside the ongoing laser treatments. The addition of roflumilast cream greatly improved each of their symptoms, ultimately leading to resolution of pruritus and significant improvement of plaque size and texture. Keywords: Laser therapy, topical, roflumilast, plaque psoriasis
Introduction
Psoriasis is a chronic and persistent immune-mediated disease that affects millions of people worldwide and 3% of adults in the United States (US).1 Over 2% of the world’s population has psoriasis, with the highest prevalence rates seen in North America and Europe.2 Plaque psoriasis is the most prevalent form, representing 80% to 90% of cases. Other variants include guttate, inverse, pustular, erythrodermic, and nail psoriasis, each exhibiting distinct clinical features.2,3 The etiology of psoriasis is not fully known, but current evidence supports a multifactorial pathogenesis involving genetic predisposition and environmental factors leading to immune system dysregulation and keratinocyte hyperproliferation.2,3 Known exacerbating factors include physical trauma to the skin, infections, certain medications, and psychological stress. Modifiable risk factors, particularly smoking and obesity, have been identified as significant contributors to disease onset and progression.2
The progression of psoriasis is unpredictable, varying from intermittent flares to chronic, persistently active disease.2 This variability necessitates personalized treatment approaches based on disease severity, psoriasis subtype, involvement of sensitive areas, and patient-specific factors including age, comorbidities, and treatment preferences.2 Intertriginous psoriasis affects approximately 20% to 30% of patients, manifesting in skin folds (inframammary, axillary, inguinal, intergluteal)4,5 with characteristically erythematous, smooth plaques that lack the classic scale of plaque psoriasis.5,6 As one of the most prevalent chronic inflammatory dermatologic conditions affecting the geriatric population, psoriasis is frequently associated with comorbidities.7 Associated conditions include psoriatic arthritis, cardiometabolic diseases (hypertension, hyperlipidemia, type 2 diabetes), autoimmune disorders, and mental health conditions.1,3,7 While topical therapies remain first-line, either as monotherapy or in combination with targeted phototherapy, their limitations might lead to inadequate disease control with persistent physical discomfort and decreased quality of life.3,5,7 In elderly patients with psoriasis, the risk of polypharmacy and complex comorbidities demands thorough evaluation when considering systemic or biologic agents.7 In recent years, there have been new topical therapies approved by the US Food and Drug Administration (FDA) to treat psoriasis. One of them, roflumilast cream 0.3%, is a steroid-free, highly selective, potent topical phosphodiesterase-4 (PDE4) inhibitor that is not immunosuppressive and was approved by the FDA in 2022 for the treatment of psoriasis, including intertriginous areas, and in 2023 in a foam formulation for the treatment of seborrheic dermatitis. Additionally, roflumilast cream 0.15% was approved in 2024 for the treatment of atopic dermatitis, and roflumilast foam 0.3% was approved in 2025 for the treatment of plaque psoriasis of the scalp and body.
This case series presents the cases of 2 older female patients with thick chronic plaque psoriasis on tough-to-treat areas of the sacral region and lower extremities that was refractory to conventional topical corticosteroid therapy. Both patients declined additional topical and systemic treatments and were subsequently treated monotherapy with a 1,064nm neodymium-doped yttrium aluminium garnet (Nd:YAG) laser (Aerolase Neo Elite; Aerolase, Tarrytown, New York). When pruritus returned and worsened, both subjects trialed roflumilast cream 0.3% as combination therapy alongside the ongoing laser treatments. The addition of roflumilast cream greatly improved each of their symptoms, ultimately leading to resolution of pruritus and significant improvement of plaque size and texture.
Case Series
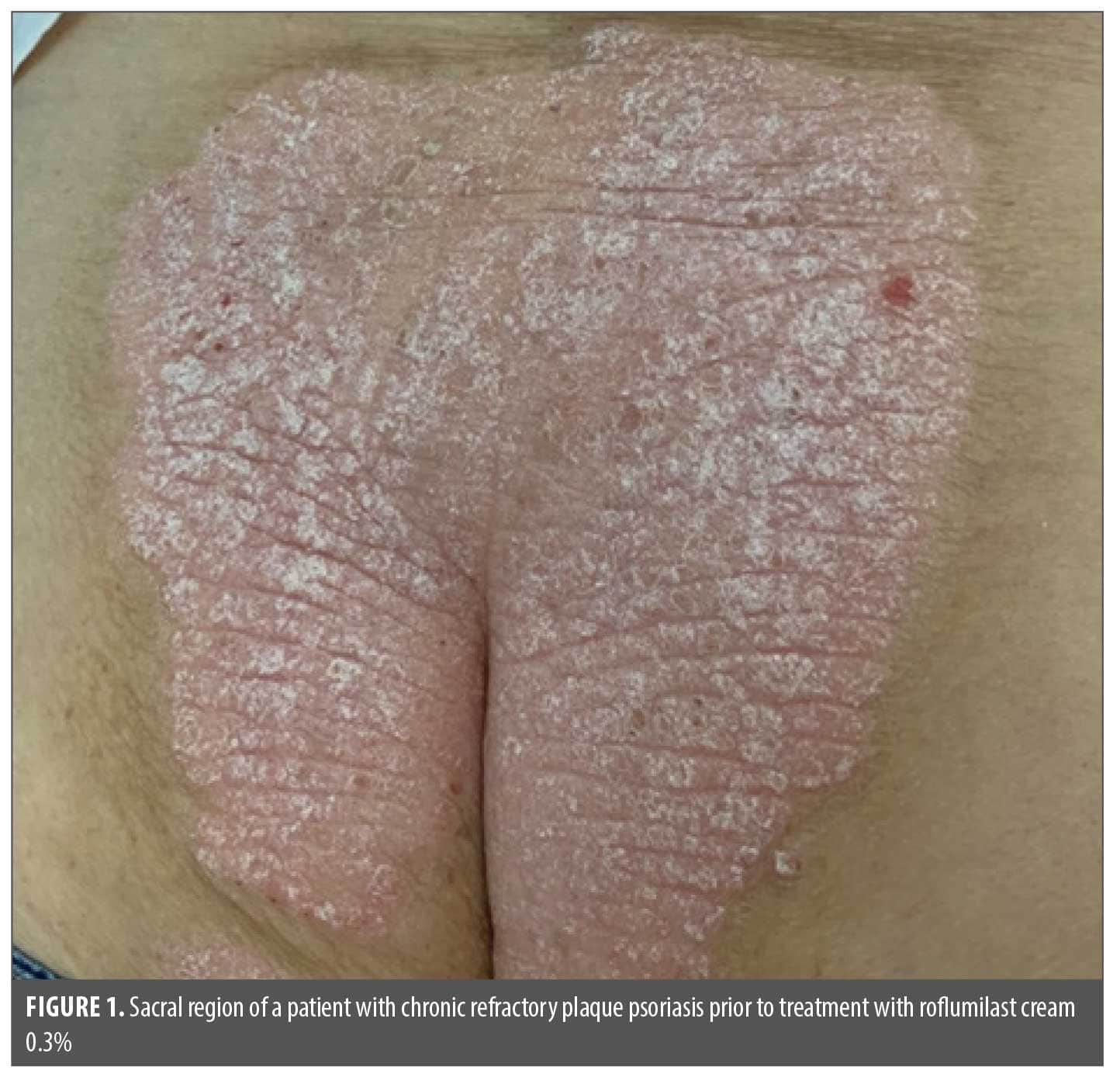
Case 1. The first patient, a 90-year-old female individual with a 3-year history of chronic plaque psoriasis, presented with a plaque involving the sacral region and intertriginous fold. Initially evaluated by an outside provider in 2021, her psoriasis Physician Global Assessment (PGA) score was 4.0 (severe), with 10% total body surface area (BSA) involvement. High-potency topical corticosteroids were prescribed but failed to significantly reduce disease severity or BSA. Upon transitioning to our care in May 2023, the clinical assessment shifted to the Itch Numeric Rating Scale (NRS), at which time she reported moderate pruritus (6/10) and an increased BSA of 12%. Despite prior inadequate response to topical therapy, she declined systemic (oral or injectable) therapies. Given her preference for nonsystemic treatment, we initiated 1,064nm Nd:YAG laser therapy as monotherapy, leveraging its anti-inflammatory properties and ability to target dermal vasculature. The patient underwent monthly laser treatments from June 2023 through November 2024, and although these treatments were maintained for 18 months, persistent plaque morphology was observed.
Following missed appointments due to illness and inclement weather, the patient returned in April 2025 with recurrent pruritus (NRS: 4/10) and measured BSA involvement of 10% (Figure 1). Still averse to systemic therapies, she was offered a trial of topical roflumilast cream 0.3%, a steroid-free PDE4 inhibitor with a favorable safety profile. Roflumilast cream is approved for plaque psoriasis, with a unique distinction as the first topical therapy also specifically indicated for intertriginous involvement—a setting where traditional treatments often fail. Clinical trials including roflumilast cream 0.3% reported the most common adverse events in ≥1% of patients, with the most common being diarrhea, headache, insomnia, application site pain, upper respiratory tract infections, and urinary tract infections.8 Informed consent was obtained after reviewing possible adverse effects.
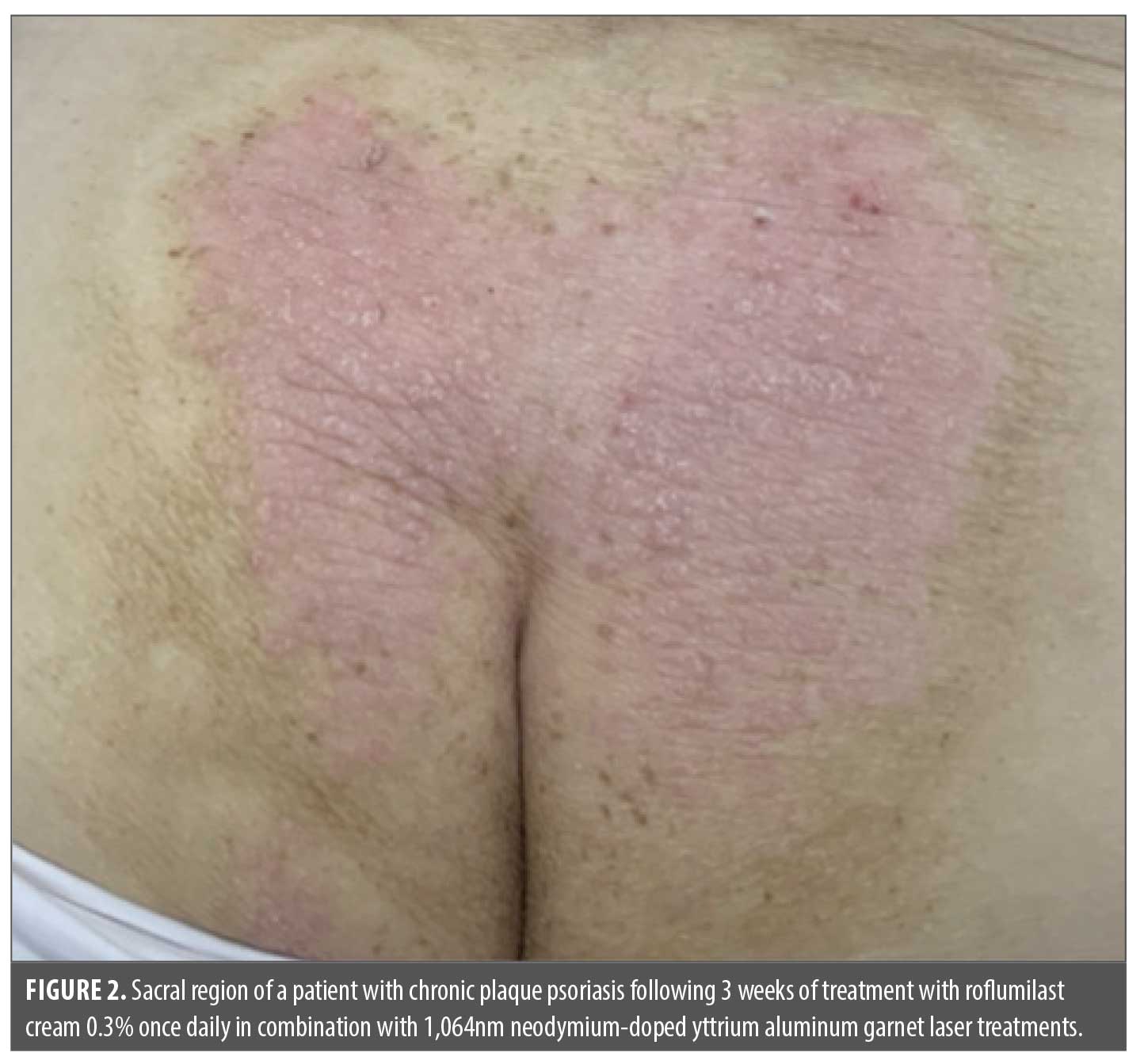
By her follow-up on April 23, 2025, she reported complete pruritus resolution (NRS: 0/10) following roflumilast initiation. Clinical examination demonstrated significant reduction in plaque size, erythema, and scaling, with a reduction in affected BSA to 8% (Figure 2). The patient expressed satisfaction with the treatment and elected to continue concurrent 1,064nm Nd:YAG laser therapy and daily topical roflumilast application. No adverse events were observed, and no contraindications to combination therapy were identified.
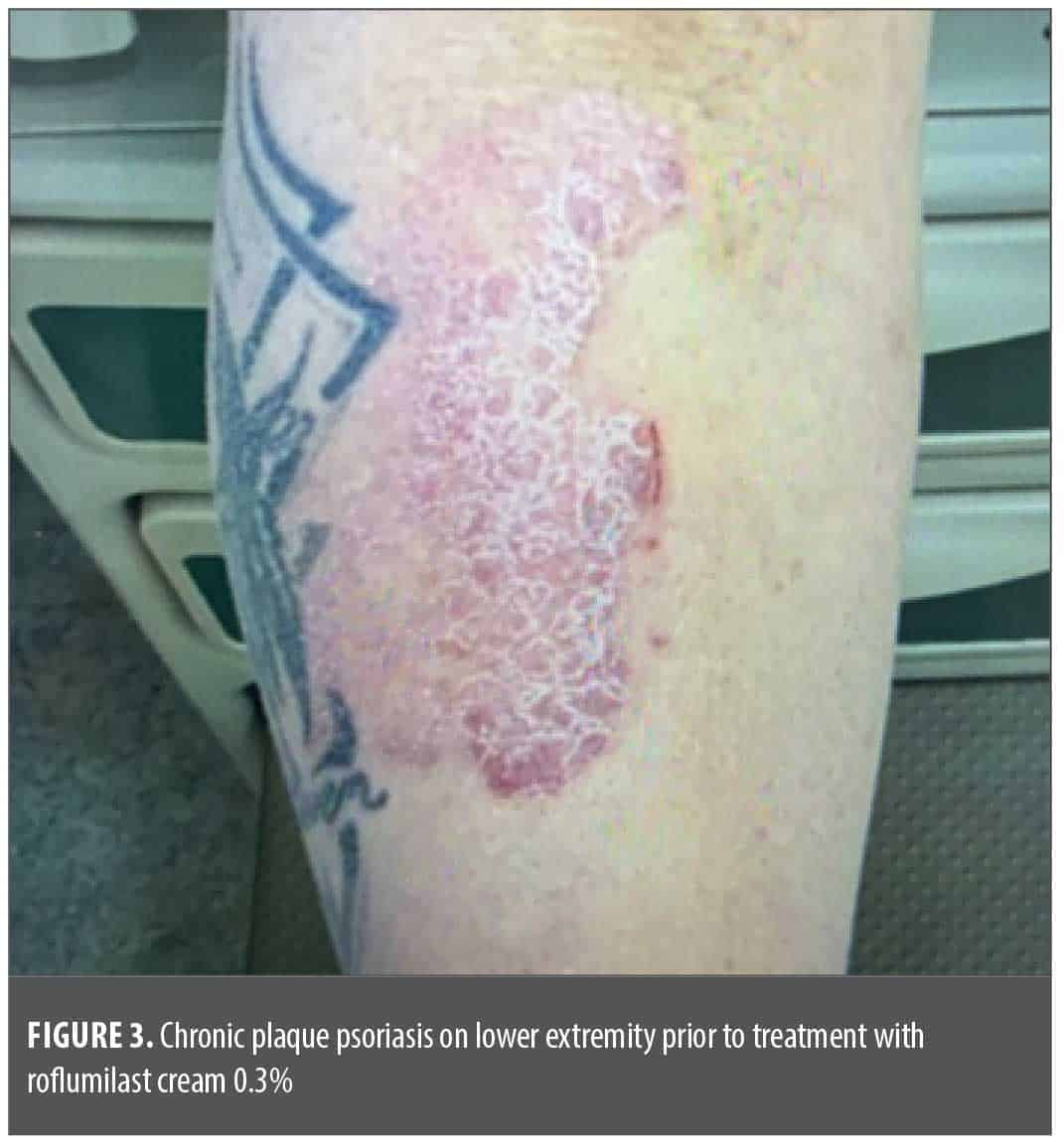
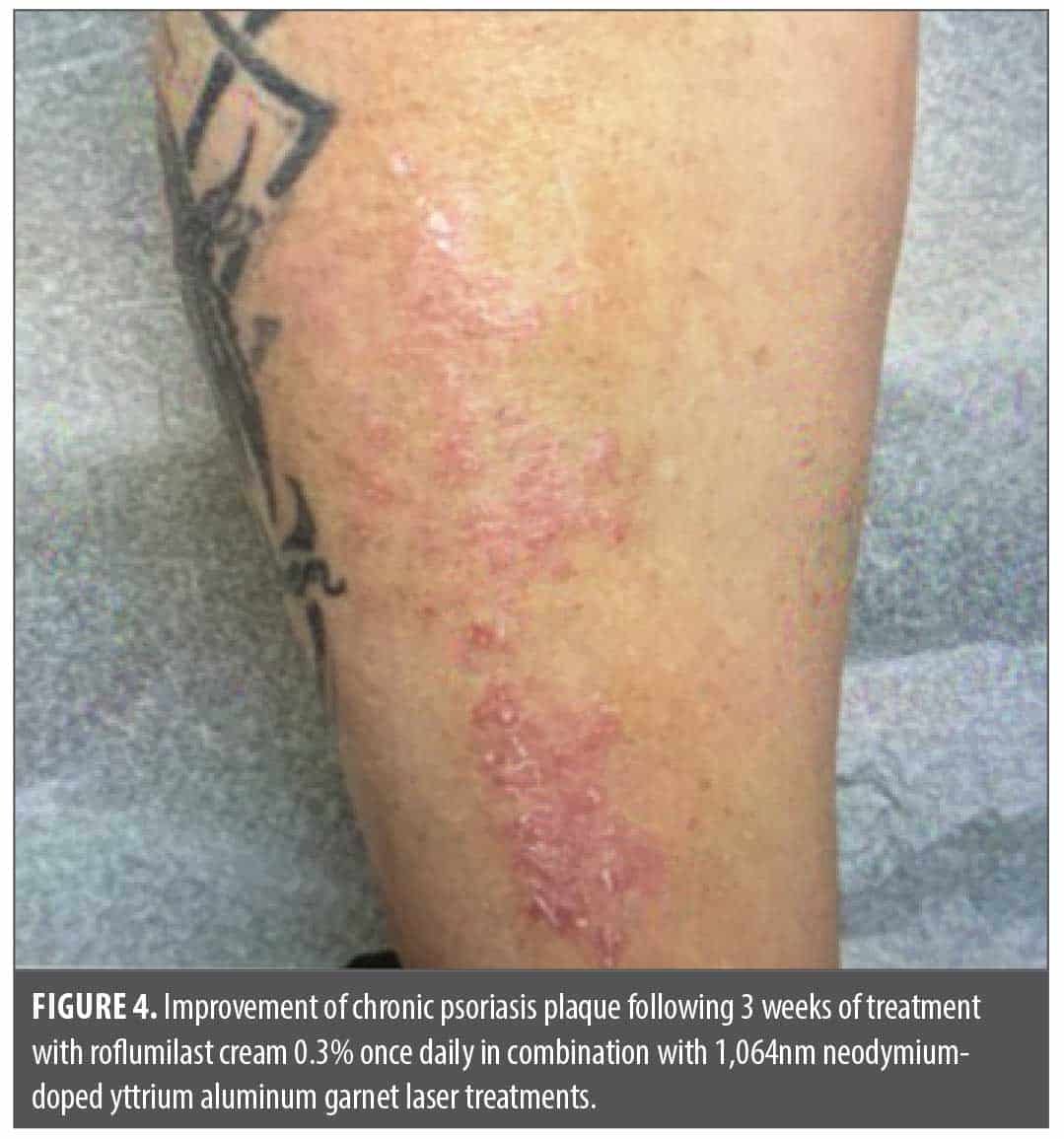
Case 2. In the second case, a 62-year-old female patient with a 3-year history of chronic plaque psoriasis on her right lower extremity and left knee, presented to the clinic with PGA score of 3.0 (moderate), 5% total BSA involvement, and significant itch (NRS: 8/10; Figure 3). She was initially prescribed clobetasol and calcipotriene to apply topically, but she was not consistent with treatment application and was not interested in any other topical, oral, or injectable medications. Eight months passed before she returned to the office, at which point treatment options were thoroughly discussed, and she chose to begin monotherapy treatment with the 1,064nm Nd:YAG laser. Six weeks later, at her second laser treatment, she reported improvement in pruritus (NRS: 2/10) and PGA score of 2.0 (mild). Over the next year and a half, her appointments for laser treatment were very inconsistent, and she returned to clinic almost a year after her fourth laser treatment when her itch became worse. When she presented for her fifth laser treatment, PGA score was 2.0 (mild), and pruritus had increased (NRS: 4/10). After a lengthy discussion with the patient, she was given a sample of roflumilast cream 0.3% to use once daily in combination with continued laser treatments. She returned 3 weeks later for her sixth laser treatment and stated that she had been using roflumilast cream nightly. She reported that pruritus had completely resolved (NRS: 0/10) and her psoriasis plaques were almost clear (PGA: 1.0) as seen in Figure 4. Returning 12 weeks later for her seventh laser treatment, she reported sustained itch relief/resolution (NRS: 0/10), and psoriasis remained almost clear (PGA: 1.0). She commented that out of all the topical medications she has used in the past, roflumilast cream was the only one to provide lasting relief.
Both patients remain highly satisfied with their current treatment regimens, reporting sustained symptomatic relief and visible improvement of plaque size and texture.
Conclusion
This case series describes 2 female patients with moderate pruritus and chronic psoriasis plaques in tough-to-treat areas that were refractory to topical corticosteroids. Both patients experienced successful symptom control and clinical improvement with roflumilast cream 0.3% in combination with 1,064nm Nd:YAG laser therapy. This case highlights the utility and safety of roflumilast cream, a novel and effective PDE4 inhibitor, combined with targeted laser therapy in the senior population, particularly those who are not candidates for systemic agents and have limited treatment options. The combination regimen was well tolerated in both cases with no reported adverse events, while demonstrating sustained pruritus relief and marked regression of refractory, thickened plaques on the knee and lower extremity as well as the tough-to-treat intertriginous area of the sacrum. Further clinical studies are needed to assess the therapeutic potential and safety of topical roflumilast in combination with laser treatment.
References
- Armstrong AW, Mehta MD, Schupp CW, et al. Psoriasis prevalence in adults in the United States. JAMA Dermatol. 2021;157(8):940–946.
- Chakith MRS, Pradeep S, Gangadhar M, et al. Advancements in understanding and treating psoriasis: a comprehensive review of pathophysiology, diagnosis, and therapeutic approaches. PeerJ. 2025;13:e19325.
- Armstrong AW, Read C. Pathophysiology, clinical presentation, and treatment of psoriasis. JAMA Dermatol. 2020;323(19):1945–1960.
- Aldredge LM, Higham RC. Manifestations and management of difficult-to-treat psoriasis. J Dermatology Nurses Assoc. 2018;10(4):189–197.
- Hong JJ, Mosca ML, Hadeler EK, et al. Genital and inverse/intertriginous psoriasis: an updated review of therapies and recommendations for practical management. Dermatol Ther (Heidelb). 2021;11(3):833–844.
- Dopytalska K, Sobolewski P, Błaszczak A, et al. Psoriasis in special localizations. Reumatologia. 2018;56(6):392–398.
- Çalışkan E, Edek YC, Keskin N, et al. Geriatric psoriasis: evaluation of clinical features, disease course, and treatment modalities of patients from a tertiary care hospital. Dermatol Pract Concept. 2025;15(1):4511.
- ZORYVE (roflumilast) topical cream [prescribing information]. Westlake Village, CA: Arcutis Biotherapeutics; Jul 2024. Accessed 4 Aug 2025. https://www.arcutis.com/wp-content/uploads/USPI-roflumilast-cream.pdf