J Clin Aesthet Dermatol. 2019;12(3):28–31
 by Alison Kang, MD; Alexis Lyons, MD; Jennifer Herrmann, MD; and Ronald Moy, MD
by Alison Kang, MD; Alexis Lyons, MD; Jennifer Herrmann, MD; and Ronald Moy, MD
Drs. Kang and Herrmann are with the Division of Dermatology, Harbor-UCLA Medical Center in Torrance, California. Drs. Lyons, Herrmann, and Moy are with Moy-Fincher-Chipps Facial Plastics and Dermatology in Beverly Hills, California. Dr. Moy is with the Department of Dermatology, Keck School of Medicine at the University of Southern California in Los Angeles, California.
FUNDING: No funding was received for this study.
DISCLOSURES: The authors have no conflicts of interest relevant to the content of this article.
ABSTRACT: Objective. The objectives of this study were to evaluate the efficacy, safety and patient satisfaction of a unique combination of wavelengths 589nm and 1,319nm for the treatment of facial acne vulgaris.
Design. This was a small, randomized, prospective, split-face, single-blinded study of patients with moderate-to-severe acne vulgaris.
Setting.The study took place at a single outpatient center study in Torrance, California.
Participants. Nine patients underwent four treatment sessions at 2- to 3-week intervals. Each patient received one pass with the 1,319nm laser followed by one pass with the 589nm laser only to the randomized treatment side of the face.
Measurements. A blinded, board-certified dermatologist reviewed photographs and counted acne lesions on treated and nontreated sides.
Results. Of the nine patients, eight were Fitzpatrick Skin Type IV. At the final visit, inflammatory acne lesions were reduced by 2.5 (-23.1%) on the treatment side and increased by 1.1 (+11.1%) on the control side. No patients experienced bruising, edema, hyperpigmentation or scarring. At the conclusion of the study, 77.8 percent of the patients reported overall satisfaction.
Conclusion. This unique combination of lasers appears to be safe in patients with Fitzpatrick Skin Type IV, and might be useful in treating moderate-to-severe acne vulgaris.
KEYWORDS: Acne, acne vulgaris, active acne, acne scarring, laser
Introduction
Acne vulgaris is the most common skin condition in the United States, affecting up to 50 million Americans each year.1 Although most prevalent during the teenage years, acne often persists into adulthood and is more common in women than men.2 Acne affects all skin colors and can cause negative self-image, lower self-esteem, and feelings of isolation, anxiety, and depression.3 Scarring is a common complication of acne and has been reported in up to 95 percent of patients with acne.4
Standard medical treatments for acne include topical medications such as benzoyl peroxide, antibiotics, retinoids, and salicylic acid, as well as oral medications such as antibiotics, contraceptive pills, spironolactone, and isotretinoin.5–7 Treatments are individualized depending on acne severity, type, and etiology. Recently, there has been increasing recognition of laser- and light-based therapies for the treatment of active acne and resultant scarring.8,9 Lasers studied include the 1,540-nm erbium:glass laser, 1,550-nm fractionated erbium:glass laser, pulsed-dye laser (PDL), q-switched 1,064-nm neodymium-doped yttrium aluminium garnet (Nd:YAG) laser, fractional 1,320-nm Nd:YAG laser, 1,450-nm diode laser, and 532-nm potassium titanyl phosphate laser.8,9 In addition, the 1,450-nm diode laser has been shown to reduce sebum production.10
To date, few studies have investigated laser combinations, including PDL combined with either a 1,064-nm Nd:YAG or a 1,450-nm diode laser.11–13 The device investigated in this study is a unique, solid-state laser with both 589-nm and 1,319-nm wavelengths. The 589-nm wavelength targets the superficial cutaneous microvasculature and might reduce acne-associated erythema,14–16 while the 1,319-nm wavelength is absorbed primarily by water, generating thermal energy nonspecifically, leading to dermal collagen remodelling.21 Studies evaluating the 1,320-nm wavelength have demonstrated histologic improvement in epidermal and dermal thickening as well as acne scar improvement.17–24 In addition, the 1,319-nm wavelength might also target the sebaceous gland directly, leading to reduced sebum production.25
The primary objective of this study was to evaluate the efficacy of a unique combination of the 589-nm and 1,319-nm wavelengths for the treatment of facial acne vulgaris. The secondary objectives of this study were to assess the safety of this combination of lasers in patients with Fitzpatrick Skin Type IV and to evaluate overall patient satisfaction.
Materials and Methods
A randomized, prospective, split-face, single-blinded study was performed at a single center in Torrance, California. Participants were at least 16 years of age, with Fitzpatrick Skin Types I to IV and moderate-to-severe inflammatory acne, and were required to provide informed assent/consent. Informed consent was provided by a legal guardian for participants under the age of 18 years. Exclusion criteria included the initiation of new topical or oral acne therapy within the previous three months, history of oral retinoid therapy, history of other laser treatments, dermabrasion, or other methods to treat scars, and pregnancy. This small study was performed in accordance with the 2013 revision of the Declaration of Helsinki. Informed assent/consent was obtained from all individual participants included in the study. Photo consent was obtained from participants. Moderate-to-severe acne was defined for our study as having at least four inflammatory papules or pustules on each half of the face.
Each patient was randomized to receive treatment on either the left or the right side of the face. Out of nine total participants, five (55.6%) patients were randomized to receive treatment on the left half of the face and four (44.4%) were randomized to receive treatment on the right half of the face. Patients underwent four treatment sessions at 2- to 3-week intervals. Each patient received one pass with the 1,319-nm laser followed by one pass with the 589-nm laser only to the randomized treatment side of the face. Laser settings were chosen based on patient skin type and tolerability ranging from 16 to 19mJ/cm2 for the 1,319-nm setting and 14 to 17mJ/cm2 for the 589-nm setting. Commercially available ice packs and cooling gel were used for improved patient comfort during the treatment with the 589-nm laser. Photographs were taken at each visit prior to the treatment. Patients were followed for up to 5.4 weeks after their final treatment, and final post-treatment photographs were obtained. A poststudy patient survey was conducted to assess subjective perceived improvement of four metrics: skin texture, redness, oiliness, and scarring. In addition, patients were asked to report any experienced discomfort and their overall satisfaction. At the conclusion of all laser treatments, a blinded board-certified dermatologist reviewed photographs and counted acne lesions on treated and nontreated sides.
Results
 A total of nine patients who fulfilled the inclusion criteria were enrolled in and completed the study. No participants dropped out or failed to follow up appropriately for study visits. There were seven (77.8%) women and two (22.2%) men between the ages of 17 and 40 years (median age: 23 years). One (11.1%) patient had a Fitzpatrick Skin Type II and eight (88.9%) patients had Fitzpatrick Skin Type IV. The demographic characteristics of the nine patients are summarized in Table 1.
A total of nine patients who fulfilled the inclusion criteria were enrolled in and completed the study. No participants dropped out or failed to follow up appropriately for study visits. There were seven (77.8%) women and two (22.2%) men between the ages of 17 and 40 years (median age: 23 years). One (11.1%) patient had a Fitzpatrick Skin Type II and eight (88.9%) patients had Fitzpatrick Skin Type IV. The demographic characteristics of the nine patients are summarized in Table 1.
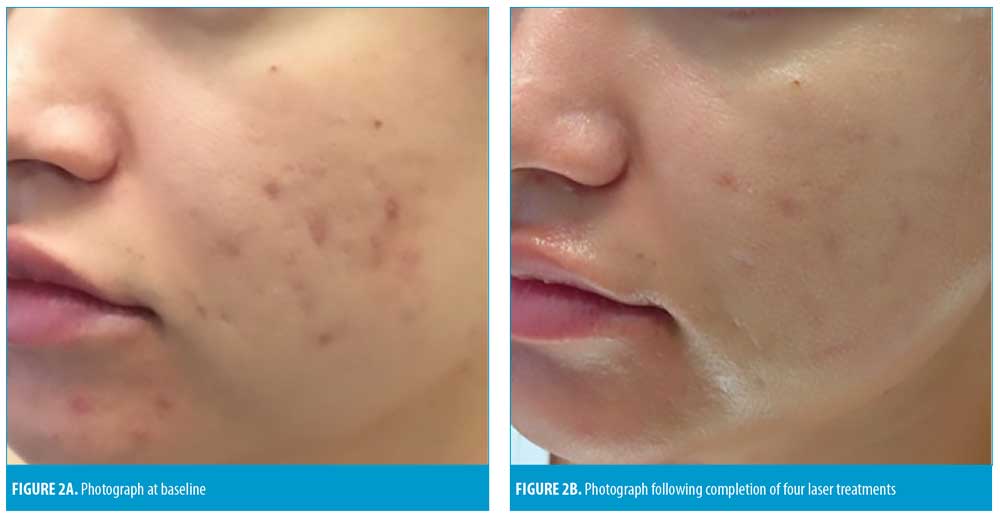
Average baseline inflammatory acne lesion count was 11.1 on the treatment side and 10.3 on the control side. Reduction in acne lesion count was noted in 57.1 percent of patients after the first treatment session. However, between the first and second treatments, these improvements were not sustained, with some patients experiencing an increase in acne lesions. After the second treatment, 40 percent of patients experienced a reduction in acne lesions counts. After the third and fourth treatments, 57.1 and 85.7 percent of the patients showed improvement, respectively. At the final visit, inflammatory acne lesions were reduced by 2.5 (-23.1%) on the treatment side and increased by 1.1 (+11.1%) on the control side. Two patients experienced increased acne counts on both sides of the face. Representative photographs of patients treated in the study are shown in Figures 1A–B and 2A–B. The efficacy of the laser treatments was noted to be sustained for up to 5.4 weeks following the final treatment session, which was the longest follow-up period in this study. All nine patients completed the survey at the completion of the study; 77.8 percent of patients reported overall satisfaction with the results of the laser treatments. Patients were asked to rate their degree of improvement on a linear scale, with 0=no improvement and 10=very significant improvement. Average and median scores were 4.9 and 7 points, respectively, for subjective evaluation of response to treatment. Specifically, patients reported an improvement in skin texture (6/9, 66.7%), scarring (4/9, 44.4%), redness (6/9, 66.7%), and oiliness (7/9, 77.8%). Finally, patients were asked to rate their level of discomfort during the laser treatments from the following choices: none, mild, moderate, or severe. One patient reported none, five patients reported mild discomfort, and three patients reported moderate discomfort. No patients reported severe discomfort. All patients developed transient post-treatment erythema that resolved completely within 24 hours. No patients experienced bruising, edema, hyperpigmentation, or scarring.


Discussion
Recently, laser- and light-based therapies have emerged as popular options for the management of active acne and acne scarring. These modalities can be used as adjunct therapy to conventional acne treatments or as monotherapy.26 Laser therapy is advantageous because it is an in-office treatment, which ensures patient adherence to therapy. In addition, it offers no systemic side effects that might complicate treatment when using oral acne medications. Although many different lasers have been studied for the treatment of acne, only a few studies to date have have evaluated a combination of lasers, which include PDL with either a 1,064-nm Nd:YAG or a 1,450-nm diode laser.11–13
Our research is unique in that it studied a novel, solid-state laser with both 589-nm and 1,319-nm wavelengths available in the single device. To our knowledge, no similar combination of wavelengths has been studied previously. We found that more than half of our patients had temporarily reduced acne lesion counts after only one session, and 85.7 percent of the patients showed improvement after four sessions, which was sustained through the follow-up period (5.4 weeks). These results might be due to effects on the sebaceous gland. The 1,319-nm wavelength might target the sebaceous gland directly and reduce sebum production, similar to the sebum reducing effects that have been observed in the 1,450-nm diode laser.10 However, further studies are necessary to assess the effects of the 1,319-nm wavelength on sebaceous gland activity and sebum production. In addition, 66.7 percent of the patients reported an improvement in redness. This might be explained by the 589-nm wavelength, which has been shown in other studies to improve acne-associated erythema.14–16 Improvement in erythema in a representative patient can be seen in Figures 1A–B.
It is noteworthy that treatment with this combination of laser wavelengths was generally well-tolerated and led to high patient satisfaction. Future studies that investigate the optimal frequency of treatments and assess duration and long-term efficacy are warranted. Furthermore, it would be interesting to study the role of this laser as an adjunct therapy to conventional acne treatments or in combination with chemical peels.
Limitations. This study is limited by its small sample size, modest improvement, and short follow-up times to assess duration and long-term efficacy.
Conclusion
This unique combination lasers appears to be safe in Fitzpatrick Skin Type IV patients and might be useful in treating moderate-to-severe acne vulgaris.
References
- Bickers DR, Lim HW, Margolis D et al. The burden of skin diseases: 2004 a joint project of the American Academy of Dermatology Association and the Society for Investigative Dermatology. J Am Acad Dermatol. 2006;55(3):490–500.
- Collier CN, Harper JC, Cafardi JA, et al. The prevalence of acne in adults 20 years and older. J Am Acad Dermatol. 2008;58(1):56–59.
- Dalgard F, Gieler U, Holm J, et al. Self-esteem and body satisfaction among late adolescents with acne: results from a population survey. J Am Acad Dermatol. 2008;59(5):746–751.
- Layton AM, Henderson CA, Cunliffe WJ. A clinical evaluation of acne scarring and its incidence. Clin Exp Dermatol. 1994;19(4):303–308.
- Arowojolu AO, Gallo MF, Lopez LM, et al. Combined oral contraceptive pills for treatment of acne. Cochrane Database Syst Rev. 2012;(7):CD004425.
- Bhate K, Williams HC. What’s new in acne? An analysis of systematic reviews published in 2011–2012. Clin Exp Dermatol. 2014;39(3):273–277.
- Zaenglein AL, Pathy AL, Schlosser BJ, et al. Guidelines of care for the management of acne vulgaris. J Am Acad Dermatol. 2016;74(5): 945–973.e33.
- Wiznia LE, Stevenson ML, Nagler AR. Laser treatments of active acne. Lasers Med Sci. 2017;32(7):1647–1658.
- Barbaric J, Abbott R, Posadzki P, et al. Light therapies for acne. Cochrane Database Syst Rev. 2016;(9):CD007917.
- Laubach HJ, Astner S, Watanabe K, et al. Effects of a 1,450 nm diode laser on facial sebum excretion. Lasers Surg Med. 2009;41(2):110–115.
- Glaich AS, Friedman PM, Jih MH, et al. Treatment of inflammatory facial acne vulgaris with combination 595-nm pulsed-dye laser with dynamic-cooling-device and 1,450-nm diode laser. Lasers Surg Med. 2006;38(3):177–180.
- Jung JY, Choi YS, Yoon MY, et al. Comparison of a pulsed dye laser and a combined 585/1,064-nm laser in the treatment of acne vulgaris. Dermatol Surg. 2009;35(8):1181–1187.
- Salah el din MM, Samy NA, Salem AE. Comparison of pulsed dye laser versus combined pulsed dye laser and Nd: YAG laser in the treatment of inflammatory acne vulgaris. J Cosmet Laser Ther. 2017;19(3):149–159.
- Yoon HJ, Lee DH, Kim SO, et al. Acne erythema improvement by long-pulsed 595-nm pulsed-dye laser treatment: a pilot study. J Dermatolog Treat. 2008;19(1):38–44.
- Leheta TM. Role of the 585-nm pulsed dye laser in the treatment of acne in comparison with other topical therapeutic modalities. J Cosmet Laser Ther. 2009;11(2):118–124.
- Park KY, Ko EJ, Seo SJ, et al. Comparison of fractional, nonablative, 1550-nm laser and 595-nm pulsed dye laser for the treatment of facial erythema resulting from acne: a split-face, evaluator-blinded, randomized pilot study. J Cosmet Laser Ther. 2014;16(3):120–123.
- Bellew SG, Lee C, Weiss MA, et al. Improvement of atrophic acne scars with a 1,320 nm Nd:YAG laser: retrospective study. Dermatol Surg. 2005;31(9 Pt 2):1218–1221.
- Bhatia AC, Dover JS, Arndt KA, et al. Patient satisfaction and reported long-term therapeutic efficacy associated with 1,320 nm Nd:YAG laser treatment of acne scarring and photoaging. Dermatol Surg. 2006;32(3):346–352.
- Chan HH, Lam LK, Wong DS, et al. Use of 1,320 nm Nd:YAG laser for wrinkle reduction and the treatment of atrophic acne scarring in Asians. Lasers Surg Med. 2004;34(2):98–103.
- Rogachefsky AS, Hussain M, Goldberg DJ. Atrophic and a mixed pattern of acne scars improved with a 1320-nm Nd:YAG laser. Dermatol Surg. 2003;29(9):904–908.
- Sadick NS, Schecter AK. A preliminary study of utilization of the 1320-nm Nd:YAG laser for the treatment of acne scarring. Dermatol Surg. 2004;30(7):995–1000.
- Goldberg DJ. Non-ablative subsurface remodeling: clinical and histologic evaluation of a 1320-nm Nd:YAG laser. J Cutan Laser Ther. 1999;1(3): 153–157.
- Goldberg DJ. Full-face nonablative dermal remodeling with a 1320 nm Nd:YAG laser. Dermatol Surg. 2000;26(10):915–918.
- Tanzi EL, Alster TS. Comparison of a 1450-nm diode laser and a 1320-nm Nd:YAG laser in the treatment of atrophic facial scars: a prospective clinical and histologic study. Dermatol Surg. 2004;30(2 Pt 1):152–157.
- Orringer JS, Kang S, Maier L, et al. A randomized, controlled, split-face clinical trial of 1320-nm Nd:YAG laser therapy in the treatment of acne vulgaris. J Am Acad Dermatol. 2007;56(3): 432–438.
- Thiboutot D, Gollnick H, Bettoli V, et al. New insights into the management of acne: An update from the global alliance to improve outcomes in acne group. J Am Acad Dermatol. 2009;60(5 Suppl):S1–S50.
