J Clin Aesthet Dermatol. 2026;19(2):22–25.
by Aaron Cheng, BA, BS; Justin Guzman; and David G. Cotter, MD, PhD
Mr. Cheng is with the Long School of Medicine at the University of Texas Health San Antonio in San Antonio, Texas. Mr. Guzman is with the University of Nevada Reno in Reno, Nevada. Dr. Cotter is with Las Vegas Dermatology in Las Vegas, Nevada, and University of Nevada Las Vegas School of Medicine in Las Vegas, Nevada.
FUNDING: No funding was provided for this article.
DISCLOSURES: The authors have no conflict of interest to declare.
ABSTRACT: A “blueberry muffin rash,” typically attributed to congenital toxoplasmosis, rubella, cytomegalovirus, and herpes simplex virus (TORCH) infections, is a rare and underreported cutaneous manifestation of serious underlying pathology, including hematologic malignancies. We report a case of congenital acute myeloid leukemia (AML) in a full-term newborn who presented at day-of-life 0 with multiple blue to purple macules, patches, and indurated papulonodules and plaques on the trunk and extremities consistent with a “blueberry muffin rash”. Notably, the rash was transient and spontaneously resolved within 24 hours of life, making it easy to overlook, potentially delaying life-saving treatment. This case reinforces the need for a full diagnostic workup and high clinical suspicion for leukemia in neonates presenting with a “blueberry muffin rash.” Keywords: Acute myeloid leukemia, blueberry muffin rash, congenital leukemia, leukemia cutis
Introduction
Congenital leukemia is an exceptionally rare condition that typically presents within the first few weeks of life.1 Leukemia cutis, a cutaneous infiltration by leukemic cells, is an unusual manifestation of congenital leukemia observed in only 25% to 30% of affected infants.2 Leukemia cutis may present with a “blueberry muffin rash,” characterized by widespread, blue-red or violaceous macules and papulonodules.3 This eruption is typically associated with congenital TORCH (ie, toxoplasmosis, other, rubella, cytomegalovirus, and herpes simplex virus [HSV]) infections rather than malignancy. Thus, early diagnosis of leukemia may be challenging.3 Herein, we report the case of a female newborn who initially presented with an extensive, transient violaceous cutaneous eruption suggestive of a blueberry muffin rash that was ultimately diagnosed as congenital leukemia cutis, along with her clinical evaluation, treatment, and clinical course. We also review previously reported cases of blueberry muffin rash exclusively linked to neonatal or congenital leukemia.
Case report
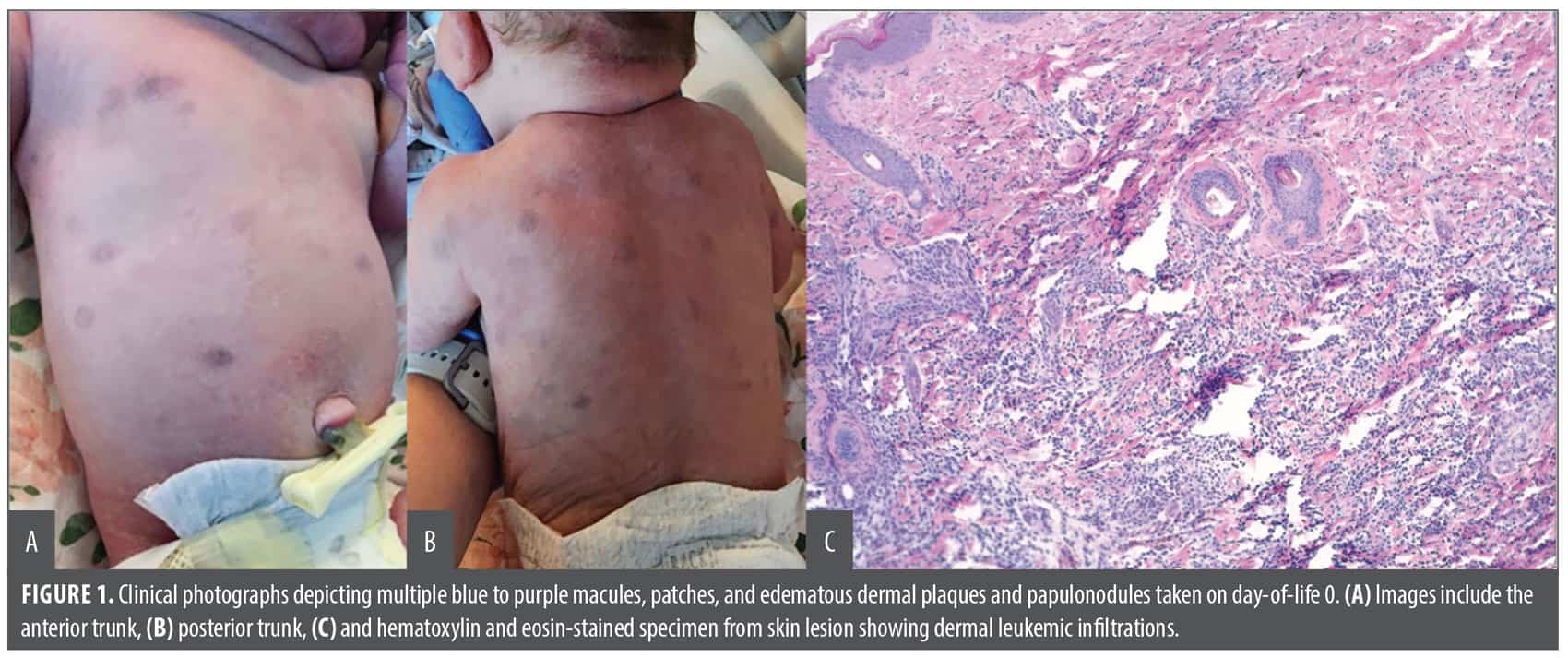
A newborn girl, born at 38 weeks, 1 day gestation via repeat cesarean delivery, presented at day-of-life 0 with multiple blue to purple macules, patches, and indurated papulonodules and plaques on the trunk and extremities (Figures 1A and 1B), resulting in a “blueberry muffin” appearance. On initial evaluation by dermatology, the patient appeared well with normal vital signs for her age and no other signs of systemic disease. No visible signs of respiratory distress or hemodynamic instability were noted on physical exam. Apgar score, birth weight and height, and head circumference were all within normal limits. Additionally, infectious studies were negative for cytomegalovirus, toxoplasmosis, syphilis, HSV-2, and the patient showed positive HSV-1 and rubella immunoglobulin G (IgG) titers.
A punch biopsy taken from a plaque on the patient’s back revealed an extensive dermal mononuclear infiltrate (Figure 1C). The cells were CD33 and CD68 positive, with a subset positive for myeloperoxidase (MPO) suggestive of acute myeloid leukemia (AML) with monocytic differentiation.
Further diagnostic workup, including bone marrow aspirates, revealed hypercellular marrow with maturing trilineage hematopoiesis, myeloid megakaryocytic hyperplasia, and an abnormal immature monocyte population consistent with AML. Interestingly, within 24 hours of the initial clinical presentation, the patient’s rash spontaneously resolved. The patient was treated with an intensified fludarabine, high-dose cytarabine, granulocyte colony-stimulating factor, idarubicin chemotherapy regimen with gemtuzumab ozogamicin (FLAG/Ida + GO) regimen and achieved complete remission. She continues to do well and shows no signs of active disease. A multidisciplinary team will provide ongoing monitoring for disease recurrence.
Discussion
The term “blueberry muffin baby” was first used during the American rubella epidemic in the 1960s to characterize the distinctive cutaneous manifestations of congenital rubella infections.3 The skin lesions result from extramedullary hematopoiesis, a process in which blood cells are produced outside of the bone marrow, and are typically triggered by congenital TORCH infections, hematologic dyscrasias (eg, hereditary spherocytosis, hemolytic disease of the newborn, twin-to-twin transfusion syndrome), or neoplasms (mastocytosis, histiocytosis, neuroblastoma, rhabdomyosarcoma, leukemia).3 Rarely, blueberry muffin rash has been associated with Langerhans cell histiocytosis and juvenile xanthogranuloma.4,5
We present a case of AML presenting as a transient blueberry muffin rash in a female newborn. Leukemia is the most commonly diagnosed malignancy in childhood and is most commonly reported in infants with Down syndrome.6,7 However, congenital leukemia is extremely rare, accounting for less than 1% of all reported cases of pediatric leukemia.8 The typical clinical presentation of AML in neonates includes anemia, bleeding, febrile neutropenia, lethargy, leukocytosis, central nervous system involvement, and hepatosplenomegaly.9 Additionally, leukemia cutis is a rare manifestation of congenital leukemia that can often mimic other conditions such as congenital TORCH infections.9 A blueberry muffin rash is an exceptionally unusual presentation of AML in neonates and can be easily mistaken for
other pathologies.
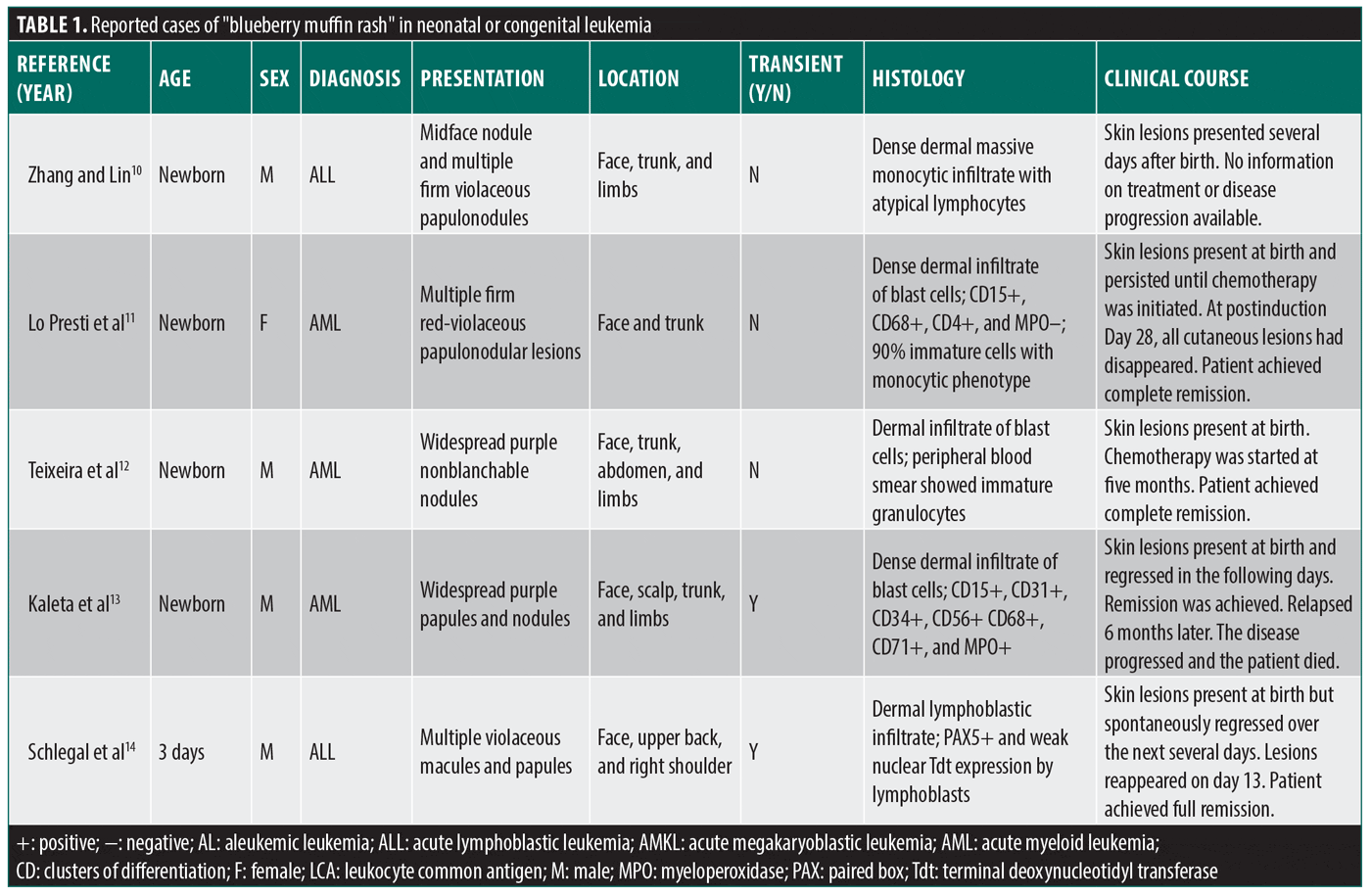
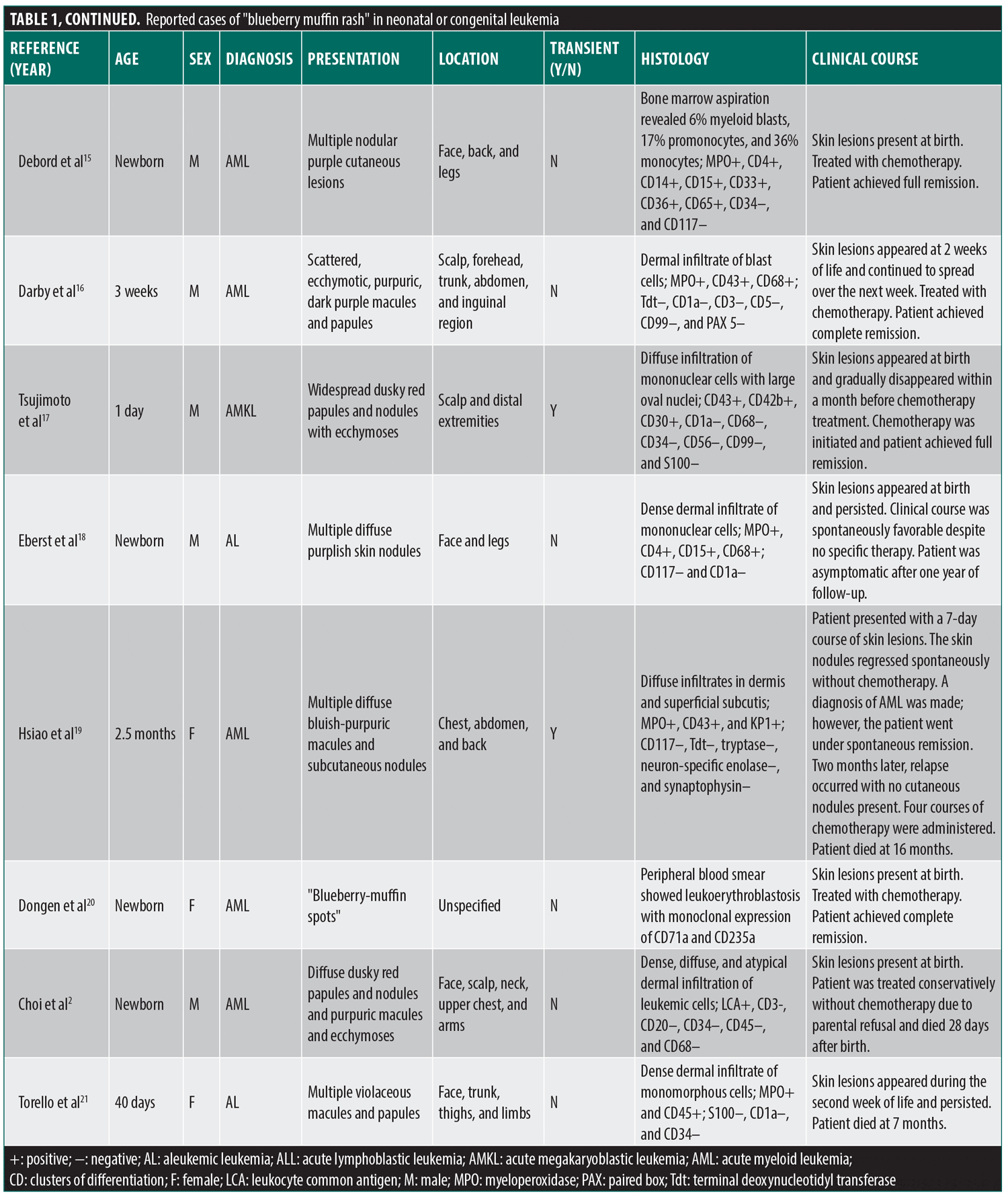
A literature search identified only 13 previously published cases of blueberry muffin rash exclusively linked to congenital leukemia in the past 20 years, a summary of which is included in Table 1. Lesion characteristics were similar across all cases, with widespread violaceous macules, papules, and nodules present at birth being the most common presentation. Additionally, most cases reported similar locations of the rash with facial, truncal, and abdominal involvement being the most prevalent, similar to our patient. On histology, the most common finding was a dense dermal infiltrate of leukemic cells, similar to our patient.
In four of the 13 previously reported cases, the skin lesions appeared at birth and persisted until the patient was treated. In these cases, all patients achieved full remission and are doing well with no residual skin lesions. Four other cases reported a transient cutaneous eruption with varying presentations.13,14,17,19 Interestingly, the eruption in one infant appeared paroxysmal, spontaneously regressing and reappearing before treatment was initiated.17 Of these four transient cases, only two patients achieved full remission and remain in good health; the other two experienced relapse and ultimately succumbed to their disease. Our patient presented with a transient rash similar to these cases and was treated accordingly with a FLAG/Ida + GO chemotherapy regimen. Although our patient achieved full remission, close follow-up with a multidisciplinary team is critical to monitor for any signs of relapse to ensure she remains disease-free.
To our knowledge, this is only the fifth documented report of a transient blueberry muffin rash in a newborn diagnosed with AML. Given its rarity, it is critical for providers to recognize that while a blueberry muffin rash is most commonly associated with congenital infections, it may be an early manifestation of serious hematologic malignancies. The transient nature of the rash, as shown in this case, presents an additional diagnostic challenge. Its spontaneous resolution may lead to a false sense of reassurance or a missed diagnosis, potentially delaying workup and treatment. Increased awareness among providers about the potentially deceptive course of leukemia cutis is crucial to avoid missing or underestimating the significance of a blueberry muffin rash in neonates.
References
- Bayhan T, Çiki K, Tavil B, Gümrük F, Çetin M, Ünal Ş. An infant with congenital leukemia cutis and AML-M5 with MLL gene rearrangement. J Pediatr Hematol Oncol. 2015;37(7):566-567.
- Choi JH, Lee HB, Park CW, Lee CH. A case of congenital leukemia cutis. Ann Dermatol. 2009;21(1):66-70.
- Mehta V, Balachandran C, Lonikar V. Blueberry muffin baby: a pictoral differential diagnosis. Dermatol Online J. 2008;14(2):8.
- Clark EE, Walton M, Chow LML, Boyd JT, Yohannan MD, Arya S. Disseminated juvenline xanthogranuloma with a novel MYH9-FLT3 fusion presenting as a blueberry muffing rash in a neonate. AJP Rep. 2023;13(1):e5-e10.
- Shaffer MP, Walling HW, Stone MS. Langerhans cell histiocytosis presenting as blueberry muffin baby. J Am Acad Dermatol. 2005;53(2 Suppl 1):S143-S146.
- Metayer C, Dahl G, Wiemels J, Miller M. Childhood leukemia: a preventable disease. Pediatrics. 2016;138(Suppl 1):S45-S55.
- Baruchel A, Bourquin JP, Crispino J, et al. Down syndrome and leukemia: from basic mechanisms to clinical advances. Haematologica. 2023;108(10):2570-2581.
- Yang CX, Yang Y, Zhang FL, et al. Congenital leukemia: a case report and review of literature. World J Clin Cases. 2023;11(29):7227-7233.
- Calvo C, Fenneteau O, Leverger G, Petit A, Baruchel A, Méchinaud F. Infant acute myeloid leukemia: a unique clinical and biological entity. Cancers (Basel). 2021;13(4):777.
- Zhang Z, Lin Z. Blueberry muffin rash in neonatal leukemia. Br J Dermatol. 2025;193(4):806.
- Lo Presti C, Szymanski G, Lefebvre C, Jacob MC, Mossuz P, Gil H. Aleukemic congenital leukemia cutis preceding monocytic leukemia with favorable outcome: a case report. EJHaem. 2024;5(1):162-165.
- Teixeira B, Losa A, Meireles A, et al. Blueberry muffin syndrome and hyperleukocytosis in a newborn: a diagnostic challenge. Cureus. 2024;16(1):e52869.
- Kaleta K, Kłosowicz A, Juśko N, Kapiñska-Mrowiecka M. Blueberry muffin baby syndrome. A critical primary sign of systemic disease. Postepy Dermatol Alergol. 2022;39(2):418-420.
- Schlegel S, Hamm H, Reichel A, et al. Neonatal acute lymphoblastic leukemia with t(9;11) translocation presenting as blueberry muffin baby: successful treatment by all-BFM induction therapy, allogeneic stem cell transplantation from an unrelated donor, and PCR-MRD-guided post-transplant follow-up. Am J Case Rep. 2020;21:e927153.
- Debord C, Grain A, Theisen O, Boutault R, Rialland F, Eveillard M. A blueberry muffin rash at birth. Br J Haematol. 2018;182(2):168.
- Darby JB, Valentine G, Hillier K, et al. A 3-week-old with an isolated “blueberry muffin” rash. Pediatrics. 2017;140(1):e20162598.
- Tsujimoto H, Kounami S, Mitani Y, Watanabe T, Takifuji K. Neonatal acute megakaryoblastic leukemia presenting with leukemia cutis and multiple intracranial lesions successfully treated with unrelated cord blood transplantation. Case Rep Hematol. 2015;2015:610581.
- Eberst E, Michel B, Stoebner P, Dandurand M, Meunier L. Lésions cutanées à type de leucémie congénitale “aleucémique” de rémission spontanée. Spontaneous remission of congenital leukemia cutis. Ann Dermatol Venereol. 2011;138(8-9):586-590.
- Hsiao YW, Tseng FW, Shih JL, Kuo TT, Jaing TH, Hui RCY. Blueberry Muffin Baby with acute myeloid leukemia and spontaneous remission. Dermatol Sin. 2011;29(2):47-49.
- van Dongen JCA, Dalinghaus M, Kroon AA, de Vries ACH, van den Heuvel-Eibrink MM. Successful treatment of congenital acute myeloid leukemia (AML-M6) in a premature infant. J Pediatr Hematol Oncol. 2009;31(11):853-854.
- Torrelo A, Madero L, Mediero IG, Baño A, Zambrano A. Aleukemic congenital leukemia cutis. Pediatr Dermatol. 2004;21(4):458-461.