J Clin Aesthet Dermatol. 2026;19(4):18–19.
by Roger I. Ceilley, MD, FAAD, FCMS, and Shandhan Sureshbabu, CDT
Dr. Ceilley is with the Department of Dermatology at the University of Iowa, Iowa City, Iowa. Dr. Ceilley and Mr. Sureshbabu are with Dermatology PC, West Des Moines, Iowa.
FUNDING: No funding was provided for this article.
DISCLOSURES: The authors have no relevant conflicts of interest.
ABSTRACT: A well-organized surgical tray and deliberate instrument selection are essential components of high-quality dermatologic surgery. Proper setup enhances workflow efficiency, minimizes errors, and supports patient safety. Moreover, growing attention to cost and sustainability highlights the importance of reducing instrument waste without compromising the quality of care. This article reviews best practices for tray preparation, discusses historical and modern perspectives on instrument selection, and provides practical recommendations for improving efficiency in dermatologic surgery. Keywords: Dermatologic surgery, surgical tray, surgical instruments, Mohs micrographic surgery, efficiency, waste reduction, safety
Introduction
In dermatologic surgery, the surgical tray represents more than just a collection of tools—it reflects the surgical team’s commitment to efficiency, precision, and patient safety. Proper tray setup reduces intraoperative delays, facilitates instrument handling, and helps prevent errors. The historical evolution of dermatologic surgical instrumentation has also influenced how trays are designed, moving from general surgical tools toward procedure-specific instruments.1
Recent discussions around sustainability and healthcare waste further highlight the need for thoughtful tray design. Excess instruments increase sterilization costs, lead to dulling due to repeated steam sterilization in the autoclave, and contribute to unnecessary environmental burden.2 Standardization and optimization of trays can therefore enhance both clinical outcomes and resource stewardship.
Principles of Surgical Tray Setup
A standardized tray layout provides a reliable foundation for surgical practice. The surgical field should be organized to allow easy access to essential instruments while minimizing unnecessary motion and
potential contamination.3
Preprocedure preparation is critical. The tray should be fully set up before the patient enters the room, with instruments arranged according to the sequence of use. For example, a right-handed surgeon may prefer the scalpel placed on the far right, followed by pickups, scissors, and then the
needle driver.
Clutter should be minimized during each stage of the procedure. For instance, anesthetic vials and syringe caps should be discarded immediately after infiltration to maintain a clean surgical field and reduce the risk
of contamination.
Instrument Selection: Historical and Modern Perspectives
The history of dermatologic surgery reveals a gradual refinement of instruments tailored to skin procedures. In the early twentieth century, dermatologists relied heavily on general surgical instruments, later transitioning toward custom-designed tools for skin cancer excision, flap repair, and Mohs micrographic surgery.1
Scalpel blades are an important part of dermatologic surgical instrumentation. The No. 15 blade is most frequently selected because its narrow, pointed tip allows for precise angling in delicate areas, while the gently curved cutting edge provides controlled, smooth incisions. The No. 10 blade, by comparison, has a broader, more convex shape and is better suited for making longer cuts or working in regions with thicker dermis.1
Adson forceps are commonly used for handling skin and subcutaneous tissue. Their fine, toothed tips provide secure grasping while minimizing crush injury, making them especially useful for wound edge approximation while suturing.1
Metzenbaum scissors are designed for delicate tissue dissection and fine cutting. Their long handles and slender blades allow the surgeon to maneuver in confined spaces with accuracy, helping preserve tissue integrity during undermining or flap mobilization.1
Needle drivers are essential for suturing, with short jaws that provide stability and control when engaging fine suture needles. Properly sized needle holders allow for efficient, secure placement of sutures while reducing surgeon hand fatigue.1
Today, surgeon preference and ergonomics play an important role. Hand size, comfort, and tactile feedback influence instrument selection, particularly for forceps and needle holders. While less expensive instruments may appear cost effective, lower quality can lead to breakage, poor performance, and ultimately higher costs from premature replacement. Additionally, the cost of sharpening, repairing, and sterilizing should be factored into purchase decisions. High-quality instruments, properly maintained, reduce long-term expense and enhance surgical precision.
Efficiency and Waste Reduction
- Instrument waste is a growing concern in dermatology. A quality improvement study found that many instruments included in standard biopsy trays are never used, contributing to unnecessary sterilization costs and material waste.2
- A targeted framework can help address this issue by tailoring tray contents to the most common procedures. Strategies include:
- Developing procedure-specific trays with only essential instruments
- Using modular packs for less common instruments
- Training staff to anticipate procedure requirements based on preoperative planning
- Incorporating ergonomic setups aligned with the surgeon’s dominant hand
- This approach not only reduces waste but also shortens setup and breakdown times, improving clinic efficiency.
Safety Considerations
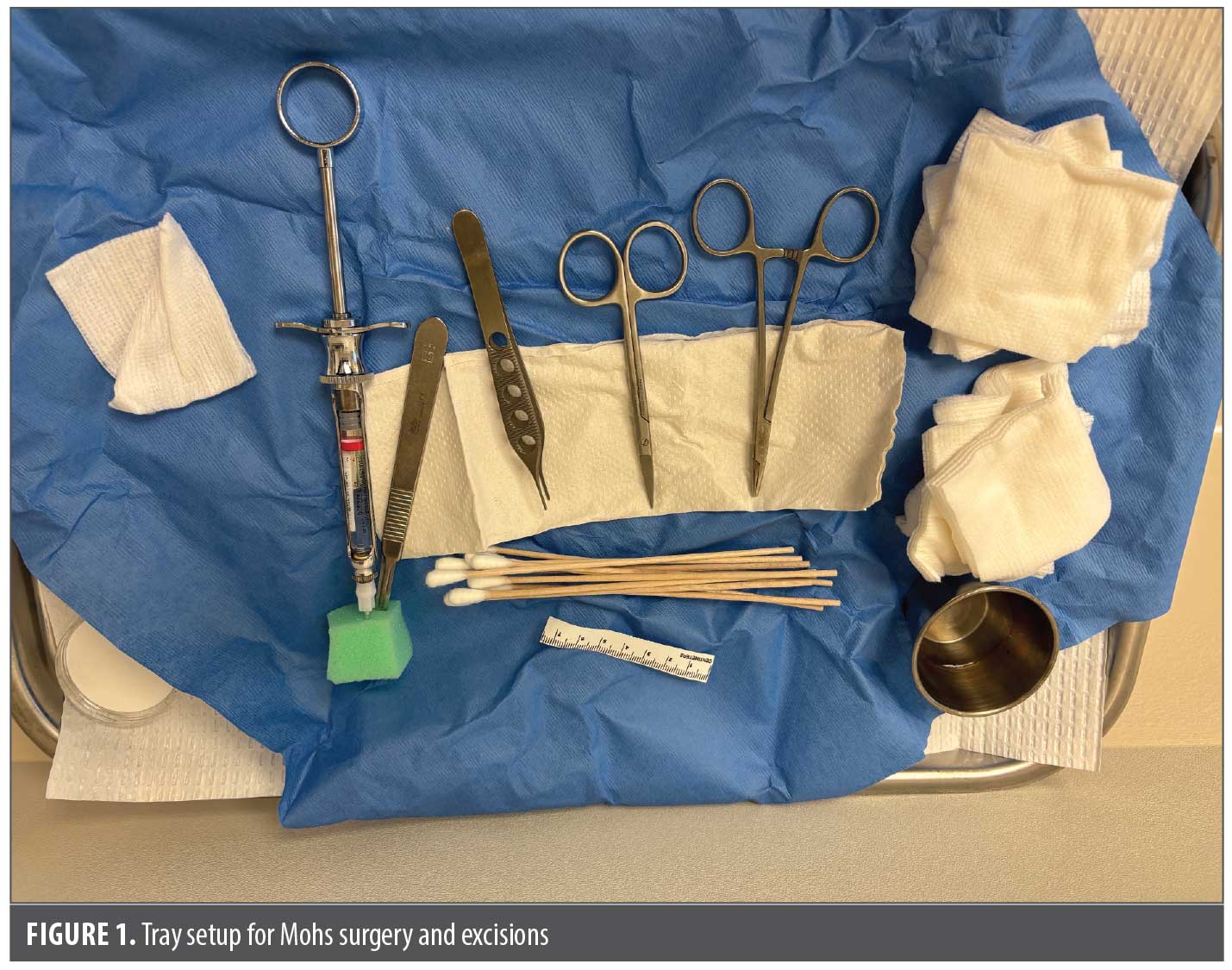
Patient safety is a cornerstone of dermatologic surgery. Standardized tray organization helps minimize errors such as missing or incorrectly placed instruments.3 As shown in Figure 1, practical addition to enhance safety for both the patient and the surgical team is the use of a designated storage apparatus, such as a foam block or sponge, for anesthetic needles and suture needles. This ensures that no sharps are left exposed and the tray is treated with a sterile field in mind.
Sterilization and cleaning protocols must be consistent and standardized to prevent infection. Instruments should be inspected before and after sterilization, and dull or damaged instruments should be removed from circulation for sharpening or replacement.4
Checklists are increasingly used in surgical safety and can be adapted for dermatologic tray setup to ensure all essential instruments are present while avoiding unnecessary items.5 Reducing clutter on the tray also minimizes the risk of cross-contamination.
Special Considerations in Mohs Micrographic Surgery
Mohs surgery presents unique challenges due to its staged nature and the need for rapid tissue handling. Instruments must be readily available for excision, tissue mapping, and reconstruction, often requiring efficient turnover between stages.6
Tray design for Mohs should emphasize flexibility alongside access to core excisional instruments. A separate set of instruments for histologic preparation—including tissue dyes, marking pens, and slides—should also
be available.
Conclusion
Optimizing surgical tray setup and instrument selection is central to delivering efficient, safe, and sustainable dermatologic surgery. Ergonomic placement, thoughtful instrument selection, and attention to workflow enhance efficiency while reducing errors. By combining historical insights, modern innovations, and quality improvement strategies, dermatology practices can reduce waste, improve patient safety, and ensure long-term cost effectiveness. The surgical tray should be viewed not only as a functional necessity but also as a reflection of best practices in dermatologic surgery.
References
- Gandhi SA, Kampp JT. Dermatologic surgical instruments: a history and review. Dermatol Surg. 2017;43(1):11–22.
- Wolstencroft PW, Zacher NC, Scotellaro K, Centkowski S, Kwon BY. Development of a framework for addressing skin biopsy tray waste in dermatology clinics: a quality improvement study. JAMA Dermatol. 2023;159(5):541–544.
- Sobanko JF. The surgical tray. In: Levitt JO, Sobanko JF, eds. Safety in Office-Based Dermatologic Surgery. Springer Cham; 2015:5–11.
- Sobanko JF, Hendi A. Surgical equipment and instrumentation. In: Dermatologic Surgery: Step by Step. Wiley-Blackwell, 14–19.
- Ceilley RI, Sureshbabu S. Enhancing safety in dermatologic surgery: the impact of checklist implementation. J Clin Aesthet Dermatol. 2024;17(12):1617.
- Davis MJ, Kingston D, Nehal KS. (2025). Mohs micrographic surgery operative room setup. In: Nouri K, eds. Mohs Micrographic Surgery. Springer Cham; 2025:761–782.
Optimizing Surgical Tray Setup and Instrument Selection in Dermatologic Surgery
Categories:
J Clin Aesthet Dermatol. 2026;19(4):18–19.
by Roger I. Ceilley, MD, FAAD, FCMS, and Shandhan Sureshbabu, CDT
Dr. Ceilley is with the Department of Dermatology at the University of Iowa, Iowa City, Iowa. Dr. Ceilley and Mr. Sureshbabu are with Dermatology PC, West Des Moines, Iowa.
FUNDING: No funding was provided for this article.
DISCLOSURES: The authors have no relevant conflicts of interest.
ABSTRACT: A well-organized surgical tray and deliberate instrument selection are essential components of high-quality dermatologic surgery. Proper setup enhances workflow efficiency, minimizes errors, and supports patient safety. Moreover, growing attention to cost and sustainability highlights the importance of reducing instrument waste without compromising the quality of care. This article reviews best practices for tray preparation, discusses historical and modern perspectives on instrument selection, and provides practical recommendations for improving efficiency in dermatologic surgery. Keywords: Dermatologic surgery, surgical tray, surgical instruments, Mohs micrographic surgery, efficiency, waste reduction, safety
Introduction
In dermatologic surgery, the surgical tray represents more than just a collection of tools—it reflects the surgical team’s commitment to efficiency, precision, and patient safety. Proper tray setup reduces intraoperative delays, facilitates instrument handling, and helps prevent errors. The historical evolution of dermatologic surgical instrumentation has also influenced how trays are designed, moving from general surgical tools toward procedure-specific instruments.1
Recent discussions around sustainability and healthcare waste further highlight the need for thoughtful tray design. Excess instruments increase sterilization costs, lead to dulling due to repeated steam sterilization in the autoclave, and contribute to unnecessary environmental burden.2 Standardization and optimization of trays can therefore enhance both clinical outcomes and resource stewardship.
Principles of Surgical Tray Setup
A standardized tray layout provides a reliable foundation for surgical practice. The surgical field should be organized to allow easy access to essential instruments while minimizing unnecessary motion and
potential contamination.3
Preprocedure preparation is critical. The tray should be fully set up before the patient enters the room, with instruments arranged according to the sequence of use. For example, a right-handed surgeon may prefer the scalpel placed on the far right, followed by pickups, scissors, and then the
needle driver.
Clutter should be minimized during each stage of the procedure. For instance, anesthetic vials and syringe caps should be discarded immediately after infiltration to maintain a clean surgical field and reduce the risk
of contamination.
Instrument Selection: Historical and Modern Perspectives
The history of dermatologic surgery reveals a gradual refinement of instruments tailored to skin procedures. In the early twentieth century, dermatologists relied heavily on general surgical instruments, later transitioning toward custom-designed tools for skin cancer excision, flap repair, and Mohs micrographic surgery.1
Scalpel blades are an important part of dermatologic surgical instrumentation. The No. 15 blade is most frequently selected because its narrow, pointed tip allows for precise angling in delicate areas, while the gently curved cutting edge provides controlled, smooth incisions. The No. 10 blade, by comparison, has a broader, more convex shape and is better suited for making longer cuts or working in regions with thicker dermis.1
Adson forceps are commonly used for handling skin and subcutaneous tissue. Their fine, toothed tips provide secure grasping while minimizing crush injury, making them especially useful for wound edge approximation while suturing.1
Metzenbaum scissors are designed for delicate tissue dissection and fine cutting. Their long handles and slender blades allow the surgeon to maneuver in confined spaces with accuracy, helping preserve tissue integrity during undermining or flap mobilization.1
Needle drivers are essential for suturing, with short jaws that provide stability and control when engaging fine suture needles. Properly sized needle holders allow for efficient, secure placement of sutures while reducing surgeon hand fatigue.1
Today, surgeon preference and ergonomics play an important role. Hand size, comfort, and tactile feedback influence instrument selection, particularly for forceps and needle holders. While less expensive instruments may appear cost effective, lower quality can lead to breakage, poor performance, and ultimately higher costs from premature replacement. Additionally, the cost of sharpening, repairing, and sterilizing should be factored into purchase decisions. High-quality instruments, properly maintained, reduce long-term expense and enhance surgical precision.
Efficiency and Waste Reduction
Safety Considerations
Patient safety is a cornerstone of dermatologic surgery. Standardized tray organization helps minimize errors such as missing or incorrectly placed instruments.3 As shown in Figure 1, practical addition to enhance safety for both the patient and the surgical team is the use of a designated storage apparatus, such as a foam block or sponge, for anesthetic needles and suture needles. This ensures that no sharps are left exposed and the tray is treated with a sterile field in mind.
Sterilization and cleaning protocols must be consistent and standardized to prevent infection. Instruments should be inspected before and after sterilization, and dull or damaged instruments should be removed from circulation for sharpening or replacement.4
Checklists are increasingly used in surgical safety and can be adapted for dermatologic tray setup to ensure all essential instruments are present while avoiding unnecessary items.5 Reducing clutter on the tray also minimizes the risk of cross-contamination.
Special Considerations in Mohs Micrographic Surgery
Mohs surgery presents unique challenges due to its staged nature and the need for rapid tissue handling. Instruments must be readily available for excision, tissue mapping, and reconstruction, often requiring efficient turnover between stages.6
Tray design for Mohs should emphasize flexibility alongside access to core excisional instruments. A separate set of instruments for histologic preparation—including tissue dyes, marking pens, and slides—should also
be available.
Conclusion
Optimizing surgical tray setup and instrument selection is central to delivering efficient, safe, and sustainable dermatologic surgery. Ergonomic placement, thoughtful instrument selection, and attention to workflow enhance efficiency while reducing errors. By combining historical insights, modern innovations, and quality improvement strategies, dermatology practices can reduce waste, improve patient safety, and ensure long-term cost effectiveness. The surgical tray should be viewed not only as a functional necessity but also as a reflection of best practices in dermatologic surgery.
References
Share:
Recent Articles:
Challenges of Treating Recurrent Merkel Cell Carcinoma in the Rural US: A Case Report
Case Series: Successful Management of Refractory Plaque Psoriasis With Combined Laser Therapy and Topical Roflumilast in 2 Patients
Quality of Life in Young Adults With Acne
From Clinic to Conference: A Practical Guide for Dermatology PAs and NPs Preparing a Scientific Poster
Letter to the Editor: April 2026
Categories:
Recent Articles:
Plant Exosome Injection: A New Boost for Postlaser Vascular Repair
Hispanic and Latino Ethnicity and Acculturation: Influences on Skin Cancer Prevention Attitudes and Behaviors
Optimizing Surgical Tray Setup and Instrument Selection in Dermatologic Surgery
Severe Nail Psoriasis and Early Psoriatic Arthritis: Illustrative Cases Confirming That Severity of Disease Is Not Solely Dependent on the Extent of Body Surface Area
The Treatment of Perioral (Periorificial) Dermatitis With Topical Roflumilast 0.3% Cream: An Illustrative Case Study With Rapid Onset and Prolonged Remission