
by Blair Ferguson, DNP, APRN
Mr. Ferguson is with Natura Dermatology and Cosmetics in Fort Lauderdale, Florida.
Funding: No funding was provided for this article.
Disclosures: The author has no conflicts of interest relevant to the content of this article.
J Clin Aesthet Dermatol. 2024;17(5–6 Suppl 1):S16–S18.
Abstract: Mantle cell lymphoma (MCL) can, in a few reported cases, create an exaggerated mosquito bite response, leading to numerous bullae and significant edema. The phenomenon is further complicated by the observance of a concurrent Epstein-Barr virus (EBV) reactivation. The current literature provides general information on treatment that most practitioners would consider when attempting to treat an arthropod hypersensitivity reaction, such as topical or systemic corticosteroids. However, no information has been published to date that details a preventive and steroid-sparing approach to treating this phenomenon, without simultaneously treating the MCL. MCL can be indolent in nature and does not always require prompt treatment. The purpose of this case report is to discuss the successful treatment of a rare disorder with a steroid-sparing regimen. The steroid-sparing regimen used consisted of oral doxycycline 100mg twice daily, cetirizine 20mg once daily, and valacyclovir 1g daily, which resulted in sustained reduction in bullous eruptions.
Keywords: Mantle cell lymphoma, mosquito bite, Epstein-Barr virus
Introduction
Mantle cell lymphoma (MCL) is a rare form of cancer that affects approximately 0.1 to 1.27 individuals per 100,000, as of 2019.1 Dermatology clinicians have experience managing associated symptoms from various cancers, as well as managing side effects of treatment involving the skin. One of the most common symptoms a dermatology clinician may see is carcinoid syndrome resulting in a rash. In rare cases, MCL may produce exaggerated mosquito bite reactions, resulting in severe edema. Other factors, such as Epstein-Barr virus (EBV) reactivation and elevated immunoglobulin E (IgE) levels may also play a role. This article discusses the severity of mosquito bite reactions in a patient with MCL, laboratory findings, and a steroid-sparing treatment regimen.
Case Report
A 73-year-old Caucasian female patient was referred by her primary care physician for a second opinion dermatology consultation after experiencing a blistering rash on her bilateral ankles and lower extremities (Figures 1–3). The rash waxed and waned over the course of a few months but was progressively becoming more severe. There was not a significant amount of pruritus or pain, but the bullae were causing significant leg and ankle swelling, limiting mobility. The primary care physician suspected bullous pemphigoid. The patient reported that she was generally healthy; however, she had seen an oncologist and was suspected to have MCL, but the disease appeared to be indolent, and a definitive diagnosis had not been given. The patient was asked about a history of cold sores, which she confirmed. Topical therapy from a previous dermatologist, augmented betamethasone cream 0.05%, was ineffective at treating her lesions.
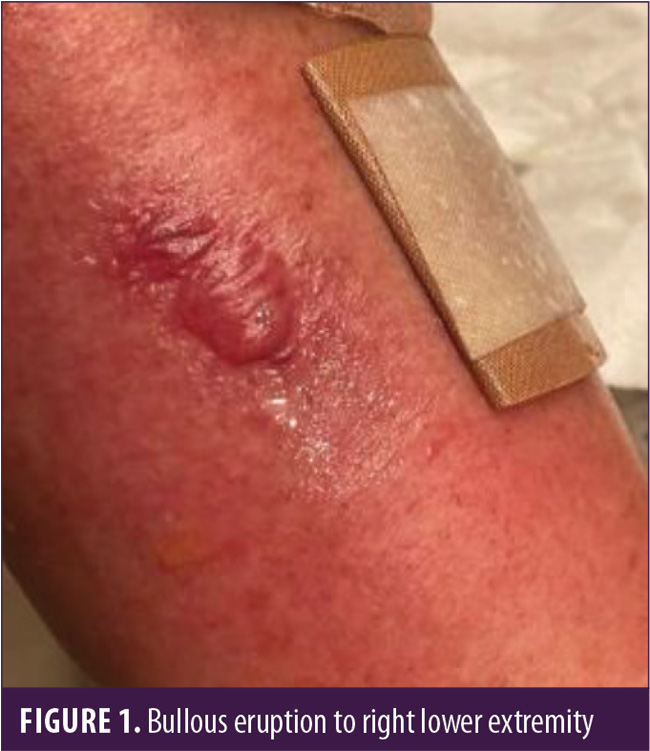
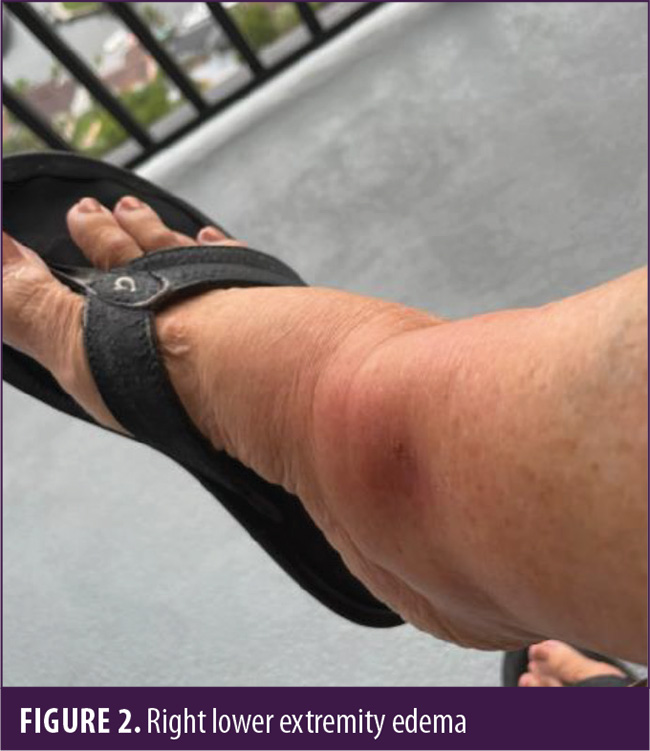
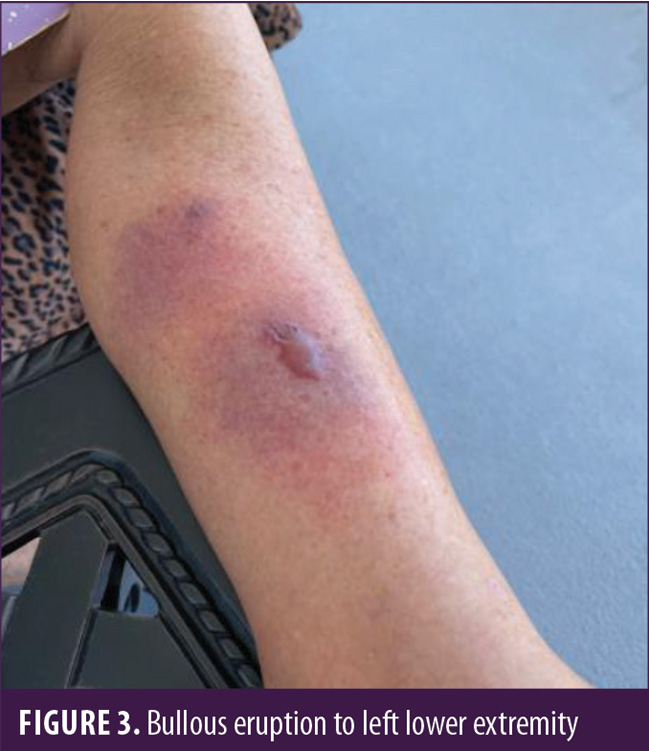
The patient was present with her spouse, and they appeared to be excellent historians. They were certain that the bullae were the result of mosquito bites. The patient stated she was about to take a vacation out of the state. Due to her upcoming trip, a punch biopsy was postponed, and the patient was treated with combination therapy to cover the three top diagnoses in the differential list (bullous pemphigoid, bullous erythema multiform related to the herpes simplex virus, and bullous arthropod hypersensitivity reaction). The patient was given 40mg of intramuscular triamcinolone, oral valacyclovir 1g three times daily, and oral doxycycline 100mg twice daily and was instructed to take 20mg cetirizine once daily. Topical betamethasone was replaced with topical clobetasol cream 0.05%.
The patient returned from her trip and followed up with the office. She had no bullous eruptions and was doing well without reporting side effects of the medications. Her valacyclovir was decreased to 1g daily, and she was instructed to follow up again in another two weeks. The patient returned and was still free of symptoms, and her doxycycline was decreased to 50mg twice daily. Six days later, the patient returned with bullae present on her bilateral lower extremities and ankles. The patient and spouse both reported they saw a mosquito bite her in the area of the current bullae. Two punch biopsies were performed, consisting of a lesional hematoxylin and eosin (H&E) stain and a perilesional direct immunofluorescence stain (DIF). Pathology returned with a diagnosis of exaggerated arthropod bullous eruption in the background of MCL; DIF was negative.
A literature review was done, and as a result, laboratory orders then included epidermal antibodies, which were negative, and serology of EBV, which showed EBV early antigen D antibody (IgG) titer of 141U/mL (normal reference range <9U/mL); EBV viral capsid antigen (VCA) of 590U/mL (positive if >21.99U/mL); and EBV EBV nuclear antigen (EBNA) titer of 111U/mL, (positive if >21.99U/mL). The patient saw the oncology department for a follow-up and reported the MCL was confirmed but did not agree that her dermatology issues were related to MCL; she agreed with her primary care physician that the diagnosis was bullous pemphigoid. The oncologist scheduled a dermatology appointment, new opinion, for an additional punch biopsy to be read by their own pathologist. The report returned with the same diagnosis, an exaggerated mosquito bite reaction. The patient was then referred to infectious disease and was told she had a previous infection with EBV, but no current infection. In addition to EBV titers, IgE levels were ordered by infectious disease and were found to be elevated. The patient then started to notice bullous eruptions where no mosquito bite was evident.
Discussion
Very little information exists in the literature regarding an exaggerated mosquito bite reaction and MCL, but a few case reports have been published.2 Some case reports have gone further to mention the association with apparent EBV, in conjunction with MCL and exaggerated mosquito bite reactions.3 No literature was found, however, that addressed resolving or treating the issue. Literature discusses the use of topical steroids and antihistamines, as well as intralesional steroids, but does not propose a reasonable long-term and preventative plan. Previous articles mentioned treating the MCL but offered no guidance on the treatment of an arthropod eruption as a preventative measure that, due to its extreme nature, was debilitating to the patient.1 Not all cases of MCL require prompt treatment.4 If the patient and the oncologist were not ready to treat the MCL, as it was not progressing and appeared to be indolent in nature, no further guidance in the previous literature was offered.
In this case, the patient resided in a tropical climate, and avoidance of mosquito bites was not practical. The presence of elevated IgE suggests the patient might hyper-respond to a variety of stimuli, not limited to mosquito or arthropod assaults.5 The first attempt at combination therapy and dosage worked well for the patient but included systemic corticosteroids, and the patient was concerned about long-term side effects, such as weight gain, changes in blood sugar, and bone loss. However, the patient also did well with a steroid sparing regimen. Her symptoms were significantly milder and did not result in a bullous eruption limiting mobility. Over the next few months, medication changes were made, with the intent of lowering a certain medication and observing for changes. Every time one of the medications was altered or lowered, which included doxycycline 100mg twice daily, cetirizine 20mg once daily, and oral valacyclovir 1g daily, the patient experienced a bullous eruption or flare, which suggests this phenomenon might be multifaceted and stem from a complex relationship between IgE elevation, reactivation of EBV, and MCL.
The complexity of this case revolves around the rarity of the condition and general lack of information and guidance for treatment. The presence of a high Epstein-Barr titer further complicates the case because it is not known what role EBV plays in the bullous eruption, or if EBV is simply an innocent bystander. It was the opinion of infectious disease that the patient had a previous exposure to EBV and did not have an active infection. Although IgG antibody titers can represent a previous exposure, when they are unusually high and symptoms are present, it seems reasonable to assume that there has been a viral reactivation, and not simply a previous exposure.6 The IgG titers correlate better in cerebral spinal fluid than serum, but IgG titer levels are routinely used to monitor disease activity.6 The patient’s IgG EBV titers rose once patient stopped or altered the treatment regimen.
This case report illustrates the first proposed steroid-sparing mechanism for treating this unusual and rare exaggerated mosquito bite reaction in the presence of EBV. The patient has remained stable with a steroid-sparing regimen over the last few months, and her current regimen includes valacyclovir 1g daily, doxycycline 100mg twice daily, and cetirizine 20mg daily, with topical clobetasol cream 0.05% twice daily at the first sign of a mosquito bite. The proposed mechanism of action for valacyclovir is the reduction in viral shedding from EBV.7 Of note, spironolactone has demonstrated even more efficacy in reducing EBV viral replication,8 but this patient was unable to take it due to a previous adverse reaction to it. Doxycycline possesses anti-inflammatory effects by way of neutrophil inhibition, as well as decreasing inflammatory cytokines,9 and has shown anti-viral activity in vitro.10 Cetirizine is known to decrease histamine binding to receptor sites, which can limit the allergic response, but has also been shown to decrease IgE levels.11
Conclusion
In some cases, MCL has been linked to a reactivation of EBV, along with elevated IgE levels and a hypersensitivity to arthropod assaults, such as mosquitos. It is unclear what role EBV reaction has in this phenomenon, if it is responsible for the elevation in IgE or if it is simply an incidental finding that plays no role in the inflammatory process. However, decreases in oral doxycycline and oral valacyclovir resulted in more extreme bullous eruptions, suggesting the antiviral properties of the medications might play a significant role in the mosquito hypersensitivity phenomenon. A steroid-sparing regimen, which included oral valacyclovir 1g daily, doxycycline 100mg twice daily, and cetirizine 20mg once daily, was found to be effective at minimizing the severity of the bullous eruptions. Although further research is needed to understand the phenomenon, the steroid-sparing regimen might be an appropriate option for patients who are unable or unwilling to include systemic corticosteroids as part of their treatment regimen.
References
- Monga N, Garside J, Quigley J, et al. Systematic literature review of the global burden of illness of mantle cell lymphoma. Curr Med Res Opin. 2020;36(5):843–852.
- Darji K, Bahram-ahi E, Dhandha M, Guo M. Mantle cell lymphoma presenting with exaggerated skin reaction to insect bites. BMJ Case Reports. 2019;12(3):e227590.
- Shigekiyo T, Ohmori H, Chohraku M, et al. Unusual skin reactions after mosquito bites and Epstein-Barr virus reactivation in a patient with mantle cell lymphoma. Intern Med. 2004;43(10):986–989.
- Furtado M, Rule S. Indolent mantle cell lymphoma. Haematologica. 2011;96(8):1086–1088.
- Yang T-LB, Kim BS. Clinical review: pruritus in allergy and immunology. J Allergy Clin Immunol. 2019;144(2):353–360.
- Volkov MS, Coppola M, Huizinga R, et al. Comprehensive overview of autoantibody isotype and subclass distribution. J Allergy Clin Immunol. 2022;150(5):999–1010.
- Mehta SK, Diak DM, Rooney BV, et al. Antiviral treatment with valacyclovir reduces virus shedding in saliva of Antarctic expeditioners. Front Virology. 2023;3.
- Verma D, Thompson J, Swaminathan S. Spironolactone blocks Epstein–Barr virus production by inhibiting EBV SM protein function. Proc Natl Acad Sci U S A. 2016;113(13):3609–3614.
- Henehan M, Montuno M, De Benedetto A. Doxycycline as an anti-inflammatory agent: updates in dermatology. J Eur Acad Dermatol Venereol. 2017;31(11):1800–1808.
- Alexpandi R, Gendrot M, Abirami G, et al. Repurposing of doxycycline to hinder the viral replication of SARS-CoV-2: from in silico to in vitro validation. Front Microbiol. 2022;13: 757418.
- Zhou P, Jia Q, Wang Z, et al. Cetirizine for the treatment of allergic diseases in children: a systematic review and meta-analysis. Front Pediatr. 2022;10:940213.
