J Clin Aesthet Dermatol. 2026;19(4):28–29.
by Madeline Lillich, BS; Mikel Muse, DO; Izabelle Bermudez, BS; Sabiha Uddin, DO; and James Appel, MD
Ms. Lillich is with the University of North Carolina at Chapel Hill School of Medicine, Chapel Hill, North Carolina. Dr. Muse is with Campbell University School of Osteopathic Medicine, Buies Creek, North Carolina, and Atlantic Dermatology, Wilmington, North Carolina. Ms. Bermudez and Dr. Uddin are with the Campbell University School of Osteopathic Medicine, Buies Creek, North Carolina. Dr. Appel is with Wilmington Health Dermatology, Wilmington, North Carolina.
FUNDING: No funding was provided for this article.
DISCLOSURES: The authors have no relevant conflicts of interest.
ABSTRACT: Extrafacial rosacea involving the scalp is an uncommon manifestation of acne rosacea, for which evidence-based treatment guidance is limited. With this retrospective study, we aimed to evaluate the effectiveness and tolerability of low-dose isotretinoin in patients with rosacea involving both the face and scalp. We conducted an observational chart review of adult male patients treated with isotretinoin for this condition at our multisite private practice between 2012 and 2022; 21 patients met inclusion criteria. Treatment courses were short with a low dose (mean cumulative dose: 81.0 mg/kg; mean daily dose: 0.67 mg/kg/day; mean duration: 3.95 months). Complete clinical clearance of facial and scalp disease was achieved in 85.7% of patients, and treatment was well tolerated, with 95.2% of patients completing a full therapeutic course. This study suggests that low-dose, short-duration isotretinoin is a viable and effective systemic treatment option for extrafacial rosacea and may fill an important gap in the management of refractory scalp disease. Keywords: Rosacea, extrafacial rosacea, isotretinoin, scalp, chronic dermatoses
Introduction
Acne rosacea is among the most common chronic dermatologic conditions affecting adults, with presentation characterized by erythema, papules, pustules, confluent nodules, and telangiectasias localized to the forehead, cheeks, and nose.1 Extrafacial rosacea is a rare and atypical presentation occurring on the scalp, neck, chest, and upper back that most commonly arises as a complication of severe facial rosacea, particularly in older men.2 As a clinical entity, rosacea involving the scalp has not been extensively characterized in the literature3-5 and is likely underreported, as diagnosis can be challenging due to atypical patterning, similarity to other common scalp dermatoses, and the hidden location of cutaneous involvement beneath hair.3 While multiple causes for the development of facial rosacea have been proposed, including vascular, chemical, environmental, and microbial etiologies such as Demodex folliculorum and Helicobacter pylori, the exact mechanism remains unclear and there is no known cause for extrafacial rosacea.5
Current rosacea treatment guidelines recommend oral antibiotics combined with topical anti-inflammatory agents as first-line therapy, which have anecdotally proven less effective against stubborn extrafacial cases of rosacea.6 Although isotretinoin has been widely used as an off-label treatment for severe and refractory cases of facial rosacea, there are limited reports in the literature of its use for extrafacial disease.1–3 Existing reports focus on a single or small number of cases treated with isotretinoin or explore treatment with alternative therapies such as tetracyclines, systemic corticosteroids, and azithromycin.2–4,7,8 Our study seeks to evaluate the effectiveness and tolerability of low-dose isotretinoin for the treatment of rosacea involving both the face and scalp.
Methods
We conducted a retrospective observational chart review at our multisite private practice to identify patients diagnosed with rosacea of the face and scalp between 2012 and 2022. Inclusion criteria were: (1) men aged 35 to 78 years; (2) clinical diagnosis of rosacea involving the face and scalp; and (3) treatment with isotretinoin. Exclusion criteria were: (1) concomitant use of prescription oral or topical rosacea treatment (eg, tetracycline antibiotics, topical metronidazole); (2) active isotretinoin treatment at time of chart review; and (3) lost to follow up prior to treatment completion. Demographic and clinical data were abstracted from the electronic medical record for further analysis using descriptive statistical methods.
Results
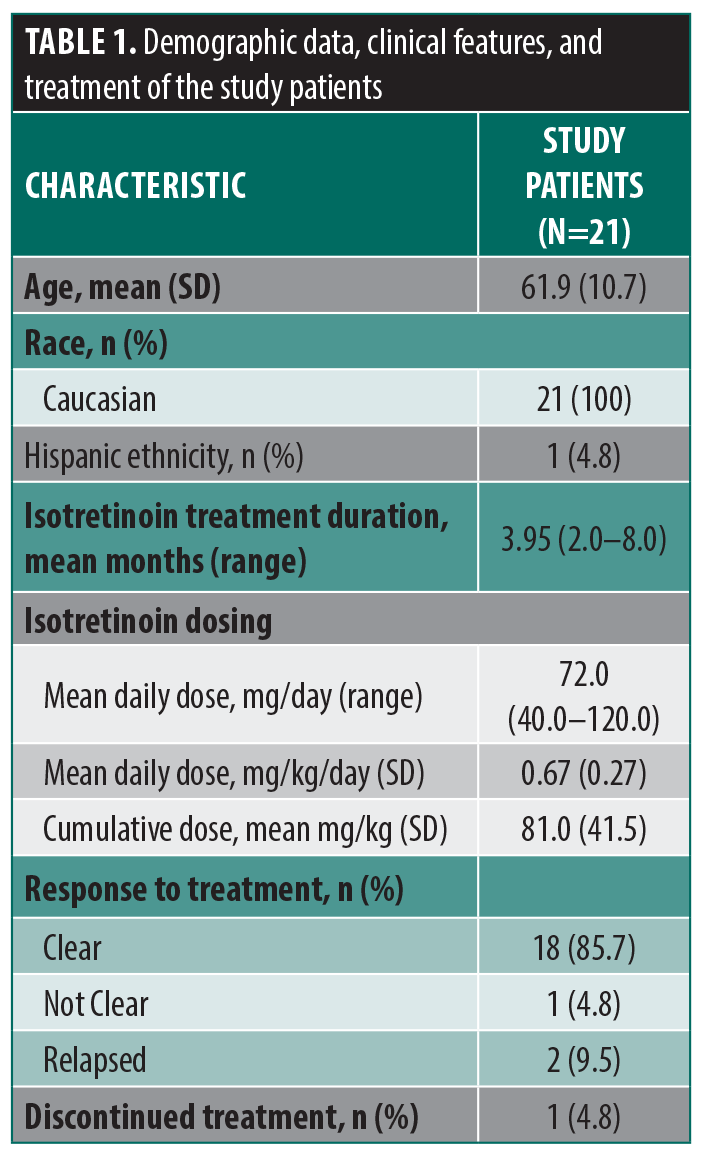
A total of 21 patients were identified as meeting the inclusion criteria. Demographic characteristics of the study population are reported in Table 1. Patients were predominantly older male adults (mean age: 61.9 years; SD: 10.7), and all identified as White. While isotretinoin treatment regimens varied in dose and length, courses tended to be cumulatively low dose (mean: 81.0 mg/kg; SD: 41.5), administered at low daily doses (mean: 0.67 mg/kg/day; SD: 0.27), and brief (mean: 3.95 months; SD: 1.3; range: 2.0–8.0; Table 1). Overall, a strong positive response to treatment was observed, with 85.7% of patients (n=18) experiencing complete clearance of their rosacea on the face and scalp. There was no predefined cutoff for treatment cessation, with clinicians generally continuing isotretinoin for an additional 2 to 3 months following achievement of complete clinical clearance. Patients who experienced relapse (n=2; 9.5%) did so within 24 to 36 months after therapy cessation; no patients experienced relapse during treatment. Treatment was also well tolerated, with nearly all patients (95.2%; n=20) completing the prescribed course of isotretinoin for its full duration. Only 1 patient discontinued treatment prematurely after experiencing dry eye as an adverse effect.
Discussion
Our results indicate that short-duration, low-dose isotretinoin is a practicable treatment option for extrafacial rosacea given its high observed efficacy and favorable tolerability profile. Notably, the majority of patients achieved complete clearance within a relatively brief treatment window and at cumulative doses substantially lower than those typically used for acne vulgaris. This suggests that therapeutic benefit may be achieved without prolonged exposure or significant dose escalation, potentially minimizing treatment-related adverse effects and improving patient adherence.
Diagnostic challenges, the predilection for severe disease in the presence of extrafacial involvement, and a lack of evidence-based treatment recommendations complicate management of this condition.2,4,5 Delayed or missed diagnosis in the face of such challenges may contribute to prolonged disease activity, impairment of patient quality of life, repeated antibiotic courses, and unnecessary exposure to systemic corticosteroids. Incorporating extrafacial rosacea into the differential diagnosis of refractory inflammatory scalp disorders may reduce diagnostic latency and improve care efficiency.
Existing reports of this condition have included small patient cohorts, isolated case reports treated with isotretinoin, or investigations of alternative treatment modalities.2,4,7 There is growing attention in the literature, however, on improving diagnostic accuracy through the characterization of disease-specific trichoscopic features.8-10 Integration of these trichoscopic criteria with our observed therapeutic response offers a practical diagnostic-treatment framework for clinicians. Earlier recognition of characteristic vascular patterns should prompt consideration of a diagnosis of extrafacial rosacea in patients with refractory scalp disease and facilitate more timely initiation of appropriate systemic therapy, with isotretinoin as a feasible option.
Of note, treatment in this cohort was achieved using relatively low cumulative doses over short durations, which likely contributed to the favorable tolerability profile observed. This is particularly relevant in the older patient demographic most commonly diagnosed with this condition, who may have greater baseline comorbidities and medication burdens. Our findings suggest that prolonged high-dose regimens may not be necessary to achieve clinical remission in extrafacial disease.
The modest sample size of this study and its retrospective nature, as well as a homogeneous study population, are limitations. Furthermore, unlike acne vulgaris, for which isotretinoin dose targets and therapeutic cessation conventions are well established, medication discontinuation in this cohort occurred based on individual clinician judgment after clinical clearance. Further prospective studies with designated follow-up periods are needed to further characterize efficacy, long-term relapse rates, and optimal isotretinoin treatment regimens for this condition.
References
- Sobottka A, Lehmann P. Rosacea 2009: new advances in pathophysiology, clinical staging and therapeutic strategies. Article in German. Hautarzt. 2009;60(12):999–1009.
- Bostanci O, Borelli C, Schaller M. Treatment of extrafacial rosacea with low-dose isotretinoin. Acta Derm Venereol. 2010;90(4):409–410.
- Fortuna MC, Garelli V, Pranteda G, et al. A case of scalp rosacea treated with low dose doxycycline and probiotic therapy and literature review on therapeutic options. Dermatol Ther. 2016;29(4):249–251.
- Pereira TM, Vieira AP, Basto AS. Rosacea with extensive extrafacial lesions. Int J Dermatol.2008;47(1):52–55.
- Crawford GH, Pelle MT, James WD. Rosacea: I. Etiology, pathogenesis, and subtype classification. J Am Acad Dermatol. 2004;51(3):327–341.
- Desai S, Friedman A. Isotretinoin for rosacea: a systematic review. JAAD Int. 2024;16(1):112–118.
- Smith LA, Meehan SA, Cohen DE. Rosacea fulminans with extrafacial lesions in an elderly man: successful treatment with subantimicrobial-dose doxycycline. J Drugs Dermatol. 2014;13(6):763–765.
- Asz-Sigall D, Segarra-Ponce A, Olvera-Lerma S, Cano-Aguilar LE, Coronoa-Rodarte E. Red scalp disease: an underdiagnosed entity. Skin Appendage Disord. 2025;11(3):291–295.
- Lin D, Martins G, Sanz J, Corral L, Miteva M. A pilot retrospective study on trichoscopy of 21 cases of rosacea of the scalp. J Am Acad Dermatol. 2023;88(4):898–900.
- Vázquez-Herrera NE, Zamora-Benze DM, Garza-Chapa JI, Rodríguez-Baca AB, Tosti A. Scalp rosacea: rethinking peripilar scaling. Skin Appendage Disord. 2021;7(5):382–386.

Optimizing Surgical Tray Setup and Instrument Selection in Dermatologic Surgery