
Impact of a List of Common Dermatology Diagnoses on Medical Student Experience During Dermatology Rotation
J Clin Aesthet Dermatol. 2022;15(10):18–20.
Dear Editor:
Not enough time in medical school is dedicated to studying dermatology.1,2 Dermatology rotations are expected to fill gaps in medical knowledge.3 There is a lack of knowledge regarding demographics of dermatology rotators and ways to improve elective experience.
Our study had two aims. The first was to compare the number of students who rotated to the number who had the potential to rotate in order to determine if there was a notable difference. The second was to investigate whether providing a list of 25 common dermatologic diagnoses to the rotators would lead to more diagnoses seen and improved knowledge retention. After IRB approval, we performed a prospective study and enrolled medical student dermatology rotators at two universities over two years.
Informed consent was obtained and students were randomized into intervention and control groups. Students received pre- and post-rotation surveys and knowledge tests, completed on REDCap. A list of 25 diagnoses was derived from the most common conditions encountered by physicians and personal experience (Supplemental Table 1).4 The list contains six diagnoses not found in the AAD Basic Dermatology curriculum.
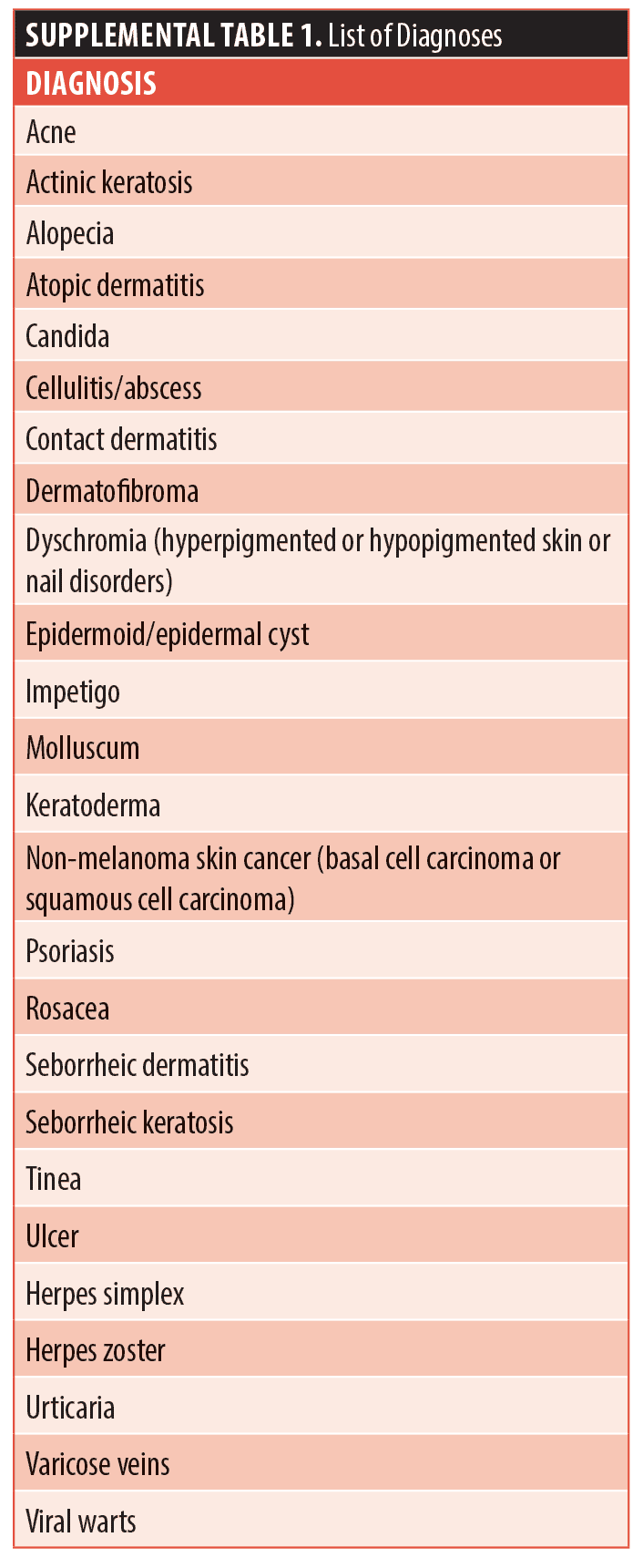
The intervention group only was handed the diagnosis list prior to the rotation. Both groups were instructed to tally the number of times any dermatology diagnosis was seen. Paired Student’s T-tests and Wilcoxon Matched-Pairs Signed Rank Tests were performed for normally and non-normally distributed data, respectively. Analyses were completed using SPSS (Armonk, NY). The significance was p<0.05.
Sixty-five students (100% of eligible rotators) were enrolled, and demographics between the two groups were similar (Table 1). Outcomes did not show statistical differences for change in interest, confidence, rotation satisfaction, and dermatology knowledge as measured by a change in the pre- and post-rotation test scores (Table 2). Higher non-significant changes in pre- and post-rotation scores and change in confidence were observed in intervention vs control group.


A significant higher number of diagnoses were seen in intervention (75.7±5.9) versus the control (50.6±6.8) group, p=0.005. There was a trend towards significance in applicability of dermatology in future careers in intervention versus the control group, p=0.130.
Twenty percent of the medical student classes could rotate per year (calculated by dividing number of rotator spots available by total class sizes), and of those, 33 to 47 percent rotated (Table 3). Home (same medical school) rotators constituted less than or greater to 50 percent of the total dermatology rotators. Fifty-seven to 67 percent of the home rotators matched dermatology.

Limitations in our data were not compared to the medical student classes as a whole. Our intervention list did not include all common diagnoses, inability to determine why there were so few rotators in dermatology, and only studying two centers.
This cohort characterizes the demographics of dermatology rotators. We demonstrate that the number of potential dermatology rotators is inadequate (Table 2). The potential slots remain underfilled, but the reason for this is unclear. We suggest that programs work to increase the number of potential spots and reach out to and promote dermatology rotations among home students.
Separately, we found that providing a list of 25 dermatology diagnoses was associated with more diagnoses seen or logged by the students. Though there was no statistical change in test scores, possibly due to too few rotators enrolled, seeking out and generating the diagnoses encourages active learning. The more diagnoses seen, the more a rotator learns and revisits; spaced education is key to learning.5 We suggest that dermatology programs distribute this list to medical student rotators.
With regard,
by Abraham Moris Korman, MD; Alecia Blaszczak, MD, PhD; Veronica Russo, MD; and Jessica Kaffenberger, MD
Keywords. Dermatology rotations, education roadmap, medical education
Affiliations. All authors are with Division of Dermatology, Department of Internal Medicine at The Ohio State University in Columbus, Ohio
Funding. No funding was provided for this article.
Disclosures. The authors report no conflicts of interest relevant to the content of this article.
References
- McCleskey PE, Gilson RT, DeVillez RL. Medical Student Core Curriculum in Dermatology Survey. Journal of the American Academy of Dermatology. 61, 30–35 e34.
- Ulman CA, Binder SB, Borges NJ. Assessment of medical students’ proficiency in dermatology: Are medical students adequately prepared to diagnose and treat common dermatologic conditions in the United States? J Educ Eval Health Prof. 2015 May 17;12:18.
- Cayce R, Bergstresser P, Hesterman K, et al. Dermatology curriculum for internal medicine residents: a randomized trial. J Grad Med Educ. 2014 Jun;6(2):296-300.
- Wilmer EN, Gustafson CJ, Ahn CS, et al. Most common dermatologic conditions encountered by dermatologists and nondermatologists. Cutis. 2014;94(6):285–292.
- Kerfoot BP, DeWolf WC, Masser BA, et al. Spaced education improves the retention of clinical knowledge by medical students: a randomised controlled trial. Med Educ. 2007;41(1):23–31.
