 J Clin Aesthet Dermatol. 2022;15(9 Suppl 1):S10–11
J Clin Aesthet Dermatol. 2022;15(9 Suppl 1):S10–11
by Archana M. Sangha, MMS, PA-C
Ms. Sangha is a medical science liaison for Incyte in Wilmington, Delaware. Prior to that, she spent over a decade as a dermatology PA specializing in general, surgical, and cosmetic dermatology. She is a fellow of the American Academy of Physician Assistants in Alexandria, Virginia. She is also Immediate Past President of the Society of Dermatology Physician Assistants.
FUNDING: No funding was provided for this article.
DISCLOSURES: Ms. Sangha is an employee of Incyte in Wilmington, Delaware.
Vitiligo has been a skin condition near and dear to my heart since I began practicing dermatology. The disease caught my attention because I saw the devastating and far-reaching repercussions it had on a patient’s self-esteem. I’ve seen, in my own clinical practice, how having vitiligo impacted the smallest to largest of life decisions. Patients shared with me how they chose their clothes painstakingly so they could conceal their patches of vitiligo. Other patients disclosed that vitiligo was the reason they didn’t take the promotion for fear of having to be “the face of their company” or chose not to have children for fear of passing along the disease. For so many patients, vitiligo seemed to be their rate-limiting step. It hindered their ability to reach their fullest potential because of how others perceived their disease and therefore them.
As a clinician, vitiligo has been a frustrating disease to treat. Until recently, we had no United States Food and Drug Administration (FDA)-approved drugs for repigmentation. But now, the future looks bright for patients with vitiligo as decades of research has led to a better understanding of its pathophysiology and more therapeutics are under development.
In this article, I debunk some of the widely held myths about vitiligo within the dermatology community.
Myth 1: Vitiligo prevalence is greater among skin of color (SOC) populations.
While the appearance of vitiligo in SOC populations is more apparent due to the sharp contrast against darker skin phototypes, vitiligo does not have a predilection for SOC populations.1
Myth 2: Vitiligo mainly impacts adults.
Nearly 50 percent of patients with vitiligo develop it before the age of 20.2
Myth 3: Depression and anxiety prevalence is the same in patients with vitiligo as the general population.
Patients with vitiligo are disproportionately affected by anxiety and depression compared to those without vitiligo. In a study looking at 100 vitiligo patients and 100 healthy controls, depression and anxiety disorders affected patients with vitiligo disproportionately (62% vs 25%).3 A recent meta-analysis found the prevalence of anxiety to be 35.8 percent among patients with vitiligo. In a subgroup analysis, it was found there were slight differences in prevalence based on the patient’s continent of residence. The highest prevalence rates of anxiety were seen in Africa.4 Another study found that out of 308 patients with vitiligo, nearly 55 percent suffered from depression. Single women in their first few years of disease were found to have greater prevalence of depression.5
Myth 4: The psychosocial disease burden of vitiligo is only seen in SOC populations.
The psychosocial impact of vitiligo affects all patients, regardless of their skin phototype. A recent article by Ezzedine et al6 showed that while the psychosocial burden of disease is similar across all patients, there are a few differences in what most concerned patients based on their skin color. In particular, fair-skinned patients were more concerned about skin cancer development, whereas darker-skinned patients were more concerned about the appearance.6
Myth 5: The hair color in a depigmented patch doesn’t mean anything.
The presence of leukotrichia (white hairs) within a patch of vitiligo is often a poor prognostic sign for repigmentation. One study looked at UVB response rates among vitiligo patients who had leukotrichia within their vitiligo patches and those who did not. Those without leukotrichia had a much higher response rate.7 This can be attributed to the reservoir of melanocyte stem cells located within the hair bulge of the hair follicle. If leukotrichia is present, there is a decreased likelihood that repigmentation will occur.
Myth 6: All areas of the body repigment at the same rate.
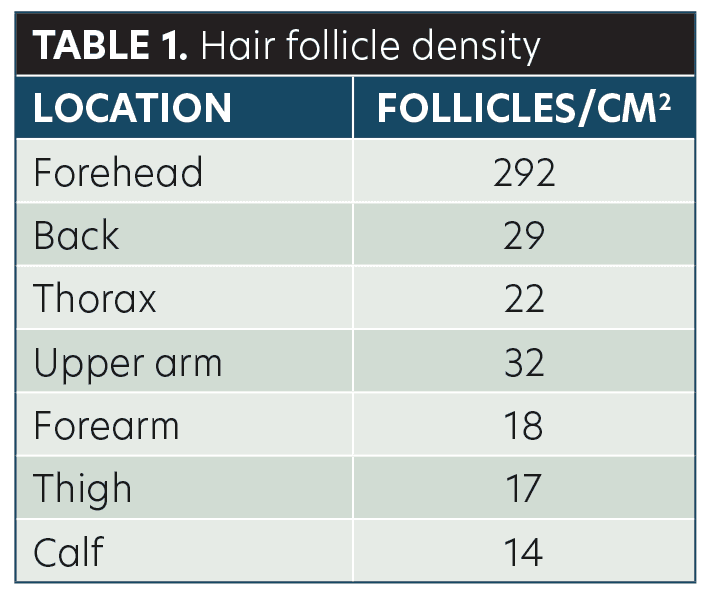
Two criteria help determine the rapidity of repigmentation within a vitiligo patch: 1) exposure to ultraviolet (UV) radiation and 2) density of hair follicles. One study by Otberg et al8 looked at hair follicle density on varying body regions (Table 1). Taking into account both UV exposure and hair follicle density, we can expect the forehead to repigment much faster than the back, which has significantly less hair follicle density and UV exposure.
Myth 7: Culture has no impact on a patient’s vitiligo.
In India, where the prevalence of vitiligo is estimated to be 0.25 to 2.5 percent,9 the social implications of the disease are often lifelong. There, it is believed that having vitiligo is a curse from God or a punishment for past sins.10 In a culture where arranged marriages are common practice, patients reported having vitiligo as a significant barrier to finding a life partner.11 Another study looking at vitiligo in the Arab population found that 84 percent believed their disease was due to fate. Additionally, 28 percent of patients in the same study believed evil eye was a cause of their illness.12 In Nigeria, vitiligo is commonly confused with leprosy and thus leads to a high level of social stigmatization.13 When evaluating patients with vitiligo, it’s important to understand how the disease has far reaching impacts on the patient’s quality of life.
Other considerations
Skin color is often a way that patients identify with their respective ethnic group/race. When areas of deeply pigmented skin become depigmented, patients can feel as though they are losing their identity. Understanding this may help clinicians better empathize with their patients. I should also mention that not all patients want to treat their vitiligo; some have embraced it while others have given up out of frustration. Don’t make assumptions on whether a patient is interested in treatment—just ask them.
References
- Alikhan A, Felsten LM, Daly M, Petronic-Rosic V. Vitiligo: a comprehensive overview Part I. Introduction, epidemiology, quality of life, diagnosis, differential diagnosis, associations, histopathology, etiology, and work-up. J Am Acad Dermatol. 2011;65 (3):473–91.
- Sehgal VN, Srivastava G. Vitiligo: compendium of clinico-epidemiological features. Indian J Dermatol Venereol Leprol. 2007;73(3):149–56.
- Vernwal D. A study of anxiety and depression in vitiligo patients: new challenges to treat. Eur Psychiatry. 2017;41(S1):S321–S321.
- Kussainova A, Kassym L, Akhmetova A, et al. Vitiligo and anxiety: a systematic review and meta-analysis. PLoS One. 2020;15(11):e0241445.
- Al-Harbi M. Prevalence of depression in vitiligo patients. Skinmed. 2013;11(6):
327–330. - Ezzedine K, Grimes PE, Meurant JM, et al. Living with vitiligo: results from a national survey indicate differences between skin phototypes. Br J Dermatol. 2015;173(2):607–609.
- Falabella R. Vitiligo and the melanocyte reservoir. Indian J Dermatol. 2009;54(4):313–318.
- Otberg N, Richter H, Schaefer H, et al. Variations of hair follicle size and distribution in different body sites. J Invest Dermatol. 2004;122(1()14–19.
- Shajil EM, Agarwal D, Vagadia K, et al. Vitiligo: clinical profiles in Vadodara, Gujrat. Indian J Dermatol. 2006;51:100–104.
- Pahwa P, Mehta M, Khaitan BK, et al. The psychosocial impact of vitiligo in Indian patients. Indian J Dermatol Venereol Leprol. 2013;79(5):679–685.
- Pandve HT. Vitiligo: is it just a dermatological disorder?. Indian J Dermatol. 2008;53(1):40–41.
- Al Ghamdi KM. Beliefs and perceptions of Arab vitiligo patients regarding their condition. Int J Dermatol. 2010;49(10):1141–1145.
- Onunu AN, Kubeyinje EP. Vitiligo in the Nigerian African: a study of 351 patients in Benin City, Nigeria. Int J Dermatol. 2003;42(10):800–802.
