 by Brian Tian, MBBS, MRCS, Dip Derm
by Brian Tian, MBBS, MRCS, Dip Derm
Dr. Tian is with Singapore General Hospital in Singapore.
J Clin Aesthet Dermatol. 2017;10(7):40–42
Funding: No funding was provided for this study.
Disclosures: The author has no conflicts of interest relevant to the content of this article.
Keywords: Laser toning, laser facial, depigmentation, leucoderma punctata, Q-switched 1,064 nm Nd:YAG, laser, non-ablative; skin rejuvenation; melasma
Abstract: In recent years, laser toning or laser facial to treat melasma has become increasingly popular in Asia. It is common to see patients undergoing lasers three times a week, or even daily. This is part of a growing trend and is sometimes recommended in the user manuals from laser manufacturers. In our study, we report on 23 Chinese patients who had lasers performed three times a week for two consecutive months, followed by rest. All 23 of them developed bilateral confetti-like hypopigmentation at the end of two months. During the four-month follow-up and rest, 10 patients were lost to follow-up. Of the remaining 13 patients, none of them had repigmentation. We conclude that frequent laser facials or laser toning at regular intervals may result in undesirable outcomes and thus should not be performed in regular intervals.
Introduction
In recent years, laser toning, or laser facial, has become increasingly popular for the treatment of melasma in Asian countries.[1,2] Laser toning involves the use of a large spot size, low fluence Q-switched (QS) Nd:YAG laser. During each session, the laser is passed multiple times over the areas of concern until a clinical endpoint is reached. This endpoint ranges from mild erythema to petechiae. Each session is then repeated frequently. This varies from daily, weekly, every other week, to monthly. Typically, once the melasma has cleared up to a satisfactory level, the frequency is reduced for the purpose of maintenance. In Asia, we’ve seen a trend for more aggressive and frequent treatment. In recent years, laser toning, or laser facial, has become increasingly popular for the treatment of melasma in Asian countries.[1,2] Laser toning involves the use of a large spot size, low fluence Q-switched (QS) Nd:YAG laser. During each session, the laser is passed multiple times over the areas of concern until a clinical endpoint is reached. This endpoint ranges from mild erythema to petechiae. Each session is then repeated frequently. This varies from daily, weekly, every other week, to monthly. Typically, once the melasma has cleared up to a satisfactory level, the frequency is reduced for the purpose of maintenance. In Asia, we’ve seen a trend for more aggressive and frequent treatment.
While the efficacy of lasers for melasma has only been documented in a few published reports,[2–4] there are multiple reports on complications, including the development of hypopigmentation and depigmentation.[2,5,6] In our center, we have performed close to 30,000 laser procedures to date. From our internal audits, we found the optimum frequency of treatment to be every two weeks (unpublished data). However, it is common practice outside of our clinic, and at times recommended by laser manufucturers, to perform laser treatments up to three times per week. To elucidate if such practices were safe and effective, we performed a retrospective analysis of patients who had undergone three laser toning sessions a week.
We report herein a retrospective analysis of 23 patients who had undergone low fluence laser toning with the 1064nm QS Nd:YAG three times a week for two consecutive months in which all of the patients developed confetti hypopigmentation bilaterally.
Methods and Materials
We reviewed the records of 23 patients who had undergone laser toning three times a week for two consecutive months during the period of January 2015 to June 2015. As per our clinic protocol, baseline photographs were taken pre-treatment and monthly to track progress. These patients were all female with ages ranging from 32 to 51 years old. They all had Fitzpatrick skin type III with bilateral malar or centrofacial pattern of melasma. They were otherwise in good health with no other concomitant laser or topical therapies during the past one year.
We treated each patient using the 1064nm Q-switched Nd YAG laser (Tri-beam, Jeisys, Seoul, Korea) with fluence of 2.0J/cm2, spot size 10mm, 12 Hertz. Each session of treatment consisted of a single full face pass and multiple repeat passes over the melasma until mild erythema was seen. There was no anesthesia involved. Cooling of the skin with a cryogen spray was performed during the procedure. This was repeated three times a week for two consecutive months.
The patients were followed for a total of six months, including the two months of laser therapy. They went without further treatment for the remaining four months. The patients and their respective photographs were examined by an independent dermatologist. Patients were also administered self-evaluation questionnaires pre-laser therapy and six months post-laser therapy.
All patients gave informed consent, and the study was conducted in accordance to the principles of Helsinki.
Results
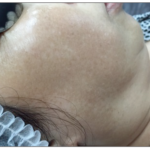
All 23 patients developed clinically visible, mottled hypopigmentation at the end of the two month period (Figure 1). Clinically, all 23 patients had lightening of the melasma patches when photographs were compared. This was also in agreement with the patients’ opinions. However, the overall patient satisfaction was poor despite the improvement in the existing melasma. All patients felt that with the mottling, they looked worse than before.
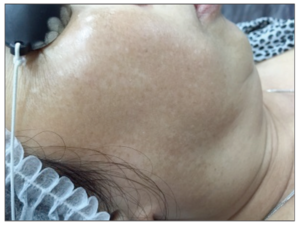
The extensiveness and the morphology of depigmentation were variable among patients— some having just a few white spots over localized areas and others having more confluent white patches over their cheeks, forehead, and chin.
After the two months of laser facial treatment, the patients were advised to rest for another four months to observe for repigmentation. Ten patients were lost to follow-up. Of the 13 remaining patients, none of them showed repigmentation. The hypopigmentation remained stable in morphology and size throughout.
Discussion
Over the last few years, laser facials, or laser toning, has become increasingly popular in Asia. The most common indications for treatment are nonablative skin rejuvenation or melasma. This technique is reported to produce clinically significant results that are delivered in safe, affordable, tolerable doses with no downtime.[5] As laser treatment is used at sub-therapeutic fluences, we’ve seen a demand by physicians and patients for greater frequency of treatment to hasten the results. At our center, we strongly recommend laser facials no more than every two weeks. We have found at our clinic that laser facials performed three times a week at regular intervals carries the risk of hypopigmentation. Other possible side effects, though not seen in our study group of 23 women, include herpes outbreak, burns, blisters, and post-inflammatory hyperpigmentation.[2,6–16]
The mechanism by which the QS Nd YAG laser causes hypopigmentation is not known. Parallels have been drawn to “punctate leukoderma,” which is seen in vitiligo.[17–19] The clinical appearance can be similar. The areas of hypopigmentation are round or oval and confetti-like. Histological studies show that there is patchy loss of melanin pigment in basal keratinocytes and decreased number of functional melanocytes and melanin granules.[17–20] The widely accepted theory is that cumulative phototoxic damage to melanocytes give rise to the hypopigmentation.[7,20]
The treatment of the laser-induced hypopigmentation is not a well-studied topic. Polnikorn[2] demonstrated that the hypopigmentation is reversible after laser treatment is terminated, although, this is not always the case. It is reported[21] that most of these areas of hypopigmenation are irreversible, as seen in our patient sample.
Conclusion
To the best of our knowledge, our study is the first to actively report on the utility of frequent laser toning and the resulting complication of melasma. Unfortunately, this practice is not well researched but is still a common practice in Asia. We acknowledge that our study is limited for a number of reasons, including the small number of study subjects and limited follow-up time. Propsective, large-scale studies that examine various treatment intervals and have longer follow-up periods are needed before definite conclusions can be drawn. However, based on our experience and the results of our study, frequent laser toning (more than every 2 weeks) should be avoided, as it may produce undesirable results, such as melasma.
References
- Mun JY, Jeong SY, Kim JH, Han SS, Kim IH. A low fluence Q-switched Nd:YAG laser modifies the 3D structure of melanocyte and ultrastruc- ture of melanosome by subcellular-selective photothermolysis. J Electron Microsc. 2011;60:11–18.
- Polnikorn N. Treatment of refractory dermal melasma with the MedLite C6 Q-switched Nd:YAG laser: Two case reports. J Cosmet Laser Ther. 2008;10(3):167–173.3.
- Berlin AL, Dudelzak J, Hussain M, Phelps R, Goldberg DJ. Evaluation of clinical, microscopic, and ultrastructural changes after treatment with a novel Q-switched Nd:YAG laser. J Cosmet Laser Ther. 2008;10(2):76–79.4.
- Lee MC, Hu S, Chen MC, Shih YC, Huang YL, Lee SH. Skin rejuvenation with 1,064-nm Q-switched Nd:YAG laser in Asian patients. Dermatol Surg. 2009;35(6):929–932.5. Won KW, Lee SH, Lee MH, et al. A prospective, split-face, double-blinded, randomized study of the efficacy and safety of afractional 1064-nm Q-sqitched Nd:YAG laser for photoaging-associated mottled pigmentation in Asian skin. J Cosmet Laser Ther. 2016;18(7):381-386. Epub 2016 Jul 19.6.
- Chan HH, Yang CH, Leung JC, Wei WI, Lai KN. An animal study of the effects on p16 and PCNA expression of repeated treatment with high-energy laser and intense pulsed light exposure. Lasers Surg Med. 2007;39(1):8–137.
- Kim MJ, Kim JS, Cho SB. Punctate leucoderma after melasma treatment using 1064-nm Q-switched Nd:YAG laser with low pulse energy.
- J Eur Acad Dermatol Venereol. 2009;23(8):960–962.8. Manaloto RM, Alster T. Erbium:YAG laser resurfacing for refractory melasma. Dermatol Surg. 1999;25(2):121–123.9.
- Nouri K, Bowes L, Chartier T, Romagosa R, Spencer J. Combination treatment of melasma with pulsed CO2 laser followed by Q-switched alexandrite laser: A pilot study. Dermatol Surg. 1999;25(6):494–497.10.
- Angsuwarangsee S, Polnikorn N. Combined ultrapulse CO2 laser and Q-switched alexandrite laser compared with Q- switched alexandrite laser alone for refractory melasma: Split-face design. Dermatol Surg. 2003;29(1):59–64.11.
- Wang CC, Hui CY, Sue YM, Wong WR, Hong HS. Intense pulsed light for the treatment of refractory melasma in Asian persons. Dermatol Surg. 2004;30(9):1196–1200.12.
- Negishi K, Kushikata N, Tezuka Y, Takeuchi K, Miyamoto E, Wakamatsu S. Study of the incidence and nature of ‘‘very subtle epidermal melasma’’ in relation to intense pulsed light treatment. Dermatol Surg. 2004;30(6):881–886, discussion 886.13.
- Rokhsar CK, Fitzpatrick RE. The treatment of melasma with fractional photothermolysis: A pilot study. Dermatol Surg. 2005;31(12):1645–1650.14. Li YH, Chen JZ, Wei HC, et al. Efficacy and safety of intense pulsed light in treatment of melasma in Chinese patients. Dermatol Surg. 2008;34(5):693–700, discussion 700–691.15. Lee HS, Won CH, Lee DH, et al.
- Treatment of melasma in Asian skin using a fractional 1,550-nm laser: An open clinical study. Dermatol Surg. 2009;35(10):1499–1504. 16. Kang WH, Yoon KH, Lee ES, et al. Melasma: Histopathological characteristics in 56 Korean patients. Br J Dermatol. 2002;146(2):228–237.17. Dogra S, Jain R, Parsad D, Handa S. Leukoderma punctatum following systemic PUVA therapy. Int J Dermatol. 2002;41(12):922–923.18.
- Park JH, Lee MH. Case of leukoderma punctata after topical PUVA treatment. Int J Dermatol. 2004;43(2):138–139.19.
- Falabella R, Escobar CE, Carrascal E, Arroyave JA. Leuko-derma punctata. J Am Acad Dermatol. 1988;18(3):485–494.20.
- Bhatnagar A, Kanwar AJ, Parsad D, Narang T, De D. Confetti-like hypopigmentation: A rare complication of common phototherapeutic modality. J Eur Acad Dermatol Venereol. 2007;21(9):1276–1277.21.
- Chan NP, Ho SG, Shek SY, Yeung CK, Chan HH. A case series of facial depigmentation associated with low fluence Q-swithced 1,064nm Nd:YAG laser for skin rejuvenation and melasma. Lasers Surg Med. 2010;42(8):712–719.

