
by Graciela Araújo do Espírito-Santo; Diniz Pereira Leite Jr; Hugo Dias Hoffmann-Santos; Luciana Basili Dias; and Rosane Christine Hahn
Drs. Espírito-Santo, Leite, Hoffmann-Santos, Dias, and Hahn are with the Faculty of Medicine, Post Graduate in Health Sciences at the Federal University of Mato Grosso, Cuiabá, Mato Grosso, Brazil. Drs. Leite and Hahn are with Specialized Medical Mycology Center, Federal University of Mato Grosso, Cuiabá, Mato Grosso, Brazil. Drs. Leite and Hoffmann-Santos are with University Center of Varzea Grande, Várzea Grande, Mato Grosso, Brazil.
J Clin Aesthet Dermatol. 2017;10(8):56–61
Funding: Financial support for this study was provided by FAPEMAT – Fundação de Amparo à Pesquisa no Estado de Mato Grosso (Foundation for the Support of Science of the State of Mato Grosso).
Disclosures: The authors have no conflicts of interest relevant to the content of this article.
Keywords: Onychomycosis, toenails, 1340nm Nd:YAP laser, monotherapy
Abstract: Onychomycosis is an infection of the nail plate by fungal microorganisms. This infection has an important social impact on women and men and poses a major challenge for its treatment. The traditional treatment of onychomycosis involves the use of topical and oral antifungal agents. However, the presence of adverse effects frequently associated with oral antifungals, their high cost, and their potential interactions with other drugs reflect some of the problems associated with conventional therapy. The current report details the evaluation of a 1340nm laser as monotherapy for toenails affected by onychomycosis. A 1340nm, neodymium-yttrium:yttrium-aluminum-perovskite (Nd:YAP) (e) laser (Etherea, Industra Technologies, Brazil) was used with the following treatment parameters: a spot size of 6mm, pulse duration of 5ms, fluence of 22 to 25J/cm², and repetition rate of 1.5 to 2.5Hz. In all, 72 toenails were evaluated in 30 patients who had clinical and laboratory confirmation of onychomycosis. The efficacy of treatment was measured by the degree of patient satisfaction on a scale of 0 to 10 and by mycological cure evidenced by direct mycological exam and culture. Considering three applications of laser therapy and a clinical/laboratory follow-up period of 12 weeks, monotherapy with 1340nm laser was not effective, since 93.3 percent of the assessed patients remained without clinical and mycological cure. Despite reports of variable success rates with the use of different lasers for the treatment of onychomycosis, it is not yet possible to state that this therapeutic alternative is indicated for the treatment of these infections, mainly due to the limited number of patients and/or nail plates evaluated and the controversial results described in the literature.
Introduction
Onychomycoses are fungal infections that are extremely prevalent in the world population and may reach infection rates of up to 24 percent in the elderly.[1] Due to the high adaptation of fungal microorganisms to keratinized nail tissue, the persistence of fungal spores in nail tissues leads to frequent recurrences.2 Unfortunately, the application of topical drugs is not effective, and the use of oral antifungals presents a series of undesirable adverse effects, in addition to their high cost.[3] For these reasons, laser therapy, a novel, alternative option, might be considered, especially for pregnant patients and patients with pre-existing diseases.Onychomycoses are fungal infections that are extremely prevalent in the world population and may reach infection rates of up to 24 percent in the elderly.[1] Due to the high adaptation of fungal microorganisms to keratinized nail tissue, the persistence of fungal spores in nail tissues leads to frequent recurrences.[2] Unfortunately, the application of topical drugs is not effective, and the use of oral antifungals presents a series of undesirable adverse effects, in addition to their high cost.[3] For these reasons, laser therapy, a novel, alternative option, might be considered, especially for pregnant patients and patients with pre-existing diseases.
In 2010, the United States Food and Drug Administration (FDA) approved different laser systems for clearing the nail plate.[4] It is important to emphasize that as a criterion for the cure of onychomycosis, mycological exam results should be negative after the laser sessions and at the time of clinical and laboratory follow-up. Therefore, the clinical improvement or clearing of the nail plate alone would not be satisfactory to define the cure of the clinical presentations previously diagnosed as onychomycosis. However, due to the minimal invasive nature of the procedure, the low number of sessions recommended for treatment, and the possibility of clearing the nail plate, the use of laser therapy currently has been considered an alternative for the treatment of onychomycosis, at the expense of conventional treatment based on antifungal drugs.
This study evaluated the efficacy of 1340nm neodymium-yttrium:yttrium-aluminum-perovskite (Nd:YAP) laser therapy performed in three sessions at three-week intervals for treating onychomycosis, as measured by patient satisfaction and mycological tests three months after the last session.
Patients and Methods
Inclusion criteria. Inclusion criteria were presentation of clinical findings consistent with onychomycosis in the toenails, a direct mycological examination, positive culture for fungi, and the absence of prior treatment with antifungal therapy within three months.
Exclusion criteria. Exclusion criteria were pregnancy, age younger than 15 years, the use of anticoagulants and antifungals, and the presence of onychomycosis caused by yeasts, fingernail onychomycosis, psoriasis, lichen planus, hematomas, and other nail pathologies.
Study design. This was an analytical cross-sectional study performed between December 2014 and September 2015 at the dermatology outpatient clinic of the Julio Muller University Hospital, Federal University of Mato Grosso, Cuiabá, in the Midwest region of Brazil. It was approved by the research ethics committee under number 888.913/2014 – Brazil platform.
Patient evaluation. Demographic data were retrieved from each patient participating in the study and included the following: sex, age, occupational activity, underlying diseases, and time of progression of onychomycosis. The clinical classification was subdivided as follows: total dystrophic onychomycosis (TDO), superficial white onychomycosis (SWO), distal lateral subungual onychomycosis (DLSO), and proximal subungual onychomycosis (PSO).
Nail samples and fungal culture. Nail fragments 1 to 2mm in size or subungual deposits were collected from the nail plates with clinical suspicion of onychomycosis. A direct mycological examination was performed (40% potassium hydroxide preparation [KOH]), and fungal structures such as arthrospores and hyphae were considered as conferring positivity in the direct examination. Sabouraud’s dextrose agar (DIFCO™) containing chloramphenicol (100mg/mL) and mycobiotic agar were used as media for the fungal cultures. Cultures were incubated at 28?C for three weeks until fungal colonies developed.
Cure criteria. The term complete cure reflected two aspects: significant clinical improvement and negative mycological exams. The clinical improvement of the nail plate was considered based on either the clearing of the nail plate or a decrease in the area affected by the fungal disease.
Results
Clinical onychomycosis type. In the 72 nail plates assessed, the distal subungual form was observed in 73.6 percent and the total dystrophic form in 26.4 percent of cases. The involvement of the plates was classified by the area of change: 41.7 percent of the slides showed involvement of two-thirds of the area, while 34.7 percent showed full involvement.
Fungus type. Dermatophytes were observed in 90.3 percent and nondermatophytes in 9.7 percent of the assessed cases (30 patients). Of the 72 nail plates, the species were identified in the clinical samples from 41 of the nail plates. Trichophyton rubrum was observed in 65.8 percent of the clinical samples, while T. mentagrophytes and Fusarium species were each observed in 17.1 percent of the clinical samples.
Patient demographic data. Thirty patients, 23 women and seven men, were selected and presented with involvement of 72 nail plates. The group had an average age of 53.2 years (confidence interval [CI]=95%, 49.2–57.1). The patients were queried about their work activities: 23.3 percent were housewives/husbands exclusively, 16.7 percent were retired, and 16.7 percent were sellers. The average time of progression of the disease was 7.5 years (CI=4.1–10.9). The patients had the following associated diseases: systemic arterial hypertension (50%), Type 2 diabetes mellitus (14.8%), arthritis (7.14%), hypothyroidism (7.14%), and hypercholesterolemia (7.14%). Nine patients reported prior treatment with fluconazole, and two with amorolfine nail lacquer.
Mycologic cure of nail fungal infections. The patients returned 12 weeks after the last laser session for the clinical assessment and collection of control test results. The mycological tests showed persistence of infection by fungi in 66 nail plates (91.7%) and absence of infection in six nail plates. Of those cured, none were dystrophic forms. The involvement of the nail plate was classified in area of change: 41.7 percent of the nail plates presented involvement of two-thirds of the area, and 34.7 percent were fully affected.
Adverse events. At the end of the laser sessions, patients reported a score for the sensation of pain, which could be 0 (painless), 1 (mild), 2 (moderate), 3 (severe), and 4 (unbearable). No patient classified the pain as intolerable, but the majority classified the pain as either mild or moderate.
Discussion
Many factors contribute to therapeutic failure in onychomycosis. These include high fungal adaptation to the keratinized tissue and chronic characteristic of the fungal infection, causing aesthetic discomfort alone in most of the cases, without other damage to the patients. In addition to the high cost of available antifungals, adverse effects should be taken into account, especially in patients with associated diseases who receive other medications that may interact with the antifungal agents. For these reasons, laser therapy has emerged as a potential novel option.
Currently, the studies conducted have employed different types of lasers (crystals, gases, and semiconductors) with regard to wavelengths and varied pulse duration (milliseconds, microseconds, and nanoseconds). Each published study evaluated one brand of laser with its properties; therefore, there is no standardized method of treatment defined for the use of laser in epilation or for vascular lesions.
In general, few studies on laser therapy for the treatment of onychomycosis validate this alternative as monotherapy. This is due to the small number of patients evaluated, the scarcity of randomized trials,[5–7] and the variable periods used for the clinical and laboratory monitoring of patients who received laser therapy.
In this study, onychomycosis was more prevalent in women, who reported aesthetic discomfort on the appearance of the nails during the laser sessions. The majority of patients were between 40 and 60 years of age, with a mean age of 53.2 years. In 2000, Ghannoum[8] described a similar adult population. The same author reported a higher prevalence of onychomycosis in patients with perfusion alterations such as diabetes, hypertension, and arteriosclerosis. The data obtained in the present study were in agreement, as 50 percent of the patients had hypertension, 14.3 percent had diabetes mellitus, and 7.1 percent had hypercholesterolemia.
In relation to work activities, the majority of published studies make no mention of this variable with the exception of one study carried out in India by Gupta et al[9] in 2007, in which the authors related the predominance of clinical presentation of onychomycosis to rural workers. This can be associated with the poor hygiene habits of these individuals and with greater contact with the soil. In the group of patients assessed in the present study, 23.3 percent were housewives/husbands and an additional 30.1 percent were retired people (16.7%), cooks (6.7%), and janitors (6.7%). This group of workers has regular activities that entail the use of water and cleaning products, as reported by Elewski et al.[10]
The distal subungual clinical form of onychomycosis was more frequent in the group evaluated in this study, which is in agreement with other published studies. This form occurs due to the easier access of the fungus to the free edge of the nail plate. It was also observed that the dystrophic form showed no case of cure with laser treatment. The dystrophic form presents a thickening of the nail plate. The presence of dermatophytoses is very common in this form, representing the aggregation of fungal agents and conferring the worse form of prognosis with traditional treatments.[11]
The dermatophyte T. rubrum is the most frequent causative agent in onychomycosis in toenails,[4,12] having also been the most isolated fungus in the group of patients assessed in this study, followed by T. mentagrophytes and Fusarium spp. Some authors consider that the production of xanthomegnin by the dermatophyte fungi[13] would act as a target for the laser,[14] in accordance with the theory of selective photothermolysis.[15] The choice of toes as the anatomic site assessed in this study and others rather than fingernails was made by taking into account the fact that yeast can be isolated in the fingers and can represent only contaminant agents.
In a total of 15 published studies (Table 1), different authors investigated the use of the 1064nm laser (Nd:YAG) either as a single intervention, as a combination of 1064nm/532nm, or in comparison with another laser. In all of these studies, the authors stated that only the toenails were evaluated, exactly as performed in this study. Only one report used an 870/930nm laser and another used a CO2 laser as a strategy for penetration of topical antifungal in nail plates. This series of studies was compiled in a very well documented review by Bristow[16] in 2014. In general, the review included both case studies and comparative studies, but there was a randomized study Landsman et al[17] that included 36 patients with proven onychomycosis. In addition, Hollmig et al[5] also conducted a randomized study, which evaluated 27 patients and 125 nail plates. Li et al[6] in 2014 compared the use of the 1064nm Nd:YAG laser with itraconazole and observed better results at Weeks 8 and 16 in the group using itraconazole.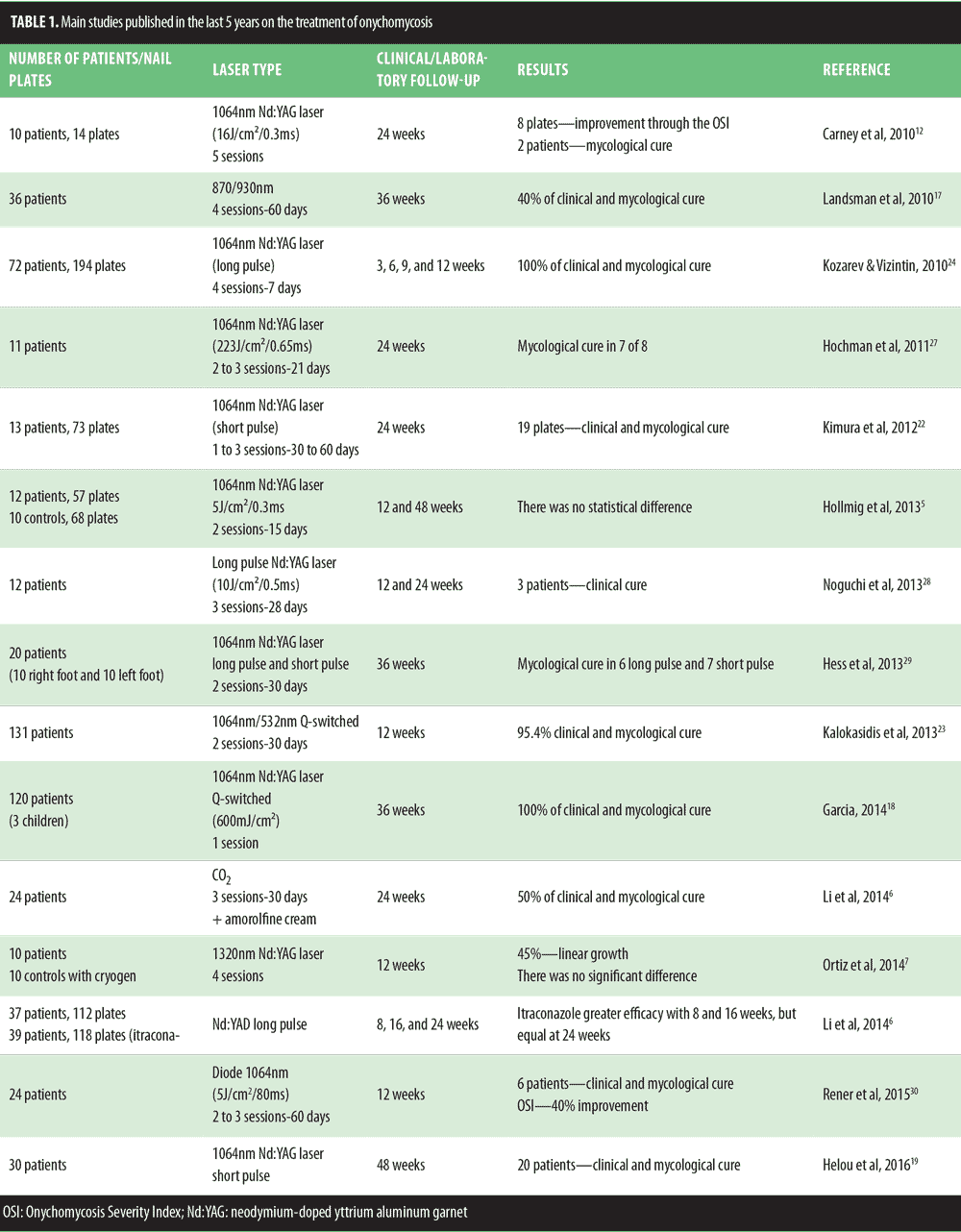
However, equal results were observed at the 24th week of follow-up. Notably, in the last five years, only three randomized studies were conducted.[6,18,19] In 2014, Garcia[18] in Mexico evaluated a group of 100 patients, including three children, with onychomycosis, and clinical and mycological cure was observed in 100 percent of cases. More recently, Helou et al[19] showed clinical and mycological cure in 20 of 30 patients treated with short pulse Nd:YAG laser.
In general, all studies reported in the last five years have included a very limited number of patients, ranging in number from 8 to 131. Among the diagnostic criteria used, the fungal culture tests and direct mycological tests were more common, followed by periodic acid-Schiff (PAS) stain and culture polymerase chain reaction. Weinberg et al20 evaluated 94 samples of the nail plate and suggested the following technique sensitivities: KOH (80%), PAS stain (92%), and culture (59%). As a methodological strategy, the number of patients included in this study (n=30) was within the average adopted by different researchers. In the 15 studies published in the last five years, Weinberg et al[20] placed seventh in total number of study subjects, surpassed by Zhang et al[21] (n=33), Kimura et al[22] (n=31), Kalokasidis et al[23] (n=131), Kosarev and Vizintin[24] (n=72), Li et al[6] (n=76), and Garcia[18] (n=120).
Surprisingly, the results reported by Kalokasidis et al[23] showed a high cure rate (95.4%), corroborated by the negative results of the direct mycological tests and culture for fungi. This cure rate was far superior to the rates reported in other studies. The laser used was the Q-switched Nd YAG 1064nm/532nm, with patients undergoing two treatments with an interval of 30 days. The results obtained suggest that the distal subungual and white superficial onychomycosis types are more susceptible to this modality, while the dystrophic clinical type is less susceptible. In our study, there was a predominance of the distal subungual clinical form (53 of a total of 72 nail plates evaluated). However, the use of the 1340nm laser did not present a high cure rate, considering the 30 patients cured.
In general, there is no consensus on the efficacy of laser therapy for the treatment of onychomycosis, despite the methodological differences observed in the studies published on the subject. This lack of consensus can be justified by the lack of standardization regarding the types of studies, the numbers of patients evaluated, the number of nail plates included, and the types of fungi isolated. The majority of the research suggests that the elderly have the highest prevalence of onychomycosis.
The visual appearance of the nail plates, reflecting a clinical improvement in some studies published in the last five years as well as in our study, was based on the levels of satisfaction of the patients assessed. However, the frequent use of the Onychomycosis Severity Index (OSI), which is an instrument that grades the surface of affected nails, has been observed in the literature. It is important to emphasize that an actual “cure” requires some skepticism on the part of the physician, even if a clinical improvement of onychomycosis is observed.In general, when taking into account the duration of the studies carried out, from 12 weeks up to 36 weeks, it is important to stress that the growth rate of the nail plate is approximately 1mm/month. However, in the elderly, the growth rate decreases by 0.5 percent. Recently, an exception regarding the study duration was verified in the study published by Hollmig et al[5] in 2014, because this group of researchers held laboratory clinical follow-up of the patients evaluated for 12 months. This is the longest recorded period in the literature regarding the use of laser therapy for the treatment of onychomycosis.
The information published by Yan et al[25] in 2004 regarding the slower growth of the nail plate infected by dermatophytes should be highlighted. T. rubrum was the most isolated fungus in this study, and the period of patient follow-up (3 months) can be considered relatively narrow for the growth of the nail plate. Thus, a longer clinical and laboratory follow-up may be useful to assess the effectiveness of laser therapy in onychomycosis.
In this context, findings published by Hollmig et al[5] in 2014 show that although there was an improvement in the appearance of the nail plates of the group assessed in the study at three months, this improvement was not confirmed in a longer period (12 months), suggesting temporary clinical improvement. With these observations in mind, one must recall the possibility of relapses, which are very frequent in onychomycosis. Relapses are defined as the recurrence of fungal infections on the nail plate with insufficient clearing. In contrast, reinfections are attributed to new infections, which can appear in the nail plates that were previously cleared of infections.[16] The type of onychomycosis is an important factor that can contribute to the success of the chosen treatment.[26] Thus, the types classifiable as distal lateral subungual and proximal white subungual are those with better response to the laser treatments. Some published studies do not mention the clinical classification of onychomycosis, as opposed to this study.[5,21,27]
Conclusion
Due to the use of different methods and types of lasers used in the published literature, it is not yet possible to conclude that laser therapy is effective as a monotherapy for treatment of onychomycosis. Further studies should be conducted, including classification of the type of onychomycosis, clinical and laboratory follow-up over longer periods, and comparison of the groups treated with conventional therapy. Randomized and comparative studies may provide more reliable results.Taking into account the current state of the art and the relevant literature published to date, the clinical presentation of onychomycosis remains a major challenge in terms of the treatment and eradication of the fungal agent involved.
References
- Anane S, Chtourou O, Chedi A, et al. Onychomycosis in the elderly. Ann Dermatol Venerereol. 2007;39:746–753.
- Scher RK, Tavakkol A, Sigurgeirsson B, et al. Onychomychosis: diagnosis and definition of cure. J Am Acad Dermatol. 2007;56:939–944.
- Debruyne D, Coquetel A. Pharmacokinetics of antifungal agents in onychomycoses. Clin Pharmacokinet. 2001;40(6):441–472.
- Gupta AK, Simpson FC. Medical devices for the treatment of onychomychosis. Dermatologic Therapy. 2012;25:574–581.
- Hollmig ST, Rahman Z, Henderson MT, et al. Lack of efficacy with 1064-nm neodymium:yttrium-aluminum-garnet laser for the treatment of onychomycosis: a randomized, controlled trial. J Am Acad Dermatol. 2014;70(5):911–917.
- Li ME, Kim H, Park Y, et al. Toenail onychomycosis treated with a fractional carbon-dioxide laser and topical antifungal cream. J Am Acad Dermatol. 2014;70(5):918–923.
- Ortiz AE, Truong S, Serowka K, Kelly C. A 1320 nm Nd: YAG for improving the appearance of onychomycosis. Dermatologic Surgery. 2014;40:1356–1360.
- Ghannoum MA, Hajjeh RA, Scher R, et al. Large-scale North American study of fungal isolates from nails: the frequency of onychomycosis, fungal distribution, and antifungal susceptibility patterns. J Am Acad Dermatol. 2000;43(4):641–648.
- Gupta M, Sharma NL, Kanga NL, et al. Onychomycosis: clinico-mycologic study of 130 patients from Himachal Pradesh, India. India J Dermatol Venerol and Leprol. 2007;73(6):389–392.
- Elewski MB, Rich P, Tosti AP, et al. Onchomycosis: an overview. Journal of Drugs Dermatology. 2013;12(2):96–103.
- Grover C, Khurana A. An update on treatment of onychomycosis. Mycoses. 2012;55(6):541–551.
- Carney C, Cantrell W, Warner J, Elewski B. Treatment of onychomycosis using a submillisecond 1064nm neodymium: aluminum garnet laser. J Am Acad Dermatolol. 2013;69(4):578–582.
- Gupta AK, Ahmad I, Borst I, Summerbell R. Detection of xantomegnin in epidermal materials infected with Trichophyton rubrum. J Invest Dermatol. 2000;18:901–905.
- Vural E, Winfield HL, Shegleton AW, et al. The effects of laser irradiation on Trychophyton rubrum growth. Lasers Med Sci. 2008;23:349–535.
- Anderson RR, Parrish JA. Selective photothermolysis: precise microsurgery by selective absorption of pulsed radiation. Science, New Series. 1983;220(4596):524–527.
- Bristow IR. The effectiveness of laser in the treatment of onychomycosis: a systematic review. Bristow Journal of Foot and Ankle Research. 2014:7–34.6.
- Landsman AS, Robins AH, Angeline PS, et al. Treatment of mind, moderate and severe onychomychosis using 870-930nm light exposure. J Am Podiatr Med Assoc. 2010;100:166–177.
- Garcia HRG. Onychomychosis: 1064nm Nd: YAG q-switch laser treatment. J Cosmetic Dermatol. 2014;13:232–235.
- Helou J, Maatouk I, Hajjar MA, Moutran R. Evolution of Nd: YAG laser device efficacy on onychomycosis: a case series of 30 patients. Mycoses. 2016;59:7–11.
- Weinberg JM, Koestenblatt EK, Tutrone WD, et al. Comparison of diagnostic methods in the evolution of onychomycosis. J Am Acad Dermatol. 2003;49:193–197.
- Zhang RN, Wang DK, Zhuo FL, et al. Long-pulse Nd:YAG 1064nm laser treatment for onychomychosis. Chin Med J. 2012;125:3288–3291.
- Kimura U, Tacheuchi K, Kinishita A, et al. Treating onychomychoses of the nail: clinical efficacy of the sub-milisecond 1064nm Nd:YAG laser using a 5mm spot diameter. J Drugs Dermatol. 2012;11:496–504.
- Kalokasidis K, Onder M, Trakatelli BR, Fritz K. The effect of Q-switched Nd:YAG 1064nm/532nm laser in the treatment of onychomycosis in vivo. Dermatology Research and Practice. 2013:1–10.
- Kozarev J, Vizintin Z. Novel laser therapy in treatment of onychomycosis. Journal of the Laser and Health Academy. 2010;1:1–8.
- Yan L, Sisi Y, Jin X, et al. Comparison of the efficacy of long-pulse Nd: YAG laser intervention for treatment of onychomicosis of toenail of fingernails. Journal of Drugs in Dermatology. 2014;13:1258–1263.
- Bhatta AK, Huang X, Keyal U, Zhao JJ. Laser treatment for onychomychosis: a review. Mycoses. 2014;57:734–740.
- Hochman LG. Laser treatment of onychomicosis using a novel 0, 65 – millisecond pulsed Nd:YAG 1064nm laser. Journal of Cosmetic and Laser Therapy. 2011;13:2–5.
- Noguchi H, Miyata K, Sugita T, et al. Treatment of onychomycosis using a 1064nm Nd:YAG laser. Med Micol J. 2013;54:333–339.
- Hess H, Jager MW, Raulin C. Treatment of onychomycosis using the 1064nm Nd:YAG laser: a clinical pilot study. JDDG. 2013. DOI: 10.1111/ddg.12292.
- Renner R, Gruber K, Sticherling M. 1,064-nm diode laser therapy of onychomycosis: results of a prospective open treatment of 82 toenails. Dermatology. 2015;230:128–134.

